Mohs Micrographic Surgery, Optimizing Wound Healing
Mohs Micrographic Surgery, Optimizing Wound Healing
Introduction
Mohs micrographic surgery (MMS) is the preferred treatment for skin cancers due to its precise removal of tumors, sparing as much healthy tissue as possible. However, achieving optimal outcomes after MMS requires more than simply extirpating the tumor; it also depends heavily on effective wound healing. This crucial phase significantly impacts the final cosmetic and functional results for patients. This activity reviews the complex mechanisms of wound healing, identifies factors that can hinder this process, and presents current evidence and innovative strategies to improve wound healing after MMS, ultimately enhancing patient outcomes and satisfaction.
Function
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Function
Understanding the physiology of wound healing is essential for optimizing surgical outcomes and promoting tissue regeneration following MMS. Wound healing after cutaneous surgery is a complex and dynamic process involving intricate cellular and molecular events. The physiological cascade of wound healing can be broadly divided into 4 overlapping phases: hemostasis, inflammation, proliferation, and remodeling.
Hemostasis
Immediately after tissue injury, vasoconstriction and platelet aggregation occur to achieve hemostasis and prevent blood loss. The endothelium of damaged blood vessels rapidly releases endothelin and other vasoconstrictive agents, leading to smooth muscle cell contraction. Concomitantly, circulating platelets adhere to exposed collagen fibers and release granules containing adenosine diphosphate (ADP), thromboxane A2, and serotonin, further promoting platelet aggregation and vasoconstriction. Fibrin clot formation leads to the creation of a temporary matrix. It initiates the release of growth factors, including platelet-derived growth factor (PDGF) and transforming growth factor-β (TGF-β), essential for subsequent healing phases.[1]
Inflammation
The second phase of wound healing is the inflammatory phase, characterized by the influx of immune cells, such as neutrophils and macrophages, that remove debris and pathogens from the wound site. Neutrophils are among the first responders, migrating through the interstitial tissue in response to chemotactic signals, including interleukin-8 (IL-8) and leukotriene B4 (LTB4). These cells phagocytose bacteria and release proteolytic enzymes and reactive oxygen species to neutralize infectious agents. Macrophages, derived from circulating monocytes, play a critical role in debridement by engulfing apoptotic cells and necrotic tissue. These cells also secrete a wide array of cytokines, such as tumor necrosis factor-alpha (TNF-α) and interleukin-1 (IL-1), which amplify the inflammatory response and attract additional immune cells to the wound site.[2]
Proliferation
In the subsequent phase, fibroblasts proliferate and migrate into the wound bed, synthesizing extracellular matrix components such as collagen to restore tissue integrity. Fibroblasts are activated by growth factors, including fibroblast growth factor (FGF) and TGF-β, leading to their differentiation into myofibroblasts, which express α-smooth muscle actin (α-SMA) and contribute to wound contraction. Additionally, keratinocytes at the wound edges proliferate and migrate across the wound bed, a process facilitated by matrix metalloproteinases (MMPs) that degrade the provisional matrix.[3]
Angiogenesis, the formation of new blood vessels, also occurs within the proliferation phase, establishing the healing tissue's oxygen and nutrient supply. This process is driven by vascular endothelial growth factor (VEGF) and involves the proliferation and migration of endothelial cells, resulting in the formation of capillary sprouts that invade the wound matrix.[4]
Remodeling
The newly formed tissue undergoes maturation and reorganization during this final phase, leading to scar formation and tissue remodeling. Collagen fibers are realigned along tension lines, and the extracellular matrix undergoes extensive remodeling mediated by MMPs and their tissue inhibitors (TIMPs).[5] Myofibroblasts play a crucial role in wound contraction by exerting contractile forces on the extracellular matrix. The balance between collagen synthesis and degradation is carefully regulated to prevent excessive scar formation. This highly orchestrated process is tightly regulated by many growth factors, cytokines, and signaling pathways to ensure efficient wound closure and restoration of skin function.
Issues of Concern
Various factors can impede the postoperative wound healing process significantly, thereby leading to complications and suboptimal outcomes. These factors may be related to patient characteristics, wound properties, surgical technique, and postoperative care quality, as discussed below.
Patient-Related Factors
Patient-related factors determine wound healing capacity. Advanced age has been identified as a significant limiting factor, as age-related changes in cellular function, such as decreased keratinocyte and fibroblast proliferative capacity and reduced angiogenesis, can compromise efficient wound healing.[6] Additionally, comorbidities such as diabetes, immunosuppression, and peripheral vascular disease can impair wound healing by disrupting blood flow, immune function, and tissue repair mechanisms.
