Continuing Education Activity
Tinea pedis, also known as athlete's foot or foot ringworm is an infection of the feet affecting soles, interdigital clefts of toes, and nails with a dermatophyte fungus. This activity reviews the evaluation and management of tinea pedis and highlights the role of interprofessional team members in collaborating to provide well-coordinated care and enhance patient outcomes.
Objectives:
- Identify individuals at high risk for tinea pedis.
- Describe the classic presentation of tinea pedis.
- Identify management strategies for tinea pedis.
- Outline the importance of enhancing care coordination among the interprofessional team to ensure proper evaluation and management of tinea pedis.
Introduction
Tinea pedis or foot ringworm is an infection of the feet affecting soles, interdigital clefts of toes, and nails with a dermatophyte fungus. It is also called athlete’s foot.[1][2][3] The infection is caused by the dermatophyte, Trichophyton rubrum which was once endemic to many parts of Africa, Asia, and Australia. However, today the organism can be found in Europe and the Americas.
Etiology
Mainly, Trichophyton rubrum causes tinea pedis. Trichophyton interdigitale and Epidermophyton floccosum are also involved. Other occasional agents include Tricholosporum violaceum. T. rubrum accounts for about 70% of the cases.[4][5]
Risk factors include:
- A hot and humid environment
- Prolonged wear of occlusive footwear
- Excess sweating
- Prolonged exposure to water
Epidemiology
About 10% of the total population may be affected by dermatophyte infections of the toe clefts. It is mostly attributed to wearing of occlusive shoes for long periods. Sharing washing facilities is likely to increase the chances of infection as the incidence of tinea pedis is observed to be higher among those using community baths, showers, and pools. The condition is more common in adult males than in females. The mean age of onset was 15 years in one study.[4][6]
Pathophysiology
Occlusion of toe clefts, maceration, and wet conditions with a simultaneous increase in the bacterial flora probably contribute to tinea pedis infection. Skin breakdown, humidity, and temperature play a role in this infection. The fungus released enzymes called keratinases to invade the keratin layer of skin. In addition, the dermatophyte cell wall also contains molecules called mannans which suppress the body's immune response.
