Continuing Education Activity
The management of infectious colitis is complex, and new approaches have been introduced. The basic and clinical aspects of infectious colitis must be clearly defined to achieve satisfactory outcomes. This activity reviews infectious colitis, and focusses on the etiology, epidemiology, pathophysiology, evaluation, management, and complications of infectious colitis, and highlights the role of the interprofessional team in improving healthcare outcomes.
Objectives:
- Identify the etiology and along with accompanying risk factors for infectious colitis.
- Describe the pathophysiology in infectious colitis.
- Summarize the evaluation process infectious colitis.
- Review the management options available for infectious colitis.
Introduction
Colonic infection by bacteria, viruses, or parasites results in an inflammatory-type of diarrhea and accounts for the majority of cases presenting with acute diarrhea. These patients present with purulent, bloody, and mucoid loose bowel motions, fever, tenesmus, and abdominal pain. Common bacteria causing bacterial colitis include Campylobacter jejuni, Salmonella, Shigella, Escherichia coli, Yersinia enterocolitica, Clostridium difficile, and Mycobacterium tuberculosis. Common causes of viral colitis include Norovirus, Rotavirus, Adenovirus, and Cytomegalovirus. Parasitic infestation, such as Entamoeba histolytica, a protozoan parasite, is capable of invading the colonic mucosa and causing colitis. Sexually transmitted infection affecting the rectum merit consideration during assessment. These diseases can occur in patients with HIV infection and men who have sex with men and may include Neisseria gonorrhoeae, Chlamydia trachomatis, Herpes simplex, and Treponema pallidum.
The patients present with rectal symptoms that mimic inflammatory bowel disease, including rectal pain, tenesmus, bloody mucoid discharge, and urgency. Detailed medical history and identification of specific associated risks are essential in establishing the diagnosis. Stool microscopy and culture and endoscopy are crucial to the diagnosis. However, stool culture helps in the diagnosis of less than 50% of patients presenting with bacterial colitis, and endoscopic examinations usually reveal non-specific pathological changes. Therefore, an approach is needed to evaluate and diagnose the cause of colitis and exclude non-infectious causes. This activity discusses current strategies to diagnose and manage infectious colitis and how to make a high index of suspicion based on clinical presentation and use investigation methods to reach a final diagnosis. This activity discusses the etiology, epidemiology, pathophysiology, clinical presentation, evaluation, differential diagnosis, complications, and management of patients with infectious colitis.
Etiology
Infectious colitis may result from infection with:
- Bacterial infections: including Campylobacter jejuni, Salmonella, Shigella, Escherichia coli (including these subgroups - enterotoxigenic E. coli, enteropathogenic E. coli, enterohemorrhagic E. coli, enteroinvasive E. coli, enteroaggregative E. coli), Yersinia enterocolitica, Clostridium difficile, and Mycobacterium tuberculosis.
- Viral infection: Norovirus, Rotavirus, Adenovirus, and Cytomegalovirus (CMV).
- Parasitic infection such as Entamoeba histolytica (causes amoebic colitis)
- Sexually transmitted infections: Particularly infections affecting the rectum in patients with HIV infection and men who have sex with men may include the following infections: Neisseria gonorrhoeae, Chlamydia trachomatis (causes lymphogranuloma venereum), Herpes simplex 1 and 2, and Treponema pallidum (causes syphilis).