Diabetes, for example, is associated with leukocyte dysfunction, reduced growth factor production, and neuropathy, which concertedly delay healing and increase the risk of infection. Immunosuppressive states, whether due to medications or underlying conditions, impair the inflammatory phase of wound healing, leading to suboptimal pathogen clearance and delayed progression to the proliferative phase.[7]
Peripheral vascular disease compromises tissue perfusion and oxygenation, essential for collagen synthesis and angiogenesis. Smoking is another notable patient-related factor known to contribute to delayed wound healing.[8] Nicotine and other toxic cigarette components have been shown to cause vasoconstriction, which reduces blood flow to the wound area. Poor circulation lowers hemoglobin's oxygen-carrying capacity, decreases tissue oxygenation, inhibits angiogenesis, and disrupts collagen synthesis and cross-linking, all hindering natural healing.[9]
Wound-Related Factors
Wound-related factors also contribute significantly to the duration of tissue repair and the potential for complications. The size and depth of the wound are critical determinants, with larger and deeper wounds requiring more extensive tissue repair and posing a higher risk of delayed healing.[10] Wounds extending into the subcutaneous tissue or beyond necessitate complex cellular and extracellular matrix activities, increasing the healing time. Moreover, excessive tissue manipulation during surgery can disrupt the wound bed, leading to mechanical tissue damage, compromised circulation, and heightened inflammatory responses. These factors collectively impair the natural healing process and contribute to a prolonged recovery.[11]
Additionally, infections represent a significant impediment to wound healing, as they can cause inflammation and tissue necrosis and impair cellular proliferation, further delaying the healing process. Infections prolong inflammatory responses, leading to excessive production of MMPs that degrade extracellular matrix components critical for healing.[12]
Surgical Technique
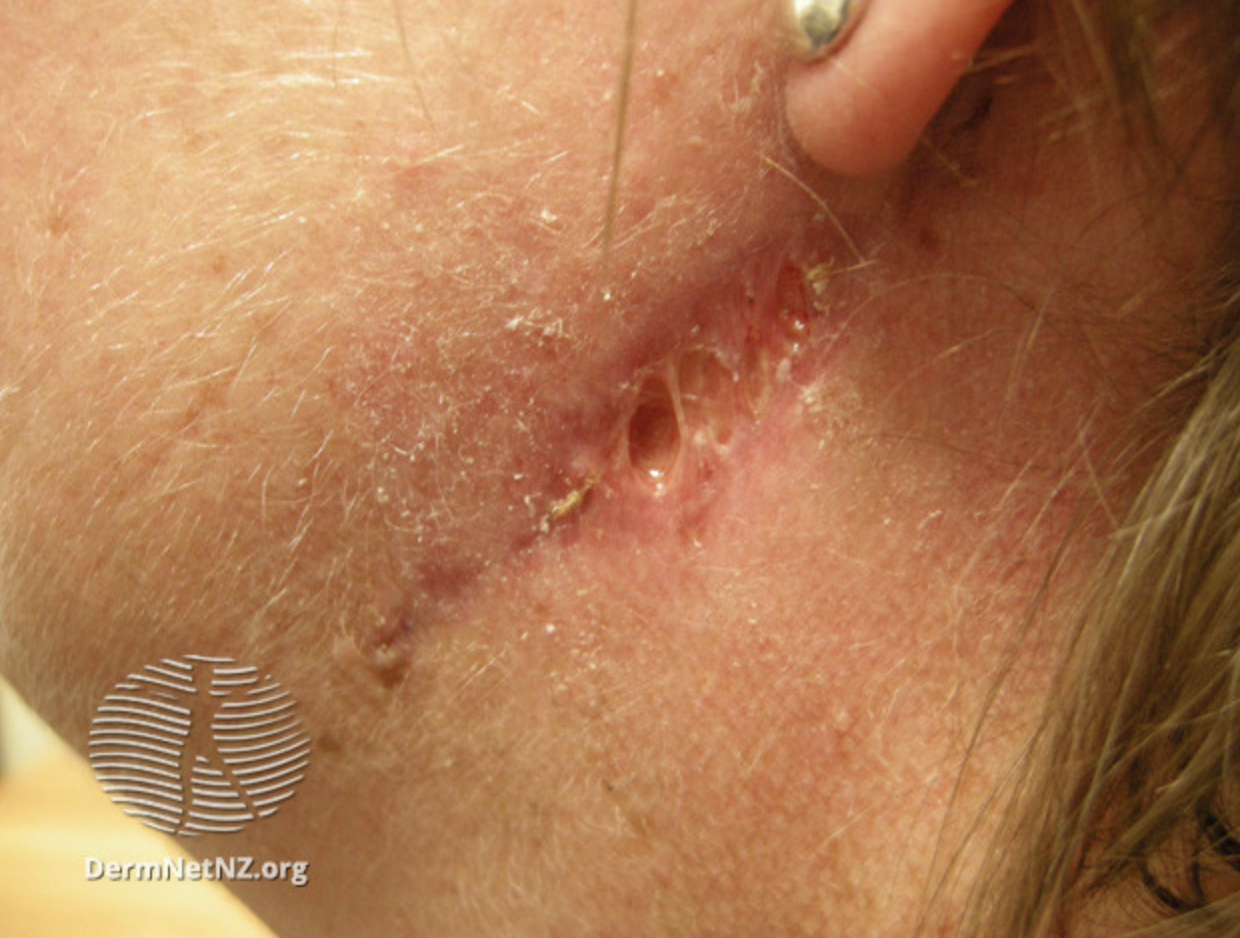
