Introduction
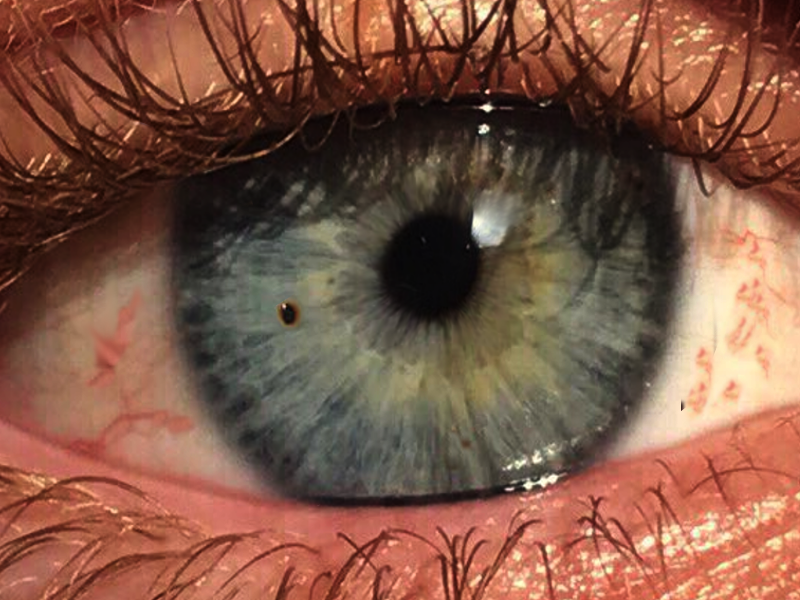
Corneal foreign bodies (CFBs) are the second most common cause of ocular trauma, following corneal abrasions. While major morbidity, such as loss of visual acuity, is rare, many CFBs are superficial and benign, though they can be uncomfortable.[1] CFBs are a common ophthalmic emergency, defined as any external object embedded on or within the corneal surface. These can include metallic, vegetative, and inorganic particles, as well as contact lens fragments. The issue of CFBs is significant due to their potential to cause pain, photophobia, tearing, blurred vision, and complications such as infections and corneal scarring, which, if inadequately managed, may result in permanent vision impairment. CFBs are particularly prevalent among industrial workers, welders, agricultural laborers, and individuals exposed to high-risk environments without appropriate eye protection (see Image. Corneal Foreign Body).[2]
Reports indicate that CFBs contribute significantly to ocular injuries, accounting for 30% to 40% of cases in emergency ophthalmology settings. Incidence rates are higher in low-resource areas where occupational safety measures are inadequate. Patients typically present with acute ocular discomfort, foreign body sensation, redness, excessive tearing, and difficulty keeping the eye open.[3] Clinical examination typically reveals hallmark findings such as corneal epithelial defects, embedded foreign material, corneal edema, rust rings (in metallic foreign bodies), anterior stromal infiltrates, or corneal melt. Although less common, posterior segment complications may include traumatic uveitis, vitreous hemorrhage, or endophthalmitis if the foreign body penetrates deeper ocular layers. Diagnosis starts with a thorough history of the injury, including its nature, mechanism, and duration, followed by slit-lamp biomicroscopy to localize and assess the foreign body’s depth.[4]
Fluorescein staining is useful for highlighting corneal abrasions, whereas imaging techniques such as anterior segment optical coherence tomography (AS-OCT), x-rays, or orbital computed tomography (CT) scans may be necessary for evaluating deeper or radiopaque foreign bodies. Management focuses on the safe and timely removal of the foreign body using sterile instruments such as needles or burrs, typically performed under topical anesthesia. Rust rings from metallic foreign bodies require careful debridement to prevent persistent inflammation. Post-removal care includes prophylactic antibiotics, lubricants, and cycloplegics to prevent infection, reduce pain, and promote healing, with close follow-up to ensure epithelial recovery and prevent secondary complications.[5]
A literature review emphasizes the importance of early intervention and appropriate techniques to minimize complications, highlighting the need for improved eye safety protocols, particularly in occupational settings. Foreign bodies can be classified into metallic, organic (vegetative), and inorganic materials, with organic bodies presenting a higher risk of infection.[6]
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
The etiology of CFBs is multifaceted, often resulting from a combination of high-risk activities and a lack of protective eyewear. These activities include grinding, hammering, drilling, and welding. Additionally, unexpected causes, such as debris from driving or walking, are observed.[7] CFBs are a common ophthalmic emergency, typically resulting from direct mechanical injury and the retention of foreign material on or within the cornea. The etiology is multifaceted, influenced by environmental, occupational, and behavioral factors. Below is a detailed breakdown of the causes.
Occupational Exposure
- Industrial and construction work: Workers in industries involving grinding, drilling, welding, or machining are at high risk for CFBs due to their encounter with metal fragments, wood splinters, and other particulate matter. High-speed machinery often propels debris directly into the eye, significantly increasing the likelihood of foreign body injuries.
- Agricultural settings: Workers exposed to soil, plant material, or organic debris face an elevated risk of foreign body injuries. These foreign bodies may also carry a high microbial load, increasing the risk of infection.
- Chemical processing: Exposure to fine particulate chemicals can result in abrasive or reactive foreign bodies, which can damage the corneal surface.[8]
Environmental Factors
- Windborne particles: Sand, dust, and pollen carried by the wind are common causes of CFBs, especially in arid or dusty regions. Prolonged outdoor exposure without protective eyewear significantly increases the risk.
- Explosions or blasts: In warfare or accidents, small shrapnel and other explosive debris can become embedded in the cornea, posing serious risks to ocular health.[9]
Behavioral and Preventive Lapses
- Lack of protective gear: Failure to wear safety goggles or face shields during high-risk activities significantly increases the risk of CFBs.
- Recreational activities: Certain sports, such as paintball, shooting, or cycling, can lead to high-velocity impacts that embed foreign particles in the eye.
- Poor workplace practices: Neglecting to maintain safe work environments, such as failing to ensure proper ventilation, increases the risk of exposure to airborne debris.[10]
Trauma
- Intentional or accidental injury: Direct eye trauma, such as from altercations, accidents, or falls, can result in foreign materials becoming embedded in the corneal tissue.
- Self-inflicted injuries: Improper handling of contact lenses or cosmetic tools, such as mascara brushes, may introduce fibers or fragments into the eye. Please see StatPearls' companion resource, "Traumatic Cataract," for more information.
Iatrogenic Causes
- Surgical complications: Retention of surgical debris or the accidental introduction of foreign materials can occur during ophthalmic procedures.
- Diagnostic tests: Improper use of diagnostic instruments, such as tonometers or slit lamps, may inadvertently introduce foreign material into the eye.[11]
Infectious and Organic Causes
- Organic foreign bodies: Plant material, insect parts, or animal hair may enter the eye during outdoor activities or animal handling. These organic materials significantly increase the risk of infections, such as fungal or Pythium keratitis.[12][13]
- Infectious agents: CFBs contaminated with microbial pathogens, including bacteria, fungi, or protozoa, can cause secondary infections, particularly in immunocompromised individuals. Please see StatPearls' companion resource, "Herpes Simplex Keratitis," for more information.[14]
Environmental Disasters and Events
- Natural disasters: Earthquakes, hurricanes, and wildfires often disperse debris into the environment, significantly increasing the incidence of CFB injuries among affected populations.
- Vehicular accidents: Glass shards or metallic splinters from broken windshields are common causes of CFBs during traffic collisions.[15]
Pediatric and Geriatric Factors
- Children: Accidental exposure during play activities, often without adult supervision, is a major contributor to foreign body injuries in the pediatric population.
- Geriatric: Older individuals are more prone to retaining CFBs due to reduced blink reflexes and slower tear clearance.[16]
Material Properties
- Metallic foreign bodies: These bodies often lead to rust ring formation if not promptly removed, complicating the clinical presentation.
- Glass and plastic fragments: These are less reactive than organic materials, but they can cause physical trauma and discomfort.
- Reactive chemicals: Substances such as lime, which undergo chemical reactions upon contact with moisture in the eye, can exacerbate corneal damage.[17]
Global Epidemiological Factors
- Developing countries: Limited access to safety equipment and healthcare facilities contributes to a higher prevalence of untreated CFBs.
- Urban versus rural divide: Urban industrial workers are more commonly exposed to metallic or synthetic CFBs, whereas rural populations face greater exposure to organic debris.[18]
Understanding the diverse etiologies of CFBs is essential for implementing targeted preventive measures, ensuring prompt diagnosis, and providing appropriate management. These measures help reduce the risk of complications and promote optimal visual outcomes.