Enterotoxigenic E. coli is the leading cause of traveler’s diarrhea. Enteroaggregative E. coli can cause traveler’s diarrhea, but it is not the leading cause. Enterohemorrhagic E. coli has two main serotypes E. coli O157: H7 and non-O157: H7; the natural reservoirs of both serotypes are cows. Therefore, the infection is related to the consumption of inadequately cooked beef, or contaminated milk or vegetables. They are responsible for outbreaks in developed countries.[1]
Two of these subgroups cause non-bloody diarrhea: enterotoxigenic E. coli and enteroaggregative E. coli; both produce enterotoxins that induce chloride and water secretion and inhibit their absorption. However, enterohemorrhagic E. coli (both strains E coli O157: H7 and non-O157: H7) causes bloody diarrhea and produce Shiga-like toxins, resulting in a clinical picture similar to Shigella dysenteriae infection.[2]
Both enteropathogenic E. coli and enteroinvasive E. coli do not produce toxins. Enteropathogenic E. coli is responsible for outbreaks, particularly in children less than two years of age, while enteroinvasive E. coli causes acute self-limited colitis and is responsible for outbreaks mainly in developing countries. However, the outbreaks in Nottingham, the UK, in 2004, highlight the need for its consideration as a potential pathogen in foodborne outbreaks in Europe.[3]
Children (in daycare centers), elderly (in nursing homes), and immunocompromised individuals are susceptible to these infections. The fecal-oral route, animal host, and ingestion of contaminated food and water are the usual modes of infection.
Food and water contaminations with pathogenic bacteria may cause large outbreaks of diseases.
Epidemiology
Bacterial colitis accounts for up to 47% of cases of acute diarrhea.[4] Campylobacter jejuni is the number one bacterial cause of diarrheal illness worldwide with an estimated prevalence of 25 to 30 per 100000 population. For Salmonella infection, an estimated 1.2 million annual cases of non-typhoidal salmonellosis occurred in the United States.
Shigellosis incidence worldwide reported to be approximately 165 million cases, but mortality has decreased in the last three decades because of improvement in laboratory diagnosis and treatment. In the United States, estimates are approximately 500000 cases per year, with 38 to 45 deaths.[5]
Yersinia enterocolitica colitis commonly presents in young children in the winter. In the United States, estimate are one case per 100000 individuals each year.
Clostridium difficile infection in hospitalized adults in the United States increased from 4.5 cases per 1000 discharge in 2001 to 8.2 cases in 2010 and a mortality rate of 7%.[6] Another study from the United Stated on Clostridium infection estimated 500000 cases in 2011 with 83000 recurrence and 29300 deaths.
Mycobacterium tuberculosis is the third most common site of extra-pulmonary tuberculosis, accounting for 12.8% of all cases under this category.[7] The recurrence of tuberculosis in developing countries parallels the AIDS epidemic distribution closely.[8] Other factors for increasing rates of tuberculosis in many developed countries are related to the migrant population, deterioration in social conditions, cutbacks in public health surveillance services, and increased prevalence of immune-suppressed individuals (AIDS, those receiving biological agents in diseases such as rheumatoid arthritis, and inflammatory bowel disease).[9]
Amebiasis ranks as the second leading cause of death due to protozoan infection after malaria, Chagas disease, and leishmaniasis.[10]
The prevalence of CMV infection in percent colitis is in the range of 21% to 34%.[11] CMV reactivation in patients with severe ulcerative colitis has a reported prevalence of 4.5% to 16.6% and as high as 25% in patients requiring colectomy for severe colitis.
Infectious proctitis among HIV-positive and HIV-negative men varied and in a recent study was as follows: chlamydia (23% versus 22%, respectively), gonorrhoea (13% versus 11%), HSV-1 (14% versus 6%), and HSV-2 (22% versus 12%), lymphogranuloma venereum (8% versus 0.7%), more than one infection (18% versus 9%). Approximately thirty-two percent of HSV proctitis had external anal ulcerations.[12]
Pathophysiology
Infection with Campylobacter jejuni is a result of orally ingested contaminated food or water. Several factors influence infections, including the dose of bacteria ingested, the virulence of organisms, and the immunity of the host. The median incubation period is from 2 to 4 days. C. jejuni multiplies in the bile and then invade the epithelial layers and travel to the lamina propria producing a diffuse, bloody, edematous enteritis.