Histopathology
Histologically, it is characterized by acanthosis, hyperkeratosis, and a sparse, superficial, perivascular infiltrate in the dermis. The vesiculobullous form shows spongiosis and parakeratosis. Staining with PAS or methenamine silver stain demonstrates fungal filaments.
History and Physical
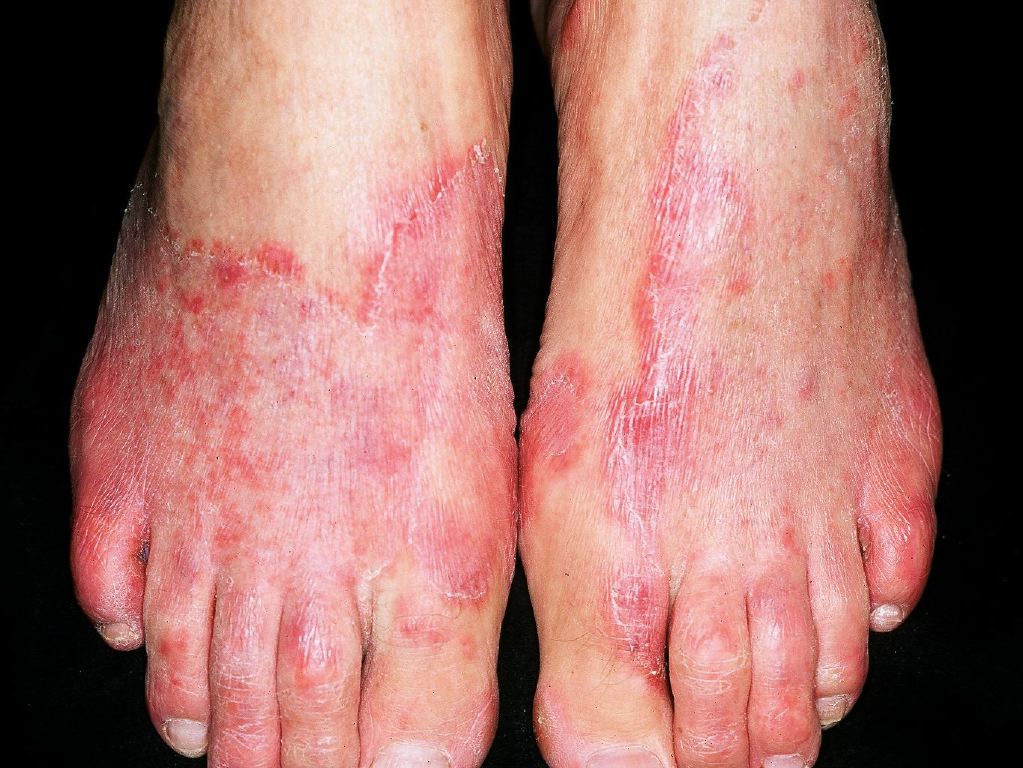
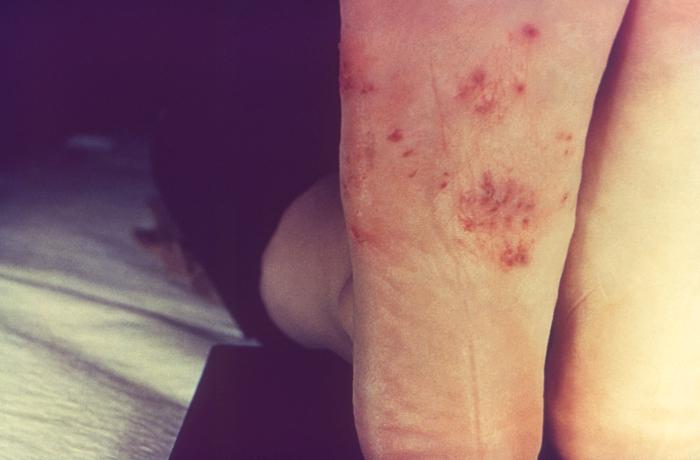
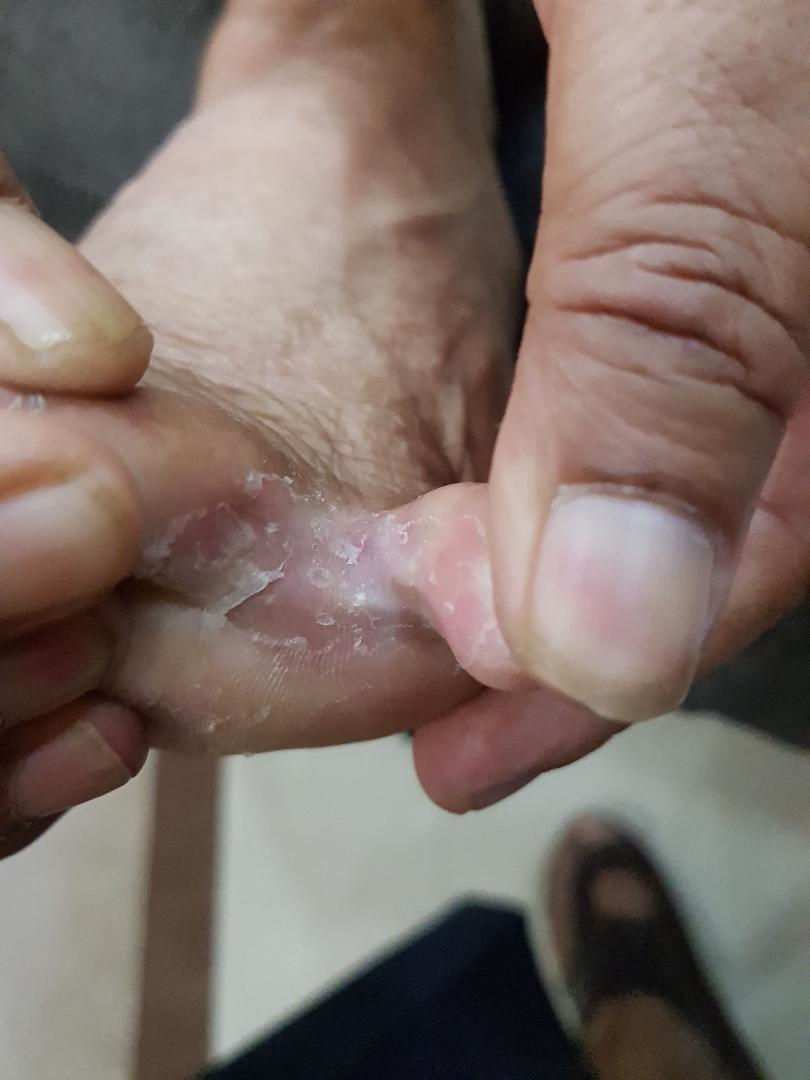
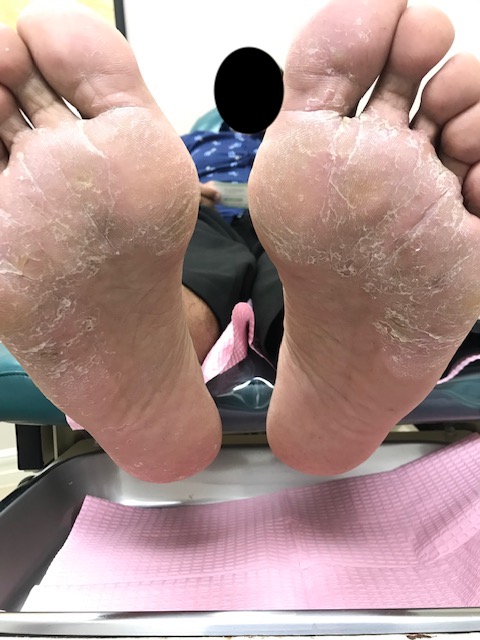
The patients with tinea pedis mostly present as a long-standing, itchy, intertriginous dermatitis of the toes characterized by peeling, maceration, and fissuring. Lateral toe clefts are mainly affected by the involvement of the under the surface of the toes. The affected areas are erythematous and covered with fine, silvery white scales. Occasionally, a pompholyx like the vesicular eruption of the sole may be present. Chronic intertriginous type is the most common presentation. It begins as scaling, maceration, erosion, and erythema of the interdigital and subdigital skin of the feet. Pruritus and malodor are present. Chronic hyperkeratotic or moccasin type usually presents with patchy or diffuse scaling of the bottom, medial, and lateral sides of the soles. The vesiculobullous form is typically caused by Trichophyton mentagrophytes and present as tense vesicles or bullae over the soles. The burning and itching caused by bullae may produce great discomfort. Sometimes, the associated bacterial infection may result in an acute ulcerative type of tinea pedis.
Evaluation
The physical exam is usually sufficient to identify tinea pedis. The diagnosis of tinea pedis may be confirmed by microscopy and culture of skin scrapings. Demonstration of the fungus by microscopic examination of the scrapings taken from the involved site establishes the diagnosis. Dry scales from the instep, heel, and sides of the foot can be gathered by scraping with the edge of a glass microscope slide. Bullae should be unroofed and either the entire roof-mounted intact or scrapings made from the underside of the roof. A few drops of a 10% to 20% solution of potassium hydroxide (KOH) are added to the material on the glass slide. A coverslip is placed over the specimen and examined under the microscope. The