Epidemiology
The incidence of CFBs varies, but a Swedish study found that eye injuries occur at a rate of 8.1 per 1000 individuals, with 40% of these injuries involving corneal or conjunctival foreign bodies. As previously mentioned, most of these injuries occur in occupational settings during high-risk activities, with noncompliance with well-fitting eye protection being a common factor. For example, during the 1991 Gulf War, data from an army field hospital revealed that 14% of the injuries were due to ocular trauma. Of these, 17% were foreign body injuries, and only 3% of the injured patients wore the protective goggles they provided.[19]
CFBs represent a significant global public health issue, particularly in occupational settings. Epidemiological studies show that CFBs account for approximately 30% to 40% of all ocular injuries presenting to emergency departments. Males are disproportionately affected, comprising up to 80% to 90% of cases, largely due to their higher involvement in industrial, agricultural, and construction work. The condition most commonly occurs in individuals aged between 20 and 45, corresponding to the working-age population, who are frequently exposed to high-risk activities such as grinding, welding, hammering, and woodworking.[20]
Geographically, the incidence of CFBs is higher in low- and middle-income countries, where occupational safety measures, such as protective eyewear, are often neglected. Regions with heavy industrialization, including Southeast Asia, South America, and parts of Africa, report higher rates of CFBs, while countries with robust safety regulations tend to have lower incidences. Rural populations, especially those involved in agriculture, face an increased risk of organic foreign bodies, such as wood, thorns, and seeds, which carry a higher risk of infection and subsequent complications, including microbial keratitis.[21]
In urban settings, metallic foreign bodies are more common, often resulting from mechanical grinding or metal-on-metal tasks. While the incidence of CFBs is lower among children, these injuries typically occur due to unintentional trauma during play. Delayed medical intervention can lead to complications, including corneal ulcers, scarring, and visual impairment, underscoring the importance of public awareness and prevention.[22]
Studies estimate an annual incidence of 2.5 to 3 cases per 1000 individuals in the United States, with variations based on socioeconomic status and occupational exposure. Worldwide, disparities in access to eye care and safety education continue to perpetuate the burden of CFBs. Preventative measures, such as consistent use of protective eyewear, occupational training, and awareness programs, are essential for reducing the incidence of CFBs and improving outcomes.
Pathophysiology
The cornea is the anterior surface of the eye, attached circumferentially to the sclera at the limbus. The cornea consists of 5 layers, with the outermost layer being disrupted in cases of corneal abrasions. However, a foreign body can become lodged in any of the 5 corneal layers. Please see StatPearls' companion resource, "Corneal Foreign Body Removal," for more information.
CFB pathophysiology involves a sequence of mechanical, inflammatory, and potentially infectious processes. When a foreign body contacts the cornea, it causes direct trauma to the corneal epithelium, potentially penetrating deeper into the stroma, depending on the velocity, size, and type of foreign object. Superficial injuries typically affect the epithelial layer, while high-impact or sharp foreign bodies can reach deeper layers, including the Bowman membrane and the stroma, resulting in significant structural disruption. Please see StatPearls' companion resource, "Intraocular Foreign Body," for more information.
The corneal nerves and epithelium initiate a strong inflammatory response following injury. The mechanical disruption prompts epithelial cells to release pro-inflammatory cytokines, including interleukins (IL-1 and IL-6) and tumor necrosis factor-alpha (TNF-α), which attract neutrophils and macrophages to the site of injury. While the inflammatory process helps neutralize foreign contaminants, it can also lead to edema, increased vascular permeability, and cellular infiltration, especially if the foreign body remains embedded.[23]
Organic foreign bodies, such as plant materials, carry a higher risk of microbial colonization, potentially leading to bacterial, fungal, or parasitic keratitis infections. In contrast, inorganic materials, such as metallic or glass foreign bodies, are typically inert but may provoke a toxic reaction if they oxidize or release ions, as observed in iron (siderosis) or copper (chalcosis) deposits. Please see StatPearls' companion resource, "Bacterial Keratitis," for more information.
If the body fails to eliminate the foreign object or the inflammation becomes chronic, corneal stromal scarring and neovascularization may compromise corneal transparency and visual acuity. In cases of posterior segment involvement (eg, globe penetration), complications such as endophthalmitis or retinal damage may arise. Prompt diagnosis and management of CFBs are essential to halt this pathophysiological progression and prevent long-term visual impairment.[24]
Histopathology
The cornea consists of 5 distinct layers. The outermost layer, the epithelium, is typically 5 to 6 cell layers thick and composed of epithelial cells. Beneath the epithelium lies the Bowman layer, which is a single layer of basal epithelial cells. The stroma, the thickest layer, is primarily made up of keratocytes. Below the stroma is the Descemet membrane, followed by the innermost monolayer of corneal endothelial cells, which originate from neural crest cells. The 5-layered cornea lacks vasculature and relies on the aqueous humor of the anterior chamber for nutrient supply. A foreign body can disrupt any of these layers, as evidenced by microscopic examinations.[25]
The histopathology of CFBs reveals critical insights into tissue changes resulting from mechanical trauma and ensuing inflammatory processes. Microscopic examination shows features that vary based on the foreign body's composition, duration of presence, and the severity of the inflammatory response.[26]
Early Phase
- In the initial stages, epithelial disruption and superficial trauma manifest as cellular loss, irregular epithelial margins, and swelling in the surrounding epithelial cells.
- The Bowman membrane remains intact in cases of superficial foreign bodies but shows breaks when deeper injuries occur.
- Acute inflammation is prominent, marked by neutrophil infiltration, especially when the foreign body is contaminated or organic in nature.[26]
Foreign Body Reaction
- When the foreign material remains embedded for an extended period, macrophages encircle the object, attempting phagocytosis.
- Multinucleated giant cells often develop, particularly with nondegradable organic or mineral foreign bodies.
- Granulomatous inflammation may appear around plant-based or fungal foreign bodies, characterized by aggregates of epithelioid cells, lymphocytes, and macrophages.[27]
Chronic Changes
- Prolonged inflammation can result in fibrosis and stromal scar formation. The stroma may show thickened collagen fibers and irregular deposition of extracellular matrix components.
- Metallic foreign bodies may lead to the accumulation of deposits such as iron (siderosis) or copper (chalcosis), manifesting as pigmented granules within keratocytes and along the Descemet membrane.[28]
Infective Features
- Microbial colonization may present histopathologically as microbial infiltrates (bacteria, fungi, or parasites), necrotic debris, and neutrophilic abscess formation within the corneal stroma.[29]
Histopathological evaluation is essential in complex or atypical cases to confirm the diagnosis, identify infectious agents, and characterize the foreign body type to guide appropriate management.
History and Physical
The history of the present illness typically involves a sudden onset event. Persistent discomfort without relief often prompts individuals to seek care. Visual acuity deficits are uncommon but may be perceived due to copious tearing and difficulty keeping the eye open. Accompanying symptoms typically reflect a generalized ocular inflammatory response, including tearing, redness, a foreign body sensation, discomfort with both open and closed eyes, photophobia, and blurred vision without significant visual acuity deficit. Many patients report engaging in high-risk activities, such as hammering or grinding, and some may identify the location of the foreign body.[30]
Clinicians should exercise caution when relying on patients to guide the inspection, as most patients inaccurately localize pain associated with CFBs. When a foreign body has been present for more than 24 hours, white blood cells (WBCs) may migrate into the cornea or anterior chamber, indicating iritis. Gross hyphema may suggest globe perforation. Additional examination findings may include eyelid edema and either generalized or focal conjunctival injection. Please see StatPearls' companion resource, "Corneal Foreign Body Removal," for more information.
Common Mechanisms of Injury in Corneal Foreign Bodies
A thorough history and physical examination are essential for diagnosing and managing CFBs. The clinical history often reveals a recent traumatic incident involving the eye. Common mechanisms include:
- Occupational exposure: Activities such as metal grinding, woodcutting, or construction work without protective eyewear are frequent causes.
- Environmental exposure: Outdoor activities may allow foreign bodies, such as sand, dust, or plant material, to enter the eye.
- High-speed impact: Metallic or glass foreign bodies propelled at high velocity during tasks such as hammering metal or explosions are common sources.
- Contact lens use: Poor contact lens hygiene or prolonged use increases susceptibility to micro-debris and foreign body retention.[10]
Key historical points include:
- Nature of the foreign body (organic or inorganic).
- Time of injury and any prior removal attempts.
- Presence of visual disturbances, such as blurring, glare, or photophobia.
- Symptoms such as pain, tearing, foreign body sensation, or redness.[31]
Physical Examination
Patients with corneal CFBs often present with pain, tearing, photophobia, and blepharospasm. Key findings on examination are listed below.
- Inspection
- Localized conjunctival injection: This refers to the redness surrounding the area where the foreign body is located.
- Corneal opacity or infiltration: This may be present if the foreign body is retained.
- Visible foreign body: This may appear dark or reflective under slit-lamp examination.
- Slit-lamp examination
- Epithelial defect: Abrasion or disruption of the corneal epithelium at the site of injury.
- Stromal involvement: Depth of the foreign body dictates stromal reactions, including edema or scarring.
- Rust ring: Metal foreign bodies may deposit rust on the cornea.
- Seidel test: Performed to detect aqueous leakage, indicating a potential corneal perforation.
- Posterior segment
- Dilated fundus examination: This is necessary for high-speed injuries to rule out intraocular foreign bodies (IOFBs).
- Additional tests
- Fluorescein staining: This highlights epithelial defects and helps identify subtle abrasions or retained material.[32]
Differentiation and Risk
The presentation varies based on the composition of the foreign body, as mentioned below.
- Organic material: This carries a higher risk of infection, such as fungal keratitis. Please see StatPearls' companion resource, "Corneal Ulcer," for more information.
- Inorganic metallic: This may lead to rust formation if removal is delayed.
- Glass or plastic: This is generally inert but can cause mechanical irritation.
In summary, it is essential to obtain a detailed history of the mechanism and timing of injury, along with a thorough physical examination emphasizing slit-lamp findings and epithelial disruption. Early detection and comprehensive evaluation are crucial for preventing complications such as infections, scarring, or vision loss.