The surgical technique also plays a pivotal role. Poorly performed wound closure techniques that result in excessive tension or improper suture placement can lead to wound dehiscence, ischemia, and suboptimal healing. Excessive tension at the wound edges can cause tissue ischemia by compressing blood vessels and reducing perfusion, while improper suture techniques can lead to tissue necrosis and wound dehiscence (see Image. Surgical Wound Dehiscence). Similarly, failure to minimize wound tension during closure increases the risk of scar contracture, tissue ischemia, and impaired wound healing, highlighting the importance of using tension-reducing techniques such as tension-relieving sutures and surgical flaps.[13]
Postoperative Care
Postoperative care is equally essential for facilitating optimal wound healing outcomes. Poor wound hygiene, characterized by inappropriate wound care practices that include improper cleansing and dressing changes and inadequate wound protection from trauma, can increase the risk of infection and disrupt the healing environment. Inadequate cleansing can leave behind debris and bacteria that may trigger inflammatory responses. Improper dressing changes can either desiccate the wound or create an overly moist environment, both detrimental to healing.
Meanwhile, prolonged immobilization or restricted mobility can impair blood flow and tissue oxygenation, hindering the healing process and increasing the risk of complications such as venous stasis and pressure ulcers. Therefore, comprehensive postoperative care protocols focusing on wound hygiene, proper dressing techniques, and mobilization strategies are essential for promoting timely and effective wound healing following MMS. Mobilization strategies encourage circulation and lymphatic drainage, which are essential for delivering nutrients and removing waste products from the healing tissue.[14]
By incorporating these considerations into patient care, healthcare providers can significantly enhance wound healing outcomes and reduce the incidence of postoperative complications.
Clinical Significance
A comprehensive clinical approach encompassing various strategies may be employed to optimize wound healing following MMS. This multifaceted approach involves preoperative assessment, meticulous surgical technique, comprehensive postoperative care, and tailored interventions based on individual patient needs.