Pseudomembranous colitis is caused by toxin-producing Clostridium difficile. The disease develops as a result of altered normal microflora (usually by antibiotic therapy such as cephalosporin and beta-lactam antibiotics) that enables overgrowth and colonization of the intestine by Clostridium difficile and production of its toxins.[13]
Enterotoxigenic E. coli produces heat-labile (HL) and heat-stable (ST) toxins. The HL toxins activate adenyl cyclase in enterocytes resulting in increased cAMP and stimulation of chloride secretion and inhibition of absorption. The ST toxins bind to guanylate cyclase resulting in increased cGMP and effects on cellular transporters similar to those caused by LT toxins resulting in secretory non-inflammatory diarrhea (this explains the limited histopathological changes in this infection).[14]
Enteropathogenic E. coli can produce proteins for “attaching” and “effacing” (A/E) lesions, which enable the bacteria to get tightly attached to the enterocytes apical membranes and causing effacement or loss of the microvilli. As stated earlier, enteropathogenic E. coli does not produce toxins, and their underlying mechanisms for causing diarrhea is by attaching and effacing lesions.[15]
Enterohemorrhagic E. coli; both of its serotypes E. coli O157: H7 and non-O157: H7 produce Shiga-like toxins similar to Shigella dysenteriae infection. However, E. coli O157: H7 strains are more likely to cause outbreaks compared to non-O157: H7 serotypes. They produce bloody diarrhea and are responsible for the development of hemolytic-uremic syndrome and ischemic colitis.[16]
Enteroinvasive coli do not produce toxins; they invade enterocytes and cause self-limited colitis. Exact details of their pathogenetic mechanisms are still not fully understood.
Enteroaggregative E. coli produces enterotoxins related to Shigella enterotoxins and ST toxins of enterotoxigenic E. coli. They attach themselves to enterocytes via adherence fimbriae.
Immunity to Mycobacterium tuberculosis undergoes mediation via T-cells resulting in macrophage stimulation to kill the bacteria. Reactivation of infection or re-exposure to the bacillus in a sensitized individual, as it is the case in most Mycobacterium tuberculosis colitis cases resulting in rapid defense reactions and increased tissue necrosis accompanied by loss of T-cell immunity (tuberculin test in these patients becomes negative although used to be previously positive, which is consistent with fading T-cell protection).[17]
Primary CMV infection in immunocompetent individuals is usually asymptomatic. However, in patients whose immune response is compromised, they develop symptoms in different body organs, including CMV colitis.
Research concerning genetics and molecular sciences of Entamoeba histolytica have brought new understanding about mechanisms by which the parasite impose invasive abilities and pathological lesions in the colon and extracolonic organs. Host factors predisposing to infection are also under research.[17]
Histopathology
No significant differences appear in histological biopsies taken from the rectum of patients with different bacterial infections. However, the absence of crypt architecture distortion or basal plasmacytosis helps differentiate acute infectious colitis from chronic inflammation caused by inflammatory bowel disease.
Infection with Escherichia coli O157: H7 may show changes similar to those of ischemic colitis (small atrophic crypts, hyalinized lamina propria, and fibrin thrombi).
Yersinia enterocolitica shows inflammatory changes, ulcerations in the cecum and terminal ileum areas, hyperplasia of Peyer patches, microabscesses, and granulomas. (This condition requires differentiation from Crohn disease and Mycobacterium tuberculosis involving the terminal ileum/caecum area).
Colonic histopathological changes are limited in enterotoxigenic E. coli, enteroinvasive E. coli, and enteroaggregative E. coli infections.
In Mycobacterium tuberculosis, characteristic granulomas with central caseation are present; tubercle bacilli are identifiable with acid-fast stains.[18]
The diagnosis of CMV colitis requires histological examination of biopsy tissues, taken from the ulcer edge or base. Patients with punched-out ulcers are associated with an increase in inclusion bodies on histology [Yang H et al. 2017]. Colonic mucosal biopsies stained with H & E may reveal the typical inclusion associated with CMV colitis, “owl eye appearance” inclusion bodies, which are highly specific for CMV. However, H & E staining has low sensitivity compared to immunohistochemistry, which is considered the gold standard for diagnosing CMV colitis.[19]
The histological features of biopsies taken from the rectum are non-specific and cannot differentiate syphilitic proctitis and lymphogranuloma venereum. Laboratory tests, including serology and PCR, are essential in making such differentiation.