Evaluation
All suspected CFBs or ocular trauma should be evaluated systematically, thoroughly, and meticulously. A standard routine eye examination is recommended to prevent the common mistake of focusing only on the most obvious findings and overlooking more subtle issues. First, adequate pain control should be administered to all ocular trauma patients to ensure an accurate and thorough exam.[33]
Following pain control, the examination should begin with the 3 vital signs of the eye—visual acuity, pupillary examination, and anterior chamber pressure. The pupillary examination should assess the shape, reactivity, equality, accommodation, and any afferent pupillary defects. Measuring anterior chamber pressure should be done cautiously and may be omitted if globe perforation or rupture is strongly suspected.[34]
Patients suspected of having a CFB should undergo a thorough slit-lamp examination. The entire eye must be inspected, including flipping the upper lid, as foreign bodies can lodge beneath the tarsal plate and cause micro-trauma with each blink. Initial examination should be performed without fluorescein dye, focusing on the lids, lashes, conjunctiva, and sclera. Key observations include injection, chemosis, anterior chamber depth, the presence of cells and flare in the anterior chamber, and any visible foreign bodies.[35]
After adding fluorescein, perform a general inspection once more to check for any corneal abrasions or lacerations. The dye will also facilitate the Seidel test, which, when positive, indicates globe perforation. In a positive test, you may observe a flow of aqueous humor, creating a waterfall-like appearance at the site of trauma. Another subtle indication of a positive Seidel test is a lighter-colored dye in an area, which is caused by dilution from the aqueous humor. This finding is typically seen in very small globe perforations.[36]
After completing the slit lamp examination, additional exams and diagnostics may be considered as adjuncts. These include a full dilated funduscopic exam or CT imaging to evaluate for intraocular or intracranial foreign bodies. Bedside ultrasound can also help detect vitreous hemorrhage or retinal detachment. However, extreme caution should be exercised, as applying pressure to the globe could lead to the extrusion of intraocular contents in the presence of a globe perforation.[37]
The evaluation of CFBs requires a systematic approach that incorporates clinical examination tools, imaging modalities, and laboratory investigations to determine the nature, depth, and associated complications.
Clinical Examination
- History taking: A detailed history of the trauma, including the mechanism, type of material involved, and duration of symptoms, should be obtained. Occupational or recreational activities, such as grinding, drilling, or outdoor work, should be noted as they increase the risk of CFBs. Please see StatPearls' companion resource, "Trauma Secondary Survey," for more information.
- Visual acuity assessment: Baseline visual acuity in both eyes should be assessed using Snellen or logMAR charts. Decreased visual acuity may indicate deeper foreign bodies, epithelial disruption, or secondary complications. Please see StatPearls' companion resource, "Evaluation of Visual Acuity," for more information.
- Slit-lamp biomicroscopy: Slit-lamp biomicroscopy is a critical tool for assessing the below criteria.
- Location: Identifying the foreign body's position in the epithelium, stroma, or anterior chamber.
- Depth: Differentiating between superficial and penetrating injuries.
- Material type: Determining whether the foreign body is metallic, organic, or inert.
- Associated signs: Observing for conjunctival injection, edema, corneal infiltrates, or rust rings.
- Fluorescein staining should be used to highlight epithelial defects and detect the Seidel sign, which indicates globe perforation.[37]
Imaging Modalities
- Plain radiography: This technique is indicated for cases where metallic foreign bodies are suspected, but the history and clinical findings remain inconclusive. This procedure is useful for detecting radiopaque foreign bodies. Please see StatPearls' companion resource, "Foreign Body Imaging," for more information.
- Anterior segment optical coherence tomography: AS-OCT provides detailed imaging of the corneal layers, allowing for precise assessment of penetration depth and extent. This technique is particularly helpful for nonmetallic and organic materials.[38]
- Ultrasound biomicroscopy: This technique assesses deeper IOFBs and helps evaluate the anterior segment, lens, and ciliary body.[39]
- Computed tomography scan: A CT scan is recommended when intraocular or deep-seated foreign bodies are suspected. This technique provides accurate localization and identification of both radiopaque and non-radiopaque objects. Magnetic resonance imaging (MRI) should be avoided if metallic foreign bodies are suspected.[40]
- Magnetic resonance imaging: MRI is only used in cases where nonmetallic foreign bodies, such as wood or plastic, are suspected, as MRI offers superior soft-tissue resolution.[41]
Laboratory Investigations
- Routine blood tests: CBC with differential evaluates for signs of systemic infection if delayed presentation or endophthalmitis is suspected. Inflammatory markers, such as C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR), can support the diagnosis of inflammatory complications.[42]
- Microbiological analysis: Cultures should be performed for organic or suspected infected materials using the below procedures.
- Corneal scrapings: Gram staining, KOH smear, and cultures for bacterial, fungal, and Acanthamoeba infections.
- Polymerase chain reaction: PCR is used to detect rare pathogens.[43]
National and International Guidelines
- American Academy of Ophthalmology: This association recommends slit-lamp examination, fluorescein staining, and imaging to evaluate the depth and associated complications of CFBs. This association also follows sterile techniques for foreign body removal.
- Royal College of Ophthalmologists: This association suggests immediate removal of superficial foreign bodies and detailed imaging for suspected penetrating trauma. This association recommends using CT over MRI when the nature of metallic foreign bodies is uncertain.
- World Health Organization: WHO emphasizes the importance of properly evaluating occupational injuries to prevent complications and promote recovery.[44]
Key Points
- Accurate diagnosis and management require timely and thorough evaluation, incorporating clinical tools, imaging, and laboratory studies.
- Clinical examination is the foundation of assessment, while imaging modalities are crucial for identifying deeper or atypical foreign bodies.
- National and international guidelines emphasize the importance of multidisciplinary approaches and standardized protocols to enhance patient outcomes.[45]
Treatment / Management
For any potential penetrating ocular injury, such as corneal abrasion, foreign body, or globe perforation, the initial treatment focuses on pain control, removal of contact lenses, and eye protection to prevent further trauma. Ocular patches are not recommended for initial management, although protective eye shields may be beneficial for children or altered patients to prevent further trauma from digitization. Pain management can be achieved with topical, oral, intramuscular, or intravenous medications, with topical tetracaine being the most effective. However, overuse of tetracaine can lead to long-term corneal damage, so its use is typically reserved for the first 1 to 2 hours. Please see StatPearls' companion resource, "Corneal Abrasion," for more information.
Cycloplegic eye drops may be beneficial, along with placing a patch over the unaffected eye to minimize pupillary movement. Topical ketorolac has also shown recent benefits, though it should be avoided in pregnant patients. Additionally, systemic pain relief may be necessary if the patient cannot tolerate the examination. However, caution is advised when using systemic pain relief due to the increasing prevalence of dependence and misuse syndrome in recent years.[46]
Foreign body removal should be initiated as soon as possible, ideally within 24 hours, as after this time, the foreign body may become embedded in the corneal stroma, making removal more challenging. If the foreign body is suspected to be or has physical exam findings consistent with the involvement of full stromal thickness, an ophthalmologist should remove it immediately. While there are various methods for foreign body removal, a step-wise approach is generally considered the most effective.
After a thorough examination, the following techniques are recommended to rule out globe perforation.[47]
- Simple irrigation and a moist cotton swab are the first steps, as most recent and superficial foreign bodies can be successfully removed this way. If this approach is unsuccessful, the bevel of a needle can be used under slit-lamp guidance. While the physician's personal preference may vary, most texts recommend using a 25- to 30-gauge needle attached to a TB syringe for optimal control.[48]
- Another method for removal is using an ophthalmic corneal burr, also known as a spud or, more commonly, the "Alger brush." This tool serves 2 main functions:
- The tool can rotate to flick out the foreign body.
- The tool, more commonly, is used to shave down the rust ring left by a metallic foreign body.
In cases of full-thickness or intraocular foreign bodies, the options for removal are more limited. The patient can be observed serially if the foreign body is inert, such as glass or plastic. However, all metallic foreign bodies should be removed, regardless of depth, as they react with the corneal stroma, causing a rust ring. Small rust rings can be left in place, as they often resolve on their own, or they can be gradually shaved away as the stroma regenerates. However, central CFBs or rust rings should be aggressively removed, as they have the most significant impact on future vision. Inadequate removal of rust rings can lead to secondary iritis.[49]
Upon successful removal of the foreign body, treatment includes pain control, follow-up, and consideration of prophylactic antibiotics. For contact lens wearers, antibiotics with anti-pseudomonal coverage should be chosen. A study found that 90% of bacteria cultured from CFBs were sensitive to fluoroquinolone drops.[50] Pain relief with topical ketorolac has not been shown to impair corneal healing. Cycloplegics can also be used for comfort, although atropine should be avoided due to its prolonged effect, which can last up to 2 weeks.
Lubricating eye drops can also be beneficial. The use of an eye patch has been a topic of considerable controversy. Eye patches are contraindicated in contact lens wearers and for organic foreign bodies, as they may increase the risk of infection. Additionally, patches have not been shown to improve corneal healing time or reduce symptomatic days. After foreign body removal, treatment follows the same protocol as for a corneal abrasion. A prospective, 3-arm, randomized study found that patching had no impact on the time to comfort or healing.[51](A1)
The treatment of CFBs requires prompt removal, infection prevention, and ocular surface rehabilitation. The approach depends on factors such as the type, depth, and location of the foreign body, as well as the presence of any associated complications.
Initial Assessment and Stabilization
- Pain and tetanus prophylaxis: Topical anesthetics should be administered for pain relief during the examination. The patient's tetanus immunization status should be verified, and prophylaxis should be provided if necessary, especially for injuries involving organic foreign bodies.