Preoperative Assessment and Patient Education
A thorough preoperative assessment is essential before surgery. Evaluating patient factors such as age, comorbidities, and smoking status allows for risk stratification and tailored interventions. For example, older patients typically have decreased dermal collagen content and reduced fibroblast activity, necessitating closer postoperative monitoring and possible use of adjunctive therapies to enhance healing. In patients with diabetes, assessing glycemic control by obtaining presurgical HbA1c levels helps predict potential healing delays and allows preoperative optimization of blood glucose levels to mitigate these risks.[15]
Patient education regarding wound care expectations and adherence to postoperative instructions is likewise crucial.[16] Educating patients on the importance of proper wound care, such as maintaining a moist wound environment and avoiding mechanical stress on the wound site, can improve patient compliance and satisfaction. Providing detailed instructions on postoperative wound care, signs of infection, and the impact of lifestyle modifications, such as smoking cessation and nutritional optimization, can further enhance healing outcomes.[17] This education may include a demonstration of proper wound-cleaning techniques and a discussion of the impact of dietary choices on wound healing, emphasizing the dependence of tissue repair on adequate levels of proteins, vitamins, and minerals.[18]
Surgical Technique and Wound Closure
Meticulous surgical technique is paramount for promoting optimal wound healing outcomes. Good surgical execution includes minimizing tissue trauma, achieving hemostasis, and utilizing tissue-sparing approaches whenever possible. Techniques such as precise excision with minimal margin clearance while ensuring complete tumor removal help preserve surrounding healthy tissue and reduce the extent of required wound healing. Achieving hemostasis is critical to prevent hematoma formation, which can impede the healing process by creating a nidus of infection and promoting inflammation.[19]
Careful consideration should also be given to wound closure methods, ensuring adequate approximation without excessive tension. Techniques such as layered closure or tension-reducing sutures can help minimize wound tension and facilitate primary intention healing. Layered closure involves suturing the subcutaneous tissue separately from the dermis and epidermis, which distributes tension more evenly and promotes better alignment of collagen fibers during healing. The use of tension-relieving techniques, such as Z-plasty or V-Y advancement flaps, may also be beneficial in areas of high tension.[20]
Additionally, the use of skin substitute grafts has emerged as a valuable adjunctive therapy that promotes secondary intention healing in cases where primary closure is not feasible. Skin substitutes, such as acellular dermal matrices and bioengineered skin constructs, provide a scaffold for cellular ingrowth and promote wound contraction, ultimately expediting the healing process. These substitutes support the migration of keratinocytes and fibroblasts, enhancing reepithelialization and extracellular matrix formation.[21]
Postoperative Wound Care
Proper wound care in the postoperative period plays a significant role in facilitating wound healing. Dressings must be selected based on wound characteristics to help maintain a moist wound environment conducive to healing.[22] Advanced dressings, such as silicone-based dressings or hydrocolloids, create a moist environment that supports wound healing and reduces the risk of hypertrophic scarring (see Image. Hypertrophic Scar Formation). These dressings maintain optimal hydration, facilitate autolytic debridement, and protect against bacterial contamination.[23]
Educating patients on gentle cleansing techniques and providing instructions for pain management are other essential components of postoperative care. Gentle cleansing with noncytotoxic solutions helps remove debris and reduce the risk of infection without impairing cellular activity. Proper pain management is essential to reduce stress-induced cortisol release, which can impede wound healing.[24] Regular wound assessment and monitoring for signs of infection or other complications, such as increased erythema, purulent discharge, and delayed healing, are essential for early intervention.[25]
Addressing Complications and Risk Factors
Prompt identification and management of complications, such as infection and hematoma, are critical for preventing delays in wound healing. Infection management involves appropriate antibiotic use, necrotic tissue debridement, and maintenance of an optimal wound environment (see Image. Surgical Wound Infection). Hematoma evacuation is necessary to prevent pressure-induced ischemia and promote normal healing dynamics. Moreover, addressing modifiable risk factors, such as smoking and nutritional status, can improve healing outcomes significantly. Collaboration with other healthcare professionals, such as wound care specialists and nutritionists, may be necessary to address these factors comprehensively. Ensuring adequate protein, vitamin C, and zinc intake is crucial for collagen synthesis and immune function.
Utilization of Adjunctive Therapies
Adjunctive therapies may be employed to enhance wound healing in select cases. Negative pressure wound therapy (NPWT) promotes granulation tissue formation and wound contraction, particularly in complex wounds.[26] NPWT increases local blood flow, reduces edema, and removes exudates, creating an environment conducive to healing. Similarly, hyperbaric oxygen therapy (HBOT) improves tissue oxygenation and accelerates wound healing in patients with compromised vascularity. HBOT enhances fibroblast proliferation, collagen synthesis, and angiogenesis, providing an adjunctive benefit in ischemic or nonhealing wounds.[27] These adjunctive therapies can be valuable additions to standard wound care protocols, especially in cases of complex wounds and compromised tissue viability.
By integrating these strategies into clinical practice, healthcare providers can optimize wound healing outcomes following cutaneous surgery, leading to improved patient satisfaction and reduced complications. Continued research and innovation in wound management are essential for advancing the field and further improving patient outcomes. The development of novel biomaterials, growth factor therapies, and regenerative medicine approaches holds promise for future advancements in wound healing post-MMS.
Enhancing Healthcare Team Outcomes
Effective coordination within an interprofessional healthcare team is paramount for enhancing patient outcomes following MMS. This collaborative approach involves close communication and coordination among various healthcare professionals, including dermatologists, primary care providers, nurses, medical assistants, wound care specialists, and nutritionists, among others. Dermatologists play a central role in surgical decision-making and wound assessment, while nurses and medical assistants oversee postoperative wound care and monitor for complications.[28] Wound care specialists provide expertise in advanced wound management techniques, such as NPWT and hyperbaric oxygen therapy, which may be indicated for complex or compromised wounds.