History and Physical
Detailed medical history and identification of exposure risks are helpful in the diagnosis. It is essential to mention here that individuals with sickle cell anemia, hemolytic anemia, immunosuppression (corticosteroids, chemotherapy, and AIDS), and extremity of age are at a higher risk of Salmonella infection. Patients with bacterial colitis present with non-specific symptoms, including diarrhea, fever, tenesmus, and abdominal pain. Patients with Yersinia enterocolitica infection may present with a syndrome indistinguishable from acute appendicitis (mesenteric adenitis, mild fever, and ileocecal tenderness).
The incidence of Clostridium difficile is higher in patients with inflammatory bowel disease, particularly ulcerative colitis. Any antibiotic can trigger the disease, but the most common antibiotics responsible are cephalosporins, clindamycin, carbapenems, trimethoprim, sulfonamides, fluoroquinolone, and penicillin combinations.[13]
Patients with Mycobacterial tuberculosis may present with abdominal pain, blood per rectum, fever, sweating, tiredness, and pallor. They may give a past medical history of the treatment of pulmonary tuberculosis. They may have abdominal tenderness in the right iliac fossa (the ileocecal area is the most commonly involved site in intestinal tuberculosis).[18]
Viral colitis (Norovirus, Rotavirus, and Adenovirus) are common in infants and young children. Affected patients present with nausea, vomiting, watery diarrhea, and abdominal pain. CMV infection is frequently symptomatic in immune-competent patients. Again, symptoms are usually non-specific, including diarrhea, abdominal pain, fever, malaise, rectal bleeding, and weight loss. However, hematochezia and diarrhea are the most frequent symptoms. It is difficult to distinguish between ulcerative colitis from CMV colitis based on clinical presentation.[14]
Amoebic colitis usually presents with diarrhea, mucoid discharge, hematochezia, tenesmus, and abdominal bloating. Contaminated water supplies and poor sanitation are often the cases for traveling overseas to endemic areas and increased risk of fecal-oral transmission of amebas.
Patients with colitis-associated with sexually transmitted infection present with anorectal pain, with a purulent, mucoid or bloody discharge, tenesmus, or urgency. The sexual history is vital in evaluating these patients.
Evaluation
Diagnosis of colitis centers on clinical findings, laboratory tests, endoscopy, and biopsy. Endoscopy and biopsy should not be the primary investigations and may be necessary after a critical evaluation of the patient's condition and the results from the initial examination.