- Visual acuity: Baseline visual acuity should be recorded before any intervention.[52] (B3)
Removal Techniques
- Superficial foreign bodies: Under slit-lamp guidance, a sterile cotton swab or small 25-gauge needle can be used to dislodge foreign material.
- Embedded foreign bodies: Specialized tools, such as a foreign body spud or jeweler's forceps, should be used for deeper foreign bodies. Performing the removal under magnification ensures accuracy and minimizes collateral damage.
- Rust rings: For metallic foreign bodies, rust rings should be removed using an ophthalmic burr, ideally within 24 hours, to prevent further corneal damage.[53]
Medical Management
- Antibiotics: Prophylactic broad-spectrum antibiotics, such as fluoroquinolones, should be prescribed to prevent infection. If an infection is suspected, therapy should be tailored based on microbial cultures.
- Anti-inflammatory agents: Topical steroids should be used cautiously to manage inflammation, with close monitoring for delayed wound healing or secondary infections.
- Artificial tears: Lubricating drops or ointments are recommended to promote epithelial healing and alleviate discomfort.[54]
Surgical Interventions
- Surgical exploration: In cases of perforation or posterior segment extension, surgical removal through the anterior chamber or vitreoretinal surgery may be necessary.
- Corneal repair: For large epithelial defects or lacerations, corneal suturing should be performed to facilitate healing.[55]
Adjunctive Therapies
- Bandage contact lens: A bandage contact lens can be used to protect the corneal surface and promote re-epithelialization. Please see StatPearls' companion resource, "Contact Lens–Related Complications," for more information.
- Cycloplegics: Cycloplegics help alleviate ciliary spasms and reduce pain associated with anterior chamber inflammation.
Follow-Up Care
- Monitoring: A follow-up should be scheduled within 24 to 48 hours to assess healing, check for any remaining foreign material, and monitor for secondary complications such as infection or scarring.
- Complication management: Clinicians should promptly address sequelae such as corneal ulcers or opacification.[56]
National and International Guidelines
- American Academy of Ophthalmology: The academy recommends immediate foreign body removal and infection prophylaxis. This association emphasizes the use of imaging in cases of incomplete removal or suspected intraocular extension.
- World Health Organization: WHO stresses the importance of early diagnosis and management to prevent vision-threatening complications, particularly in low-resource settings.
- Royal College of Ophthalmologists: The academy advocates using bandage contact lenses and lubrication after removal to optimize healing.
Early intervention and adherence to established guidelines are essential for minimizing complications and preserving vision in patients with CFBs. Proper patient education and follow-up are crucial to ensure effective recovery and prevent recurrent injuries.[57](A1)
Differential Diagnosis
Any painful red eye with a foreign body sensation requires ruling out other potential etiologies. A broad differential diagnosis is essential. Infectious causes may include corneal ulcers, herpes zoster ophthalmicus, herpes simplex keratoconjunctivitis, or other viral or bacterial conjunctivitis.
- Corneal abrasion: Surface epithelial loss due to trauma, often mimicking the symptoms of foreign bodies.
- Corneal ulcer: Infectious or sterile ulceration associated with pain, photophobia, and infiltration.
- Herpes simplex keratitis: Dendritic ulcers on the cornea that resemble abrasions or foreign material.
- Corneal infiltrate: An inflammatory reaction that can resemble the appearance of retained organic material.
- Recurrent corneal erosion: Episodic epithelial defects, often with a history of previous trauma or erosion.
- Conjunctival foreign body: Often overlooked due to overlapping symptoms and its location near the fornix.
- Pinguecula or pterygium: Raised conjunctival growths that can simulate foreign bodies.
- Corneal scar: Old scars may resemble foreign bodies upon slit-lamp examination.
- Corneal dystrophies (eg, granular or lattice): Accumulation of deposits in the corneal stroma.
- Corneal endothelial guttata: Endothelial changes visible under retro-illumination.
- Anterior chamber hypopyon: WBC layering that can resemble IOFBs.
- Keratoconus: Irregular astigmatism and stromal thinning, which may be misinterpreted as anterior changes.
- Subepithelial infiltrates: Post-viral or allergic reactions that appear as foreign material.
- Contact lens deposits: Accumulation on lenses that leads to visual symptoms mimicking corneal debris.
- Fungal or acanthamoeba keratitis: Organic material or infiltrates that may be misdiagnosed as foreign bodies.
- Epithelial inclusion cysts: Localized corneal epithelial cysts that resemble retained material.
- Intraocular foreign body: Deep-seated foreign material extending into the anterior or posterior chamber.
- Corneal neovascularization: Abnormal blood vessel growth that may resemble embedded fibers.
- Dry eye disease: Filamentary keratitis or mucous strands that present as corneal material.
- Suture-associated keratitis: Suture fragments or irritation following ocular surgery.
- Globe perforation or rupture: A full-thickness injury to the eyeball caused by trauma, often requiring immediate surgical intervention to preserve vision.
- Intraocular foreign body: A foreign object lodged inside the eye, potentially causing severe ocular damage and necessitating urgent removal.
- Retinal or vitreous detachment or hemorrhage: Separation of the retina or bleeding within the vitreous, which leads to vision loss and requires prompt evaluation and treatment.
- Uveitis: Inflammation of the uveal tract, presenting with redness, pain, and photophobia, often linked to autoimmune or infectious causes.
- Iritis: Anterior uveitis specifically affects the iris and is characterized by pain, light sensitivity, and blurred vision.
- Endophthalmitis: Severe intraocular infection, usually following surgery or trauma, with rapid onset of pain, redness, and vision loss.
- Ultraviolet keratitis: Painful corneal injury caused by prolonged UV exposure, often seen in welders or from sunlamp exposure.
- Exposure keratitis: Corneal inflammation due to incomplete eyelid closure, leading to dryness and surface damage.
- Chemical injuries: Ocular damage caused by exposure to acids or alkalis, requiring immediate irrigation to minimize tissue destruction.
Pertinent Studies and Ongoing Trials
Research on CFBs continues to evolve, focusing on improving diagnostic accuracy, optimizing removal techniques, and reducing complications. A recent study published in the Journal of Cataract and Refractive Surgery evaluated the efficacy of AS-OCT in detecting and localizing CFBs, particularly in cases where slit-lamp biomicroscopy yielded inconclusive results. The study demonstrated a 95% accuracy rate in identifying the precise depth and location of both metallic and organic foreign bodies.[58]
In management, ongoing clinical trials evaluate the use of femtosecond laser technology for precise removal of deeply embedded foreign bodies to minimize tissue trauma and corneal scarring. Additionally, researchers are investigating the efficacy of antimicrobial-loaded contact lenses in reducing the risk of secondary infections following foreign body removal, particularly in high-risk patients.[59]
A multicenter trial conducted by the American Academy of Ophthalmology evaluates corneal healing agents, including recombinant growth factors and stem cell-based therapies, to promote epithelial recovery and prevent stromal scarring. Preliminary results show significant improvements in wound healing rates and visual outcomes compared to conventional treatments.[60]
Emerging evidence underscores the importance of protective measures in preventing corneal injuries. A large-scale epidemiological study from Europe reported a 40% reduction in workplace-related corneal injuries after mandating the use of industrial eye protection. Current trials are exploring innovative safety eyewear featuring impact resistance and blue-light filtering to reduce occupational hazards. These advancements aim to bridge diagnostic gaps, streamline treatment protocols, and improve patient outcomes in managing conjunctival foreign bodies, contributing to evidence-based ophthalmic care.[61]
Treatment Planning
Treatment planning for CFBs requires a stepwise and comprehensive approach to ensure prompt removal, prevent complications, and promote ocular healing. The process begins with a thorough history and clinical examination to determine the mechanism of injury, the type of foreign body (metallic, organic, or inert), and associated symptoms such as pain, tearing, photophobia, or vision changes. Please see StatPearls' companion resource, "Corneal Foreign Body Removal," for more information.
Initial Assessment
Slit-lamp biomicroscopy is essential for evaluating the size, depth, and location of the foreign body, as well as any associated damage, such as corneal abrasions, stromal edema, or anterior chamber reactions. In cases of high-velocity trauma or suspected IOFBs, advanced imaging techniques such as AS-OCT, x-ray, or CT scan are recommended to assess for deeper penetration or retained fragments.[37]
Foreign Body Removal
The primary objective is the atraumatic removal of the foreign body. Superficial CFBs can be removed using sterile needles, spuds, or burr drills under topical anesthesia. Metallic foreign bodies may necessitate rust ring removal to facilitate epithelial healing. For deeper or centrally located CFBs, ophthalmic surgical intervention might be required to prevent complications such as corneal perforation. Please see StatPearls' companion resource, "Foreign Body Imaging," for more information.
Post-Removal Care
Post-procedure care includes the use of topical antibiotics to prevent infection, cycloplegics to reduce inflammation, and lubricating agents to support epithelial recovery. A bandage contact lens may be applied to enhance comfort and promote healing in cases of larger abrasions. Patients should be closely monitored for secondary complications, such as corneal scarring, uveitis, or infection.