Nutritionists play a critical role in optimizing patients' nutritional status, which is essential for supporting wound healing and tissue repair. Primary care physicians are integral members of the interdisciplinary team, assisting in managing comorbidities such as diabetes and hypertension, which can impact wound healing, and providing support for the cessation of smoking, a modifiable risk factor associated with delayed healing. Through collaboration and shared decision-making, the interprofessional healthcare team can ensure comprehensive and holistic care tailored to individual patient needs, ultimately leading to improved wound healing outcomes and enhanced patient satisfaction.
Media
(Click Image to Enlarge)
(Click Image to Enlarge)
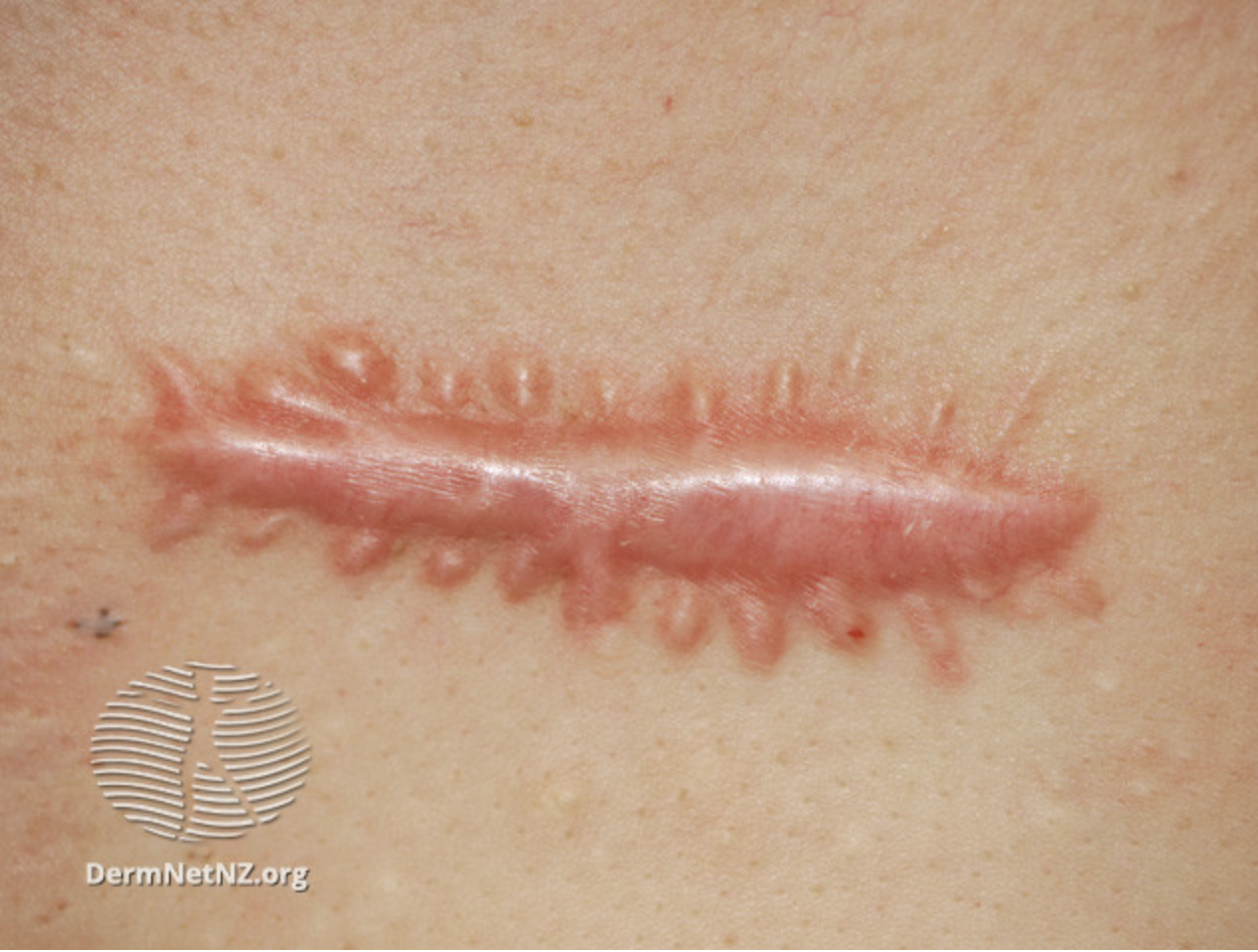
Hypertrophic Scar Formation. This image shows a hypertrophic scar. This type of scar, which forms after the wound has closed, is characterized by raised, red tissue that remains confined to the wound boundaries. This complication arises from excessive collagen production.