Because infection is a common etiology of colitis and can produce clinical presentations indistinguishable from inflammatory bowel disease, microbiological studies and cultures for bacterial and parasitic infestations should be the initial investigations. Laboratory tests including complete blood count, ESR, CRP, arterial blood gases, activated partial thromboplastin time, serum albumin, total protein, blood urea, creatinine, and electrolytes should be ordered. Polymerase chain reaction-based molecular methods (PCR-based multiplex GI pathogens) can help in the rapid identification of nvestigationsSalmonella, Shigella, and Yersinia from primary stool samples. Abdominal and pelvis CT scan, colonoscopy, tissue biopsies, and fecal cultures (multiple specimens) and antimicrobial susceptibility testing should help differentiate infectious from non-infectious causes of colitis and guiding treatment.[15]
Recently multidetector CT scans of the abdomen were used to differentiate between inflammatory bowel disease and acute colitis related to bacterial infection. The five signs described to diagnose bacterial colitis are (1) continuous distribution, (2) empty colon, (3) absence of fat stranding, (4) absence of a "comb' sign, and (5) absence of enlarged lymph nodes.[16]
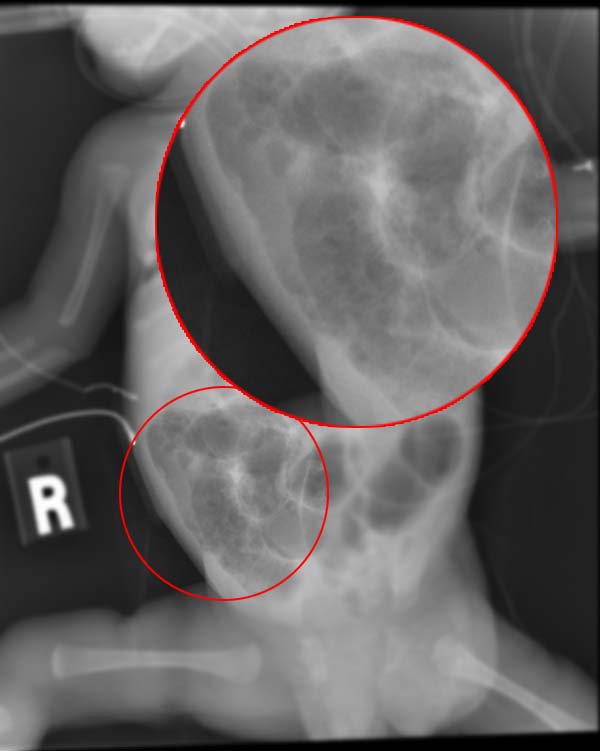
The diagnosis of active Mycobacterium tuberculosis colitis focuses on clinical presentation, clinical examination, and laboratory investigations. A complete blood count may reveal low hemoglobin, leukocytosis, and moderately elevated ESR. Chest X-ray may reveal fibrotic changes, cavitation, or old scar of pulmonary tuberculosis; an abdominal roentgenogram may reveal prominent large bowel. Abdominal and pelvis CT scans may show diffuse thickening of the colonic wall, especially of the terminal ileum and the cecum. A colonoscopy usually shows diffuse ulceration throughout the colon, from the rectum to cecum. Histopathological biopsies taken from the cecum show caseating granuloma and chronic inflammatory cells. Mantoux skin test (tuberculin test) is usually requested. This test does not measure immunity to tuberculosis but the degree of hypersensitivity to tuberculin. The results must be interpreted carefully with consideration to the patient's medical risk factors. Usually, the Mantoux test becomes negative in these patients after being previously positive, indicating the fading of resistance to the organism.[17] PCR testing and cultures of intestinal fluid for bacterial species and acid-fast bacillus are requested.
Diagnosis of CMV colitis uses clinical findings, laboratory tests, and endoscopic findings. Endoscopy and tissue CMV-specific immunohistochemistry (IHC) and or PCR CMV DNA quantification are needed to confirm the diagnosis [20].
In amoebic colitis, rectosigmoid involvement may present on colonoscopy; however, the cecum is the most commonly involved site, followed by the ascending colon (showing colonic inflammation, erythema, oedematous mucosa, erosions, white or yellow exudates, and ulcerations). The presence of amoebic trophozoites on histopathological examination or intestinal fluid cultures is important in the diagnosis. Serum E. histolytica antibody examination and antibody titer greater than 1:128 is considered positive.[17][10]
For patients with suspected sexually transmitted infections of the rectum, histological features of biopsies taken are non-specific and cannot differentiate syphilitic proctitis and lymphogranuloma venereum. Laboratory tests are usually helpful; these include:
- Gonorrhea: Microscopic examination of smears from the lesions showing Gram-negative diplococci. Culture and sensitivity tests of smears taken from lesions.
- Lymphogranuloma venereum: Genotyping of Chlamydia trachomatis- DNA PCR.
- Genital/rectal herpes: Swabs from rectal vesicles or ulcers to detect DNA by PCR.