Long-Term Follow-Up
Regular follow-ups are crucial to monitor epithelial closure and visual recovery. In cases with residual scarring or stromal opacity, visual rehabilitation options such as phototherapeutic keratectomy or corneal transplantation may be considered. Preventive education on using protective eyewear is also emphasized to avoid future injuries.[62]
Toxicity and Adverse Effect Management
Most complications, toxicities, and adverse effects are associated with metallic foreign bodies. Full-thickness foreign bodies leading to globe perforation present specific complications, although this is outside the scope of this topic. Metallic foreign bodies can lead to the formation of a rust ring, which may progress to reactive iritis. This can result in significant pain, vision loss, and an increased risk of secondary infection or keratitis. These complications can be effectively managed through prompt foreign body removal, rust ring removal, and close outpatient follow-up with an ophthalmologist.[63]
CFBs can lead to various toxicities and adverse effects based on their type, location, and timely management. Metallic foreign bodies, especially those containing iron, can cause rust ring formation, resulting in secondary stromal damage due to oxidative reactions. Prompt removal with specialized tools is essential. Organic foreign bodies (such as plant material) can trigger severe inflammatory responses and fungal infections, potentially progressing to corneal ulcers or abscesses if left untreated.[64]
Adverse effects of retained foreign bodies include epithelial defects, stromal thinning, corneal scarring, and visual impairment. Chemical toxicity from alkali or acidic particles can worsen corneal damage, leading to limbal ischemia and delayed epithelial healing. Moreover, improper removal techniques can cause complications such as corneal perforation, hypopyon formation, or traumatic anterior uveitis.[65]
Management focuses on promptly and safely removing CFBs using slit-lamp magnification or surgical intervention if deep penetration is suspected. To address adverse effects, topical antibiotics are prescribed to prevent secondary infections, while cycloplegics help manage anterior segment inflammation. Lubricants and bandage contact lenses can promote epithelial healing. Surgical repair or corneal transplantation may be necessary in severe cases to restore ocular integrity and vision.[66]
Preventing adverse effects involves early diagnosis of foreign body toxicity, appropriate imaging (eg, AS-OCT), and tailored treatment based on the type of material. Education on the use of protective eyewear is essential to reduce the incidence of occupational and environmental corneal injuries.[67]
Staging
Staging of CFBs is classified based on penetration depth, location, and associated ocular involvement. This staging helps guide clinical management and predict outcomes.
Stage 1: Superficial Foreign Bodies
- The foreign body is embedded in the corneal epithelium without stromal involvement.
- Symptoms are minimal, including tearing, irritation, and foreign body sensation.
- This is generally managed with irrigation or superficial removal.[2]
Stage 2: Subepithelial or Stromal Foreign Bodies
- The foreign body extends into the anterior stroma without penetrating the deeper layers.
- Patients may experience significant discomfort, photophobia, and tearing.
- Rust rings (from metallic foreign bodies) may develop at this stage.[68]
Stage 3: Deep Stromal Penetration
- A foreign body is embedded deep into the corneal stroma.
- The risk of scarring, infection, and visual impairment increases.
- This stage requires meticulous removal, often under slit-lamp magnification.[68]
Stage 4: Full-Thickness Perforating Foreign Bodies
- The foreign body penetrates through the full corneal thickness, potentially entering the anterior chamber.
- Signs include a positive Seidel test, hyphema, or secondary infections such as endophthalmitis.
- Surgical intervention, such as suturing and managing intraocular complications, is required.[69]
Stage 5: Posterior Segment Involvement
- The foreign body extends beyond the cornea, involving the lens, vitreous, or retina.
- This stage poses a risk of severe complications, such as cataract formation, retinal detachment, and endophthalmitis.
- This stage requires advanced imaging and surgical intervention, such as vitrectomy.[70]
Staging emphasizes the importance of early detection and treatment to minimize morbidity and optimize visual outcomes.
Prognosis
The prognosis for CFBs depends on factors such as size, location, and depth of the foreign body, as well as the timing of intervention and complications. In most cases, superficial and peripheral CFBs that are promptly identified and removed typically have an excellent prognosis, with complete recovery of vision and resolution of symptoms, as well as minimal long-term effects, if promptly identified and removed. Proper wound healing and minimal scarring usually prevent long-term effects. However, centrally located or full-thickness CFBs, while still associated with a good long-term prognosis, present a higher risk of complications and require closer follow-up.
Deeper or retained foreign bodies, especially metallic or organic, may cause rust ring formation, secondary infections such as bacterial or fungal keratitis, or corneal scarring, potentially impairing visual acuity. These cases require closer and more frequent follow-up appointments to minimize the risk of visual impairment. All centrally located rust rings pose a greater risk of visually significant scarring, but timely management and careful monitoring can help prevent this outcome.[2] Please see StatPearls' companion resource, "Corneal Foreign Body Removal," for more information.
Delayed management, improper foreign body removal, or inadequate follow-up increases the risk of complications such as corneal ulceration, recurrent erosions, and stromal thinning, which can negatively affect prognosis. Posterior segment involvement, perforation, or endophthalmitis may severely compromise vision and could lead to globe loss. However, with timely removal, topical antibiotics, anti-inflammatory therapy, and proper patient education, the overall prognosis remains favorable, and vision can often be fully restored.[24]
Complications
Although complications from CFBs are rare, they can be severe. These typically include reactive iritis often due to delayed foreign body removal (beyond 24 hours) or retained rust rings. A risk of visually significant scarring, especially with centrally located foreign bodies or retained rust rings, also exists.
- Corneal abrasion: Surface epithelial damage during foreign body removal.
- Corneal ulceration: Infection leading to stromal necrosis and ulcer formation.
- Infectious keratitis: Bacterial, fungal, or parasitic infection secondary to trauma.
- Rust ring formation: Residual metallic debris causing corneal staining and irritation.
- Corneal scarring: Persistent injury or infection leading to visual impairment.
- Corneal edema: Swelling caused by endothelial dysfunction following trauma.
- Anterior uveitis: Inflammation of the anterior segment triggered by irritation or infection.
- Hypopyon formation: Accumulation of inflammatory cells in the anterior chamber.
- Secondary glaucoma: Increased intraocular pressure due to inflammation.
- Endophthalmitis: Rare but severe intraocular infection due to deep penetration of pathogens.
- Descemet membrane detachment: Damage resulting in fluid accumulation between corneal layers.
- Siderosis bulbi: Iron deposition in the eye due to retained metallic foreign bodies.
- Traumatic cataract: Damage to the lens causing opacification.
- Corneal perforation: Full-thickness penetration of the cornea.
- Recurrent corneal erosion: Ongoing epithelial healing issues causing persistent pain.
- Reduced visual acuity: Caused by corneal scarring or irregular astigmatism.
- Corneal neovascularization: Abnormal blood vessel growth due to chronic irritation.
- Astigmatism: Irregular corneal curvature from scarring or surface changes.
- Photophobia: Persistent light sensitivity following trauma.
- Sympathetic ophthalmia: Rare bilateral granulomatous uveitis due to intraocular inflammation.
These complications underscore the importance of prompt diagnosis, meticulous foreign body removal, and careful follow-up to prevent long-term visual impairment.
Postoperative and Rehabilitation Care
Postoperative care following CFB removal is essential for promoting healing, preventing complications, and restoring visual function. Immediately after removal, topical antibiotics are prescribed to prevent secondary infections, along with lubricating drops to maintain adequate ocular surface hydration. For cases with significant corneal abrasions, cycloplegic agents may be used to relieve pain from ciliary muscle spasms. Regular follow-up examinations are crucial to monitor healing progress and detect potential complications such as corneal ulcers, infections, or persistent epithelial defects. Further removal within 24 to 48 hours may be necessary in cases involving rust rings or metallic remnants to ensure complete corneal recovery.[71]
Rehabilitation focuses on managing residual symptoms such as photophobia or mild discomfort by using protective measures such as sunglasses and continuing the use of lubricants. Patients with occupational risks should be educated about the importance of wearing protective eyewear to prevent recurrence. In severe cases where visual acuity is impaired due to corneal scarring, interventions such as corneal debridement, bandage contact lenses, or phototherapeutic keratectomy may be considered for visual rehabilitation. Patient education on medication compliance, recognizing signs of infection (such as pain, redness, and discharge), and seeking timely medical attention is crucial for optimal outcomes. Long-term rehabilitation aims to prevent recurrence and restore full visual function, ensuring patients can return to normal activities safely and effectively.[72]
Consultations
All patients with a CFB require close follow-up with an ophthalmologist. For patients with peripherally located CFBs and no retained foreign material, a follow-up appointment can be scheduled within 2 to 3 days. Centrally located CFBs or retained rust rings should be evaluated immediately, ideally within 24 hours of the event. Retained inert foreign bodies should be monitored regularly, with follow-up timing determined on a case-by-case basis, as is the case with IOFBs. Once the patient returns to baseline, annual ophthalmologic follow-up is recommended unless otherwise specified.[5]
Consultations are pivotal in managing CFBs to ensure appropriate care and avoid complications. Prompt referral to an ophthalmologist is essential when a CFB is suspected, especially if it is deeply embedded, associated with significant ocular trauma, or suspected of causing globe perforation. Emergency physicians and general practitioners should consult ophthalmologists for cases involving metallic foreign bodies, rust rings, or posterior segment involvement. Delayed referrals can lead to complications such as infection, corneal scarring, or endophthalmitis. In cases where the foreign body has caused secondary complications, such as hyphema, anterior chamber inflammation, or vision loss, a corneal specialist may offer specialized management. If the patient experiences recurrent foreign bodies or has occupational risk factors, consulting occupational healthcare specialists can help develop more effective preventive strategies.[49]
For high-risk scenarios, such as chemical foreign bodies or suspected IOFBs, a multidisciplinary consultation involving ophthalmology, radiology, and, when necessary, surgical teams ensures comprehensive care. Rapid intervention minimizes the risk of long-term visual impairment. Overall, timely and coordinated consultations improve patient outcomes, prevent complications, and ensure proper follow-up care.[73]
Deterrence and Patient Education
Most CFBs directly result from noncompliance with well-fitting safety goggles. Patients should be educated on the importance of wearing proper protective eyewear during high-risk activities and ensuring a secure fit, as loose or inadequate protective eyewear can lead to ocular trauma.[64]
Patient education and preventive strategies are essential in minimizing the incidence of CFBs. The key to prevention is raising awareness and promoting protective measures. High-risk individuals, including construction workers, welders, metal grinders, and gardeners, should be educated on the importance of wearing appropriate eyewear, such as safety goggles or shields, during hazardous activities. Employers must enforce safety protocols and ensure access to protective gear in the workplace.[74]
Patients must be educated about the risks of delayed medical intervention after ocular trauma. Prompt evaluation is essential to prevent complications such as infection, scarring, or globe penetration. Education should focus on recognizing symptoms such as persistent foreign body sensation, tearing, pain, photophobia, and reduced vision, all of which require immediate medical attention. Please see StatPearls' companion resource, "Ocular Trauma Prevention Strategies and Patient Counseling," for more information.