Courtesy of DermNet NZ, https://dermnetnz.org/topics/risks-and-complications-of-skin-surgery, accessed 06/13/24
(Click Image to Enlarge)
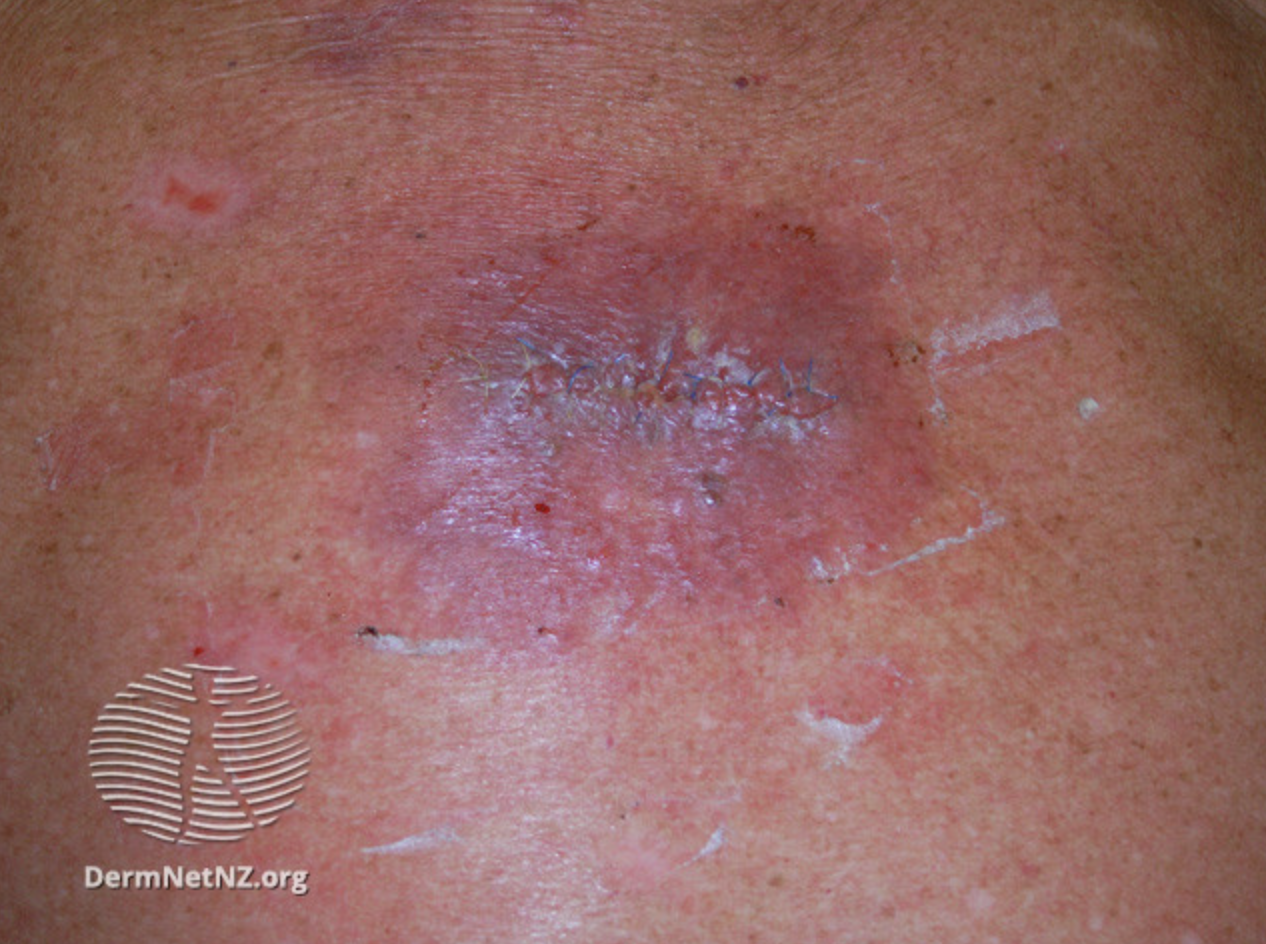
Surgical Wound Infection. This image shows an infected surgical wound. Note the erythema, papules, and pus collection close to the sutured area. Patients may complain of fever and persistent surgical wound pain.