- Syphilis: Dark-field microscopy, PCR, direct fluorescent antibody test, treponemal antigen-based enzyme immunoassays (EIAs) for IgG and IgM antibodies, Treponema pallidum hemagglutination assay (TPHA), Treponema pallidum particle agglutination assay (TPPA), and fluorescent treponemal antibody absorption (FTA-ABS) test.[20]
Treatment / Management
Not all infectious colitis requires antibiotic therapy; patients with mild to moderate C. jejuni or Salmonella infections do not need antibiotic treatment because the infection is self-limited. Treatment with quinolinic acid antibiotics is only for patients with dysentery and high fever suggestive of bacteremia. Also, patients with AIDS, malignancy, transplantation, prosthetic implants, valvular heart disease, or extreme age will require antibiotic therapy. For mild to moderate C. difficile infection, metronidazole is the preferred treatment. In severe cases of C. difficile infection, oral vancomycin is the recommended approach. In complicated cases, oral vancomycin with intravenous metronidazole is the recommendation.[18]
In patients, particularly children, with enterohemorrhagic E. coli (E. coli O157: 7H and non-O157: H7), antibiotics are not recommendations for treating infection because killing the bacteria can lead to increased release of Shigella toxins and enhance the risk of the hemolytic uremic syndrome.[2]
Because of rising multidrug resistance to antituberculous treatment, cases with active Mycobacterium tuberculosis colitis receive therapy with rifampin, isoniazid, pyrazinamide, and ethambutol for 9 to 12 months. The reader should review the recent guidelines by the World Health Organisation on treating developing resistance in tuberculosis.[19]
The majority of patients with CMV colitis who are immunocompetent may need no treatment with antiviral medications. However, antiviral therapy in immunocompetent patients with CMV colitis could be limited to males over the age of 55 who suffer from severe disease and have co-morbidities affecting the immune system such as diabetes mellitus or chronic renal failure; consider an assessment of the colon viral load. The drug of choice is oral or intravenous ganciclovir.[19]
Treatment of E. histolytica is recommended even in asymptomatic individuals. Noninvasive colitis may be treated with paromomycin to eliminate intraluminal cysts. Metronidazole is the antimicrobial of choice for invasive amoebiasis. Medications with longer half-lives (such as tinidazole and ornidazole) allow for shorter treatment periods and are better tolerated. After completing a 10-day course of a nitroimidazole, the patient should be placed on paromomycin to eradicate the luminal parasites. Fulminant amoebic colitis requires the addition of broad-spectrum antibiotics to the treatment due to the risk of bacterial translocation.[21]
Because of emerging resistance in gonorrhea, current treatment as per current guidelines comprises intramuscular ceftriaxone 500 mg together with an oral dose of azithromycin 1 g. Alternative protocols could be cefixime 400 mg stat or ciprofloxacin 500 mg orally stat.
The treatment of lymphogranuloma venereum uses doxycycline orally twice daily for three weeks, or erythromycin 500 mg orally four times daily for three weeks.[22]
Genital/rectal herpes simplex is treated with acyclovir 400 mg three times daily or valaciclovir 500 mg twice daily for five days. Analgesia and saline bathing could soothe the pain. Intravenous therapy is an option if the patient tolerates oral treatment poorly. Consider prolonging treatment if new lesions develop. For recurrent genital/rectal herpes, lesions are usually mild, may need no specific treatment. Symptomatic treatment could help. Challenging cases such as those with recurrence at short intervals may require referral for specialized advice. The partner should also have an examination and treatment if the lesion is active.