For long-term deterrence, clinicians should emphasize the importance of routine eye care and follow-up appointments after CFB removal to monitor for residual foreign material or secondary complications. Additionally, educating patients on maintaining proper hygiene practices can help prevent infections, particularly if eye rubbing or contact lens use exacerbates the injury. By promoting awareness and proactive measures, clinicians can effectively reduce the risk of CFBs, enhance patient compliance, and improve visual outcomes.[75]
Pearls and Other Issues
When examining a patient with ocular trauma, finding a site of traumatic injury does not rule out additional CFBs elsewhere. Examinations should be conducted in a standard, routine, thorough, and meticulous manner. The upper eyelid should be flipped, and contact lenses must be removed before the examination.[76]
CFBs are a common ophthalmic emergency, but prompt recognition and proper management can prevent vision-threatening complications. Superficial CFBs are typically managed easily with removal under slit-lamp magnification, while deeper or metallic foreign bodies may require more specialized expertise. Disposition includes thorough patient education on follow-up care to monitor for delayed complications such as infections, corneal scarring, or rust rings.[58]
Key considerations include assessing for IOFBs through imaging, especially in cases involving high-velocity trauma. Removal of metallic CFBs requires meticulous attention to the associated rust ring, often necessitating the use of specialized burrs. Potential pitfalls include incomplete foreign body removal, leading to chronic irritation or secondary infections, and failure to recognize subtle indications of penetrating trauma or globe rupture.[77]
Prevention is critical and involves educating patients on the necessity of wearing protective eyewear during high-risk activities such as grinding, drilling, or working in construction. Adherence to occupational safety measures and raising awareness can significantly lower the occurrence of CFBs. Clinicians should stress the need for prompt medical evaluation if foreign body sensations persist. By incorporating key insights, addressing potential challenges, and emphasizing preventive strategies, healthcare providers can facilitate effective management and minimize long-term complications associated with CFB injuries.[61]
Enhancing Healthcare Team Outcomes
Some patients with a CFB typically interact and seek care from multidisciplinary healthcare providers, including primary care physicians, nurse practitioners, and optometrists, while others present directly to the emergency department. Emergency care providers play a crucial role in rapid triage. Nurses contribute by educating patients, ensuring comfort, and performing initial assessments. Nurses may identify signs such as an irregular pupil, take steps to protect the eye, such as covering it in suspected open globe injuries, and measure intraocular pressure to guide further evaluation. Ophthalmologists provide advanced interventions as needed, ensuring comprehensive care. This collaborative approach reduces long-term complications and improves patient outcomes. A retrospective chart review highlighted intraocular pressure as a factor influencing outcomes in open globe injury outcomes.[78]
Pharmacists play a crucial role by educating patients on using eye drops and other medications properly. They ensure appropriate pharmacological therapy, including antibiotic drops, analgesics, or cycloplegics, to reduce the risk of infection and alleviate discomfort. Once the initial stages of the condition are under control or stabilized, close follow-up with a specialist is vital to monitor recovery and prevent complications. Effective management of CFBs depends on well-coordinated interprofessional collaboration within the healthcare team to ensure timely intervention, provide comprehensive care, prioritize patient safety, minimize long-term sequelae, and achieve optimal visual outcomes.[79]
Physicians, particularly ophthalmologists and emergency department clinicians, play a central role in diagnosing and managing CFBs through prompt slit-lamp examinations and foreign body removal procedures. Nurses and advanced practitioners contribute by triaging patients, assessing symptoms such as pain and photophobia, and preparing necessary instruments for interventions.[80] Effective care coordination among multidisciplinary healthcare team members is vital, particularly for patients with retained or deep-seated foreign bodies requiring surgical intervention. Clear communication among the interprofessional healthcare team enhances patient-centered care by reducing delays, reinforcing post-procedural education on ocular hygiene, and ensuring timely follow-up to prevent complications such as infections or corneal scarring.[81]
Establishing standardized protocols for evaluating high-risk patients, especially those with IOFBs, enhances both safety and efficiency. Ethical considerations, such as obtaining informed consent, managing pain effectively, and providing patient reassurance, are integral to care. Leveraging the expertise of diverse healthcare professionals, interprofessional teams can improve outcomes, prioritize patient safety, and deliver comprehensive care for CFB injuries.[82]
Media
References
Xing X, Liu F, Qi Y, Li J, Yu B, Wan L. Clinical Characteristics and Prognostic Factors of Patients with Intraocular Foreign Bodies from a Tertiary Eye Center in North China. Clinical ophthalmology (Auckland, N.Z.). 2024:18():3635-3643. doi: 10.2147/OPTH.S492986. Epub 2024 Dec 7 [PubMed PMID: 39664783]
Level 2 (mid-level) evidenceWang T, Zhong L, Yin S, Bao T, Yang J, Wang T, Ling S. Comparison of Different Types of Corneal Foreign Bodies Using Anterior Segment Optical Coherence Tomography: A Prospective Observational Study. Journal of ophthalmology. 2020:2020():9108317. doi: 10.1155/2020/9108317. Epub 2020 Aug 11 [PubMed PMID: 32850143]
Level 2 (mid-level) evidenceOnkar A. Commentary: Tackling the corneal foreign body. Indian journal of ophthalmology. 2020 Jan:68(1):57-58. doi: 10.4103/ijo.IJO_1625_19. Epub [PubMed PMID: 31856467]
Level 3 (low-level) evidenceAkbaş E, Barut Selver Ö, Palamar M. Retrospective Evaluation of Corneal Foreign Bodies with Anterior Segment Optical Coherence Tomography. Turkish journal of ophthalmology. 2021 Oct 26:51(5):265-268. doi: 10.4274/tjo.galenos.2020.42223. Epub [PubMed PMID: 34702019]
Level 2 (mid-level) evidenceSafari S, McLaughlin CJ, Shah A, Kane BG. Prolonged Ocular Foreign Body Found on Repeat Visit to a Second Emergency Department. Cureus. 2023 Apr:15(4):e37819. doi: 10.7759/cureus.37819. Epub 2023 Apr 19 [PubMed PMID: 37214081]
Shah A, Blackhall K, Ker K, Patel D. Educational interventions for the prevention of eye injuries. The Cochrane database of systematic reviews. 2009 Oct 7:2009(4):CD006527. doi: 10.1002/14651858.CD006527.pub3. Epub 2009 Oct 7 [PubMed PMID: 19821372]
Level 1 (high-level) evidenceAziz MA, Rahman MA. Corneal foreign body--an occupational hazard. Mymensingh medical journal : MMJ. 2004 Jul:13(2):174-6 [PubMed PMID: 15284696]
Tran HM, Lai CH, Chen WL, Wang CC, Liang CW, Chien CY, Pan CH, Chuang KJ, Chuang HC. Effects of occupational exposure to metal fume PM(2.5) on lung function and biomarkers among shipyard workers: a 3-year prospective cohort study. International archives of occupational and environmental health. 2024 May:97(4):401-412. doi: 10.1007/s00420-024-02055-1. Epub 2024 Mar 13 [PubMed PMID: 38480609]
Kok JF, Parteli EJ, Michaels TI, Karam DB. The physics of wind-blown sand and dust. Reports on progress in physics. Physical Society (Great Britain). 2012 Oct:75(10):106901. doi: 10.1088/0034-4885/75/10/106901. Epub 2012 Sep 14 [PubMed PMID: 22982806]