Image courtesy of DermNet NZ, https://dermnetnz.org/topics/wound-infections, accessed 06/13/24
References
Mamun AA, Shao C, Geng P, Wang S, Xiao J. Recent advances in molecular mechanisms of skin wound healing and its treatments. Frontiers in immunology. 2024:15():1395479. doi: 10.3389/fimmu.2024.1395479. Epub 2024 May 21 [PubMed PMID: 38835782]
Level 3 (low-level) evidenceMartin P, Leibovich SJ. Inflammatory cells during wound repair: the good, the bad and the ugly. Trends in cell biology. 2005 Nov:15(11):599-607 [PubMed PMID: 16202600]
Gurtner GC, Werner S, Barrandon Y, Longaker MT. Wound repair and regeneration. Nature. 2008 May 15:453(7193):314-21. doi: 10.1038/nature07039. Epub [PubMed PMID: 18480812]
Farabi B, Roster K, Hirani R, Tepper K, Atak MF, Safai B. The Efficacy of Stem Cells in Wound Healing: A Systematic Review. International journal of molecular sciences. 2024 Mar 5:25(5):. doi: 10.3390/ijms25053006. Epub 2024 Mar 5 [PubMed PMID: 38474251]
Level 1 (high-level) evidenceSinger AJ, Clark RA. Cutaneous wound healing. The New England journal of medicine. 1999 Sep 2:341(10):738-46 [PubMed PMID: 10471461]
Gauglitz GG, Korting HC, Pavicic T, Ruzicka T, Jeschke MG. Hypertrophic scarring and keloids: pathomechanisms and current and emerging treatment strategies. Molecular medicine (Cambridge, Mass.). 2011 Jan-Feb:17(1-2):113-25. doi: 10.2119/molmed.2009.00153. Epub 2010 Oct 5 [PubMed PMID: 20927486]
Broughton G 2nd, Janis JE, Attinger CE. The basic science of wound healing. Plastic and reconstructive surgery. 2006 Jun:117(7 Suppl):12S-34S [PubMed PMID: 16799372]
Troiano C, Jaleel Z, Spiegel JH. Association of Electronic Cigarette Vaping and Cigarette Smoking With Decreased Random Flap Viability in Rats. JAMA facial plastic surgery. 2019 Jan 1:21(1):5-10. doi: 10.1001/jamafacial.2018.1179. Epub [PubMed PMID: 30347026]
Lassig AAD, Bechtold JE, Lindgren BR, Pisansky A, Itabiyi A, Yueh B, Joseph AM. Tobacco exposure and wound healing in head and neck surgical wounds. The Laryngoscope. 2018 Mar:128(3):618-625. doi: 10.1002/lary.26813. Epub 2017 Sep 20 [PubMed PMID: 28940252]
Hunt TK, Hopf HW. Wound healing and wound infection. What surgeons and anesthesiologists can do. The Surgical clinics of North America. 1997 Jun:77(3):587-606 [PubMed PMID: 9194882]
Yazdanparast T, Hassanzadeh H, Nasrollahi SA, Seyedmehdi SM, Jamaati H, Naimian A, Karimi M, Roozbahani R, Firooz A. Cigarettes Smoking and Skin: A Comparison Study of the Biophysical Properties of Skin in Smokers and Non-Smokers. Tanaffos. 2019 Feb:18(2):163-168 [PubMed PMID: 32440305]
Powers JG, Higham C, Broussard K, Phillips TJ. Wound healing and treating wounds: Chronic wound care and management. Journal of the American Academy of Dermatology. 2016 Apr:74(4):607-25; quiz 625-6. doi: 10.1016/j.jaad.2015.08.070. Epub [PubMed PMID: 26979353]
Strickler AG, Shah P, Bajaj S, Mizuguchi R, Nijhawan RI, Odueyungbo M, Rossi A, Ratner D. Preventing and managing complications in dermatologic surgery: Procedural and postsurgical concerns. Journal of the American Academy of Dermatology. 2021 Apr:84(4):895-903. doi: 10.1016/j.jaad.2021.01.037. Epub 2021 Jan 23 [PubMed PMID: 33493570]
Gardner SE, Hillis SL, Heilmann K, Segre JA, Grice EA. The neuropathic diabetic foot ulcer microbiome is associated with clinical factors. Diabetes. 2013 Mar:62(3):923-30. doi: 10.2337/db12-0771. Epub 2012 Nov 8 [PubMed PMID: 23139351]