addition of 20% to 40% Dimethyl sulfoxide (DMSO) speeds clearing of keratin without the need for heating. A staining method using 100 mg of chlorazol black E dye in 10 mL of DMSO and adding it to a 5% aqueous solution of KOH can be helpful. Toluidine blue, 0.1%, can also be used on thin specimens. The mycelia may be seen under low power, but better observation of both hyphae and spores is obtained by the use of 10 times objective in a microscope.[2][7][8]
Treatment / Management
Improvement of hygiene in swimming pools and bathing areas and frequent washing and cleaning of changing room floors and walkways may help in controlling the infection. Topical treatment is usually adequate for the management in most of the patients. Magenta paint (Castellani’s paint) is still used in some cases of inflammatory tinea pedis, particularly with a coexisting bacterial infection. Topical imidazoles such as clotrimazole, econazole, ketoconazole, miconazole, isoconazole, tioconazole, and sulconazole are effective remedies in tinea pedis with the very low incidence of adverse reactions. Terbinafine and amorolfine applied topically have been shown to produce faster responses as compared to clotrimazole in tinea pedis. The use of tolnaftate powder at swimming baths prophylactically has been shown to reduce levels of toe cleft tinea pedis caused by T. interdigitale. The period of therapy depends on the response of the lesions. Repeated KOH scrapings and cultures should be negative. Much shorter courses are possible with newer antifungal agents.[9][10][11]
Systemic treatment is needed, only if there is involvement of the dorsum of foot, heel, sole of the foot or if the infection is recurrent or has blisters [10]. For adults, terbinafine given orally in a dosage of 250 mg/day produces rapid and long-lasting remissions. Itraconazole, an orally active azole of the triazole series acting through the inhibition of the cytochrome P450-dependent demethylation stage in the formation of ergosterol on the fungal cell membrane is effective in regimens of 200 mg/day for 30 days. Fluconazole is given in a regimen of 150 mg/week for a longer duration. Griseofulvin 500 to 1000 mg/day may also be used. For children, griseofulvin, 10 to 20 mg/kg/day or itraconazole 5 mg/kg/day may be used. Pulse therapy with itraconazole one week/ month is also effective.