Kyriakaki ED, Symvoulakis EK, Chlouverakis G, Detorakis ET. Causes, occupational risk and socio-economic determinants of eye injuries: a literature review. Medicine and pharmacy reports. 2021 Apr:94(2):131-144. doi: 10.15386/mpr-1761. Epub 2021 Apr 29 [PubMed PMID: 34013184]
Adar R, Bass A, Walden R. Iatrogenic complications in surgery. Five years' experience in general and vascular surgery in a University Hospital. Annals of surgery. 1982 Dec:196(6):725-9 [PubMed PMID: 7149826]
Gurnani B, Kaur K. Navigating the challenges of infective keratitis: A critical analysis of treatment and diagnostic approaches. Indian journal of ophthalmology. 2024 Aug 1:72(8):1227-1228. doi: 10.4103/IJO.IJO_706_24. Epub 2024 Jul 29 [PubMed PMID: 39078975]
Gurnani B, Kaur K. Anti-infective therapies for Pythium insidiosum keratitis. Expert review of anti-infective therapy. 2024 Oct:22(10):805-817. doi: 10.1080/14787210.2024.2403146. Epub 2024 Sep 13 [PubMed PMID: 39268901]
Gurnani B, Kaur K. Letter to the editor: Case series: Mixed infectious keratitis by Pythium insidiosum and fungal species. Optometry and vision science : official publication of the American Academy of Optometry. 2024 May 1:101(5):236. doi: 10.1097/OPX.0000000000002147. Epub [PubMed PMID: 38857033]
Level 2 (mid-level) evidenceBartholdson S, von Schreeb J. Natural Disasters and Injuries: What Does a Surgeon Need to Know? Current trauma reports. 2018:4(2):103-108. doi: 10.1007/s40719-018-0125-3. Epub 2018 Mar 23 [PubMed PMID: 29888166]
Passali D, Gregori D, Lorenzoni G, Cocca S, Loglisci M, Passali FM, Bellussi L. Foreign body injuries in children: a review. Acta otorhinolaryngologica Italica : organo ufficiale della Societa italiana di otorinolaringologia e chirurgia cervico-facciale. 2015 Oct:35(4):265-71 [PubMed PMID: 26824213]
Kowalik K, Gruszczyńska A, Knychalska K, Kaźmierczak K, Modrzejewski A. Non-metallic foreign bodies - diagnostic and therapeutic difficulties. Polski przeglad chirurgiczny. 2023 Oct 13:96(6):47-51. doi: 10.5604/01.3001.0016.3171. Epub [PubMed PMID: 39635744]
Ozkurt ZG, Yuksel H, Saka G, Guclu H, Evsen S, Balsak S. Metallic corneal foreign bodies: an occupational health hazard. Arquivos brasileiros de oftalmologia. 2014 Apr:77(2):81-3 [PubMed PMID: 25076469]
Heier JS, Enzenauer RW, Wintermeyer SF, Delaney M, LaPiana FP. Ocular injuries and diseases at a combat support hospital in support of Operations Desert Shield and Desert Storm. Archives of ophthalmology (Chicago, Ill. : 1960). 1993 Jun:111(6):795-8 [PubMed PMID: 8512480]
Level 2 (mid-level) evidenceAgrawal C, Girgis S, Sethi A, Sethi V, Konale M, Lokwani P, Sethi R. Etiological causes and epidemiological characteristics of patients with occupational corneal foreign bodies: A prospective study in a hospital-based setting in India. Indian journal of ophthalmology. 2020 Jan:68(1):54-57. doi: 10.4103/ijo.IJO_623_19. Epub [PubMed PMID: 31856466]
Level 2 (mid-level) evidenceJovanovic N, Peek-Asa C, Swanton A, Young T, Alajbegovic-Halimic J, Cavaljuga S, Nisic F. Prevalence and risk factors associated with work-related eye injuries in Bosnia and Herzegovina. International journal of occupational and environmental health. 2016 Oct:22(4):325-332 [PubMed PMID: 27813453]
Yang Y,Yang C,Zhao R,Lin L,Duan F,Lou B,Yuan Z,Lin X, Intraocular foreign body injury in children: clinical characteristics and factors associated with endophthalmitis. The British journal of ophthalmology. 2020 Jun; [PubMed PMID: 31554633]
Kamil S, Mohan RR. Corneal stromal wound healing: Major regulators and therapeutic targets. The ocular surface. 2021 Jan:19():290-306. doi: 10.1016/j.jtos.2020.10.006. Epub 2020 Oct 28 [PubMed PMID: 33127599]
Barrientez B, Nicholas SE, Whelchel A, Sharif R, Hjortdal J, Karamichos D. Corneal injury: Clinical and molecular aspects. Experimental eye research. 2019 Sep:186():107709. doi: 10.1016/j.exer.2019.107709. Epub 2019 Jun 22 [PubMed PMID: 31238077]
DelMonte DW, Kim T. Anatomy and physiology of the cornea. Journal of cataract and refractive surgery. 2011 Mar:37(3):588-98. doi: 10.1016/j.jcrs.2010.12.037. Epub [PubMed PMID: 21333881]
Vemuganti GK, Murthy SI, Das S. Update on pathologic diagnosis of corneal infections and inflammations. Middle East African journal of ophthalmology. 2011 Oct:18(4):277-84. doi: 10.4103/0974-9233.90128. Epub [PubMed PMID: 22224015]
Sheikh Z, Brooks PJ, Barzilay O, Fine N, Glogauer M. Macrophages, Foreign Body Giant Cells and Their Response to Implantable Biomaterials. Materials (Basel, Switzerland). 2015 Aug 28:8(9):5671-5701. doi: 10.3390/ma8095269. Epub 2015 Aug 28 [PubMed PMID: 28793529]
Wynn TA. Cellular and molecular mechanisms of fibrosis. The Journal of pathology. 2008 Jan:214(2):199-210 [PubMed PMID: 18161745]
Ung L, Chodosh J. Foundational concepts in the biology of bacterial keratitis. Experimental eye research. 2021 Aug:209():108647. doi: 10.1016/j.exer.2021.108647. Epub 2021 Jun 5 [PubMed PMID: 34097906]
Lim SA, Siatkowski RM, Farris BK. Functional visual loss in adults and children patient characteristics, management, and outcomes. Ophthalmology. 2005 Oct:112(10):1821-8 [PubMed PMID: 16140382]
Rauchman SH, Locke B, Albert J, De Leon J, Peltier MR, Reiss AB. Toxic External Exposure Leading to Ocular Surface Injury. Vision (Basel, Switzerland). 2023 Apr 3:7(2):. doi: 10.3390/vision7020032. Epub 2023 Apr 3 [PubMed PMID: 37092465]
Frings A, Geerling G, Schargus M. Red Eye: A Guide for Non-specialists. Deutsches Arzteblatt international. 2017 Apr 28:114(17):302-312. doi: 10.3238/arztebl.2017.0302. Epub [PubMed PMID: 28530180]
Gurnani B, Balamurugan S, Kanakath A, Kaur K, Gupta A, Chaudhary S. First clinical case series of frosted branch angiitis: A diagnostic algorithm is suggested. Clinical case reports. 2023 Sep:11(9):e7778. doi: 10.1002/ccr3.7778. Epub 2023 Aug 25 [PubMed PMID: 37636879]
Level 2 (mid-level) evidenceMicieli JA,Margolin E, A 30-year-old woman with vision loss and painful eye movements. CMAJ : Canadian Medical Association journal = journal de l'Association medicale canadienne. 2015 Jun 16; [PubMed PMID: 25869872]
Bhargava M, Bhambhani V, Sen A, Johri A. Corneal foreign body post laser in-situ keratomileusis: Diagnosis, management, outcome and review of literature. American journal of ophthalmology case reports. 2024 Jun:34():102038. doi: 10.1016/j.ajoc.2024.102038. Epub 2024 Mar 14 [PubMed PMID: 38532848]
Level 3 (low-level) evidenceDang DH, Riaz KM, Karamichos D. Treatment of Non-Infectious Corneal Injury: Review of Diagnostic Agents, Therapeutic Medications, and Future Targets. Drugs. 2022 Feb:82(2):145-167. doi: 10.1007/s40265-021-01660-5. Epub 2022 Jan 13 [PubMed PMID: 35025078]
Martin R. Cornea and anterior eye assessment with slit lamp biomicroscopy, specular microscopy, confocal microscopy, and ultrasound biomicroscopy. Indian journal of ophthalmology. 2018 Feb:66(2):195-201. doi: 10.4103/ijo.IJO_649_17. Epub [PubMed PMID: 29380757]
Shan J, DeBoer C, Xu BY. Anterior Segment Optical Coherence Tomography: Applications for Clinical Care and Scientific Research. Asia-Pacific journal of ophthalmology (Philadelphia, Pa.). 2019 MarchApril 01:8(2):146-157. doi: 10.22608/APO.201910. Epub [PubMed PMID: 31020820]
He M, Wang D, Jiang Y. Overview of Ultrasound Biomicroscopy. Journal of current glaucoma practice. 2012 Jan-Apr:6(1):25-53 [PubMed PMID: 27990069]
Level 3 (low-level) evidenceLoBue TD, Deutsch TA, Lobick J, Turner DA. Detection and localization of nonmetallic intraocular foreign bodies by magnetic resonance imaging. Archives of ophthalmology (Chicago, Ill. : 1960). 1988 Feb:106(2):260-1 [PubMed PMID: 3341985]
Bodne D, Quinn SF, Cochran CF. Imaging foreign glass and wooden bodies of the extremities with CT and MR. Journal of computer assisted tomography. 1988 Jul-Aug:12(4):608-11 [PubMed PMID: 3392261]
Bartlett KJ, Vo AP, Rueckert J, Wojewoda C, Steckel EH, Stinnett-Donnelly J, Repp AB. Promoting appropriate utilisation of laboratory tests for inflammation at an academic medical centre. BMJ open quality. 2020 Feb:9(1):. doi: 10.1136/bmjoq-2019-000788. Epub [PubMed PMID: 32098777]