Syphilis treatment is with penicillin (the drug of choice). A single dose of 2.4 mega units of intramuscular benzathine benzylpenicillin is the recommendation for early syphilis or three doses at weekly intervals with late syphilis. Doxycycline could be an alternative treatment for individuals sensitive to penicillin. Follow up patients to ensure clearance from infection and notification are required.[23]
Differential Diagnosis
- Inflammatory bowel disease
- Colorectal cancer
- Diverticulitis
- Ischemic colitis
- Irritable bowel disease
- Drug-induced colitis
- Radiation-associated colitis
- Colitis complicating immune deficiency disorders
- Graft-versus-host disease
- Acute appendicitis/ileocecal mass: The differential diagnosis may include:
- Yersinia enterocolitica infection
- Crohn disease
- Amoebic colitis
- Ulcerative colitis
- Colorectal cancer involving the cecum
Prognosis
Most infectious colitis cases last approximately seven days, with severe cases lingering for several weeks. If left untreated, prolonged disease may be confused for ulcerative colitis.[24]
Complications
Complications include[25][26][27][23]:
- Intestinal perforation
- Toxic megacolon (Clostridium difficile-associated colitis, Salmonella, Shigella, Campylobacter jejuni, Cytomegalovirus, Rotavirus), and fulminant form of amebiasis
- Pseudo-membrane formation (Clostridium difficile)
- Hemorrhagic colitis (enteroinvasive E. coli, enterohemorrhagic E. coli)
- Hemolytic-uremic syndrome (enterohemorrhagic E coli, Campylobacter jejuni, Shigella)
- Post-infectious irritable bowel syndrome, dyspepsia
- Guillain-Barre syndrome (Campylobacter jejuni colitis [serotype HS:19], Cytomegalovirus colitis)
- Encephalitis, seizure (Shigella)
- Reactive arthritis (Shigella, Campylobacter jejuni, Yersinia enterocolitica colitis)
- Pancreatitis, cholecystitis, meningitis, purulent arthritis (Campylobacter jejuni)
- Septic shock and death (Shigella, Clostridium difficile)
- Elevated serum pancreatic enzymes without clinical pancreatitis (Salmonella)
- Renal failure, shock (Clostridium difficile)
- Hypoglycemia, hyponatremia (Shigella)
- Erythema nodosum (Yersinia enterocolitica)
- Patients with CMV colitis complicating inflammatory bowel disease may develop severe hemorrhage, megacolon, fulminant colitis, or colon perforation; these complications contribute to the high risk of mortality
Deterrence and Patient Education
Patients need to receive counsel regarding the importance of antibiotic adherence, as well as any signs of relapse or worsening condition.
Pearls and Other Issues
In managing patients presenting with colitis, computed tomography scans, colonoscopy, and biopsies could help differentiate between infectious and noninfectious colitis. However, these investigations are of little help in deciding the infectious agent causing colitis. Microbiological studies, including microscopy, cultures, and sensitivity, and PCR DNA tests are of high value in defining the etiology of an infectious cause. Treatment of infectious colitis should be individualized depending on the patient’s age, causative agent, risk factors, presence of comorbidities, and current guidelines of management of infectious colitis. Antibiotics treatment of children with E. coli O157: H7 infection increases the risk of hemolytic uremic syndrome and should be avoided.
Enhancing Healthcare Team Outcomes
Infectious colitis is complex and requires an interprofessional team for the diagnosis, management, and early detection of complications. The team comprises a gastroenterologist, infectious disease consultant, pathologist, microbiologist, pharmacist, clinical pharmacologist, and general practitioner, which covers the range of expertise needed for the management of infectious colitis and handling any complications. All members of the interprofessional healthcare team, including clinicians (MDs, DOs, NPs, PAs), specialists, specialty-trained nursing staff, and pharmacists, need to communicate and collaborate across disciplinary lines in their areas of expertise to keep the entire team informed and current on the status of the case and changes required. [Level 5]
The nursing staff should monitor the follow-up of the patient. If signs and symptoms fail to resolve and/or signs or symptoms of dehydration develop, the nursing staff should arrange a return visit or possibly recommend emergency department evaluation.
Careful assessment of the patient condition and involvement of the healthcare team in evaluation and decision making is necessary for better outcomes. The nurse assigned to patient education should focus on teaching patients to wash hands, eating only well-cooked foods, and drinking bottled water, particularly during traveling, which are the essential preventable measures that patients need to know.