Xue M, Jackson CJ. Extracellular Matrix Reorganization During Wound Healing and Its Impact on Abnormal Scarring. Advances in wound care. 2015 Mar 1:4(3):119-136 [PubMed PMID: 25785236]
Level 3 (low-level) evidenceShi C, Wang C, Liu H, Li Q, Li R, Zhang Y, Liu Y, Shao Y, Wang J. Selection of Appropriate Wound Dressing for Various Wounds. Frontiers in bioengineering and biotechnology. 2020:8():182. doi: 10.3389/fbioe.2020.00182. Epub 2020 Mar 19 [PubMed PMID: 32266224]
Fronek LF, Harrison TA, Gray TE, Blalock TW. Review of Cutaneous Repairs on the Hand and Fingers Following Dermatologic Surgery. The Journal of clinical and aesthetic dermatology. 2023 Jul:16(7):45-53 [PubMed PMID: 37560505]
Alsharif AT, Alanazi OI, Alqarni RA, Alahmadi HO, Alassiri LA, Alamri SA, Khalifa RM, Alshehab EA, Alzahrani RB, Al Wahbi A. The Impact of Nutritional Condition and Compression Treatment on Venous Ulcer Recovery: A Systematic Review. Cureus. 2024 Apr:16(4):e57407. doi: 10.7759/cureus.57407. Epub 2024 Apr 1 [PubMed PMID: 38694674]
Level 1 (high-level) evidenceBittner GC, Cerci FB, Kubo EM, Tolkachjov SN. Mohs micrographic surgery: a review of indications, technique, outcomes, and considerations. Anais brasileiros de dermatologia. 2021 May-Jun:96(3):263-277. doi: 10.1016/j.abd.2020.10.004. Epub 2021 Mar 24 [PubMed PMID: 33849752]
Dewey J, Bermudez R. Mohs Micrographic Surgery Design and Execution of Advancement Flaps. StatPearls. 2025 Jan:(): [PubMed PMID: 37603654]
Vecin NM, Kirsner RS. Skin substitutes as treatment for chronic wounds: current and future directions. Frontiers in medicine. 2023:10():1154567. doi: 10.3389/fmed.2023.1154567. Epub 2023 Aug 29 [PubMed PMID: 37711741]
Level 3 (low-level) evidenceSood A, Granick MS, Tomaselli NL. Wound Dressings and Comparative Effectiveness Data. Advances in wound care. 2014 Aug 1:3(8):511-529 [PubMed PMID: 25126472]
Level 2 (mid-level) evidenceMustoe TA. Evolution of silicone therapy and mechanism of action in scar management. Aesthetic plastic surgery. 2008 Jan:32(1):82-92 [PubMed PMID: 17968615]
Zahran EM, Mohyeldin RH, Abd El-Mordy FM, Maher SA, Abdel-Maqsoud NMR, Altemani FH, Algehainy NA, Alanazi MA, Jalal MM, Elrehany MA, Bringmann G, Abdelmohsen UR. Wound healing potential of Cystoseira/mesenchymal stem cells in immunosuppressed rats supported by overwhelming immuno-inflammatory crosstalk. PloS one. 2024:19(4):e0300543. doi: 10.1371/journal.pone.0300543. Epub 2024 Apr 4 [PubMed PMID: 38573954]
Haller HL, Sander F, Popp D, Rapp M, Hartmann B, Demircan M, Nischwitz SP, Kamolz LP. Oxygen, pH, Lactate, and Metabolism-How Old Knowledge and New Insights Might Be Combined for New Wound Treatment. Medicina (Kaunas, Lithuania). 2021 Nov 1:57(11):. doi: 10.3390/medicina57111190. Epub 2021 Nov 1 [PubMed PMID: 34833408]
Mantyh C, Silverman R, Collinsworth A, Bongards C, Griffin L. Closed Incision Negative Pressure Therapy Versus Standard of Care Over Closed Abdominal Incisions in the Reduction of Surgical Site Complications: A Systematic Review and Meta-Analysis of Comparative Studies. Eplasty. 2024:24():e33 [PubMed PMID: 38846511]
Level 1 (high-level) evidenceParnis J, Magrin AMF, Hassan H. The role, safety, and efficacy of hyperbaric oxygen therapy in aesthetic practice-An evidence-based review. Journal of cosmetic dermatology. 2024 Jun:23(6):1940-1955. doi: 10.1111/jocd.16228. Epub 2024 Feb 15 [PubMed PMID: 38356446]