Gastrointestinal side effects may occur with fluconazole but are uncommon. Itraconazole may cause gastrointestinal upsets, diarrhea, and peripheral edema, especially when used in conjunction with calcium channel blockers. Hepatotoxicity occurs at a much lower rate with fluconazole and itraconazole as compared to ketoconazole. Terbinafine also produces gastrointestinal upsets, and rarely, hepatitis.
Differential Diagnosis
Hyperkeratotic lesions should be differentiated from psoriasis and heredity or acquired keratodermas.
Interdigital lesions should be differentiated from psoriasis, erythrasma, soft corns, and candidiasis.
Vesiculobullous lesions should be differentiated from pustular psoriasis and dyshidrosis.
Reiter syndrome
Interdigital tinea must be distinguished from simple maceration caused by a closed web space and gram-negative toe web infection.
Prognosis
Prognosis is good provided preventive precautions be taken. Hyperhidrosis is a predisposing factor for tinea infections. Because the disease often starts on the feet, the patient should be advised to dry the toes thoroughly after bathing. Dryness of the parts is essential if reinfection is to be avoided. The use of a good antiseptic powder on the feet after bathing, particularly between the toes, is strongly advised for keeping the part dry in susceptible persons. Tolnaftate or clotrimazole powder is an excellent dusting powder for the feet. Plain talc may be dusted onto socks and shoes to keep the feet dry. Periodic use of a topical antifungal agent may be required, especially when hot occlusive footwear is worn.
Complications
- Cellulitis
- Pyoderma
- Lymphangitis
- Osteomyelitis
In general, complications are more likely to occur in patients who are immunocompromised or are non-ambulatory
Consultations
Internal Medicine
Dermatologist
Deterrence and Patient Education
Maintain clinical hygiene. Avoid walking barefoot.
Pearls and Other Issues
Frequent hosing of the floors of shower rooms and the sides of swimming pools reduce the prevalence of dermatophytes on these surfaces and use of topical antifungal powder, such as tolnaftate, may result in a reduction of tinea pedis infection. Diabetic patients with tinea pedis are more likely to develop onychomycosis. The presence of interdigital tinea pedis is a risk factor for cellulitis in patients with lymphoedema.
Enhancing Healthcare Team Outcomes
Tinea pedis is a very common infection worldwide and is commonly encountered by the general healthcare professional. While the acute condition is managed by the physician, the focus today is on prevention. To lower the morbidity, the infection is best managed by an interprofessional team
Both the nurse and pharmacist need to educate the patient on the potential for reinfection if lifestyle changes are not undertaken. The old shoes should be discarded, and one should avoid sharing personal care items. At the swimming pool or sauna, protective footwear should be worn. The feet should be left dry, and one should avoid wearing constrictive shoes which lack aeration. Cotton socks are preferred, and one may add a drying antifungal powder if the feet are constantly perspiring. Open communication between team members is important to avoid the morbidity of the infection. [12][13] (Level V)
Outcomes
For the majority of healthy people, once treatment is started outcomes are excellent. Most people see symptoms relief in a few days and full recovery in 7-14 days. However, in patients who are hemiplegic or immunocompromised, the tinea infection can be associated with cellulitis or even pyoderma. [14][15](Level V)