Level 2 (mid-level) evidenceGurnani B, Kaur K. Intricacies and solutions for interpretation of microbiologic samples of Pythium insidiosum keratitis. Indian journal of ophthalmology. 2024 Apr 1:72(4):602-603. doi: 10.4103/IJO.IJO_1573_23. Epub 2024 Mar 28 [PubMed PMID: 38546474]
Knoop K, Trott A. Ophthalmologic procedures in the emergency department--Part III: Slit lamp use and foreign bodies. Academic emergency medicine : official journal of the Society for Academic Emergency Medicine. 1995 Mar:2(3):224-30 [PubMed PMID: 7497039]
Varghese AP, Naik S, Asrar Up Haq Andrabi S, Luharia A, Tivaskar S. Enhancing Radiological Diagnosis: A Comprehensive Review of Image Quality Assessment and Optimization Strategies. Cureus. 2024 Jun:16(6):e63016. doi: 10.7759/cureus.63016. Epub 2024 Jun 24 [PubMed PMID: 39050319]
Level 2 (mid-level) evidenceContreras-Salinas H, Orozco-Ceja V, Romero-López MS, Barajas-Virgen MY, Baiza-Durán LM, Rodríguez-Herrera LY. Ocular Cyclopentolate: A Mini Review Concerning Its Benefits and Risks. Clinical ophthalmology (Auckland, N.Z.). 2022:16():3753-3762. doi: 10.2147/OPTH.S388982. Epub 2022 Nov 15 [PubMed PMID: 36411874]
Sharma A, Sharma R. Removal of full-thickness vertical corneal stromal wooden foreign bodies: An innovative ab-interno technique. Indian journal of ophthalmology. 2021 Apr:69(4):971-973. doi: 10.4103/ijo.IJO_2397_20. Epub [PubMed PMID: 33727468]
Beyer H, Cherkas D. Corneal foreign body removal using a bent needle tip. The American journal of emergency medicine. 2012 Mar:30(3):489-90. doi: 10.1016/j.ajem.2010.12.038. Epub 2011 Feb 26 [PubMed PMID: 21354749]
Ahmed F, House RJ, Feldman BH. Corneal Abrasions and Corneal Foreign Bodies. Primary care. 2015 Sep:42(3):363-75. doi: 10.1016/j.pop.2015.05.004. Epub 2015 Jul 31 [PubMed PMID: 26319343]
Macedo Filho ET, Lago A, Duarte K, Liang SJ, Lima AL, Freitas Dd. Superficial corneal foreign body: laboratory and epidemiologic aspects. Arquivos brasileiros de oftalmologia. 2005 Nov-Dec:68(6):821-3 [PubMed PMID: 17344985]
Menghini M, Knecht PB, Kaufmann C, Kovacs R, Watson SL, Landau K, Bosch MM. Treatment of traumatic corneal abrasions: a three-arm, prospective, randomized study. Ophthalmic research. 2013:50(1):13-8. doi: 10.1159/000347125. Epub 2013 May 3 [PubMed PMID: 23652196]
Level 1 (high-level) evidenceCollins S, White J, Ramsay M, Amirthalingam G. The importance of tetanus risk assessment during wound management. IDCases. 2015:2(1):3-5. doi: 10.1016/j.idcr.2014.11.003. Epub 2014 Dec 10 [PubMed PMID: 26793439]
Level 3 (low-level) evidenceEbrahimi A, Radmanesh M, Rabiei S, Kavoussi H. Surgical removal of neglected soft tissue foreign bodies by needle-guided technique. Iranian journal of otorhinolaryngology. 2013 Winter:25(70):29-36 [PubMed PMID: 24303416]
Leekha S, Terrell CL, Edson RS. General principles of antimicrobial therapy. Mayo Clinic proceedings. 2011 Feb:86(2):156-67. doi: 10.4065/mcp.2010.0639. Epub [PubMed PMID: 21282489]
Matalia HP, Nandini C, Matalia J. Surgical technique for the management of corneal perforation in brittle cornea. Indian journal of ophthalmology. 2021 Sep:69(9):2521-2523. doi: 10.4103/ijo.IJO_2542_20. Epub [PubMed PMID: 34427257]
Chen YC, Hsiao YT, Kuo SF, Yu HJ, Fang PC, Ho RW, Yang IH, Kuo MT. Monitoring the transition from corneal ulceration to healed scar using a Scheimpflug tomography-based densitometry. Graefe's archive for clinical and experimental ophthalmology = Albrecht von Graefes Archiv fur klinische und experimentelle Ophthalmologie. 2024 Jul:262(7):2189-2198. doi: 10.1007/s00417-024-06390-4. Epub 2024 Feb 13 [PubMed PMID: 38349421]
Gower EW, Lindsley K, Tulenko SE, Nanji AA, Leyngold I, McDonnell PJ. Perioperative antibiotics for prevention of acute endophthalmitis after cataract surgery. The Cochrane database of systematic reviews. 2017 Feb 13:2(2):CD006364. doi: 10.1002/14651858.CD006364.pub3. Epub 2017 Feb 13 [PubMed PMID: 28192644]
Level 1 (high-level) evidenceQuirke M, Mullarkey C, Askoorum S, Coffey N, Binchy J. A prospective observational study of techniques to remove corneal foreign body in the emergency department. Emergency medicine journal : EMJ. 2014 Jun:31(6):463-6. doi: 10.1136/emermed-2012-201447. Epub 2013 Mar 29 [PubMed PMID: 23543227]
Level 2 (mid-level) evidenceMorales-Wong F, Navas A, Yañez-Oviedo GE, Mohamed-Noriega K. Femtosecond laser applications in corneal surgery. Taiwan journal of ophthalmology. 2023 Jul-Sep:13(3):293-305. doi: 10.4103/tjo.TJO-D-23-00083. Epub 2023 Sep 8 [PubMed PMID: 38089509]
Ljubimov AV, Saghizadeh M. Progress in corneal wound healing. Progress in retinal and eye research. 2015 Nov:49():17-45. doi: 10.1016/j.preteyeres.2015.07.002. Epub 2015 Jul 18 [PubMed PMID: 26197361]
AlMahmoud T, Elkonaisi I, Grivna M, Abu-Zidan FM. Personal protective eyewear usage among industrial workers in small-scale enterprises. Injury epidemiology. 2020 Sep 22:7(1):54. doi: 10.1186/s40621-020-00280-z. Epub 2020 Sep 22 [PubMed PMID: 32958044]
Zheng Y, Zhai CB. Performance of Bandage Contact Lens in Patients Post-ocular Surgeries: A Systematic Literature Review. Eye & contact lens. 2023 Nov 1:49(11):449-458. doi: 10.1097/ICL.0000000000001021. Epub 2023 Oct 9 [PubMed PMID: 37816246]
Level 1 (high-level) evidenceHe N, Lv Z. A rare asymptomatic metallic intraocular foreign body retained in the anterior chamber for 15 years: A case report. Medicine. 2021 Jun 25:100(25):e26470. doi: 10.1097/MD.0000000000026470. Epub [PubMed PMID: 34160455]
Level 3 (low-level) evidenceGumus K, Karakucuk S, Mirza E. Corneal injury from a metallic foreign body: an occupational hazard. Eye & contact lens. 2007 Sep:33(5):259-60 [PubMed PMID: 17873630]
Dua HS, Ting DSJ, Al Saadi A, Said DG. Chemical eye injury: pathophysiology, assessment and management. Eye (London, England). 2020 Nov:34(11):2001-2019. doi: 10.1038/s41433-020-1026-6. Epub 2020 Jun 22 [PubMed PMID: 32572184]
Keeney AH. Evaluation and management of corneal foreign bodies. The Journal of family practice. 1975 Oct:2(5):381-4 [PubMed PMID: 1206368]
Goel N, Pangtey BP, Raina UK, Ghosh B. Anterior segment optical coherence tomography in intracorneal foreign body. Oman journal of ophthalmology. 2012 May:5(2):131-2 [PubMed PMID: 22993475]
Sharma A, Sharma R. Retrieval of deep corneal stromal wooden foreign body using vitreoretinal foreign body forceps as scoop: An innovative technique. Indian journal of ophthalmology. 2023 Dec 1:71(12):3718-3720. doi: 10.4103/IJO.IJO_801_23. Epub 2023 Nov 20 [PubMed PMID: 37991311]
Zhou Y, DiSclafani M, Jeang L, Shah AA. Open Globe Injuries: Review of Evaluation, Management, and Surgical Pearls. Clinical ophthalmology (Auckland, N.Z.). 2022:16():2545-2559. doi: 10.2147/OPTH.S372011. Epub 2022 Aug 10 [PubMed PMID: 35983163]
El-Asrar AM, Al-Amro SA, Khan NM, Kangave D. Retinal detachment after posterior segment intraocular foreign body injuries. International ophthalmology. 1998:22(6):369-75 [PubMed PMID: 10937853]
Algarni AM, Guyatt GH, Turner A, Alamri S. Antibiotic prophylaxis for corneal abrasion. The Cochrane database of systematic reviews. 2022 May 27:5(5):CD014617. doi: 10.1002/14651858.CD014617.pub2. Epub 2022 May 27 [PubMed PMID: 35622535]
Level 1 (high-level) evidenceAgarwal R, Tripathi A. Current Modalities for Low Vision Rehabilitation. Cureus. 2021 Jul:13(7):e16561. doi: 10.7759/cureus.16561. Epub 2021 Jul 22 [PubMed PMID: 34466307]
Ohlhausen M, Menke BA, Begley J, Kim S, Debiec MR, Conrady CD, Yeh S, Justin GA. Advances in the management of intraocular foreign bodies. Frontiers in ophthalmology. 2024:4():1422466. doi: 10.3389/fopht.2024.1422466. Epub 2024 Sep 2 [PubMed PMID: 39285858]
Level 3 (low-level) evidenceOwens JK, Scibilia J, Hezoucky N. Corneal foreign bodies--first aid, treatment, and outcomes. Skills review for an occupational health setting. AAOHN journal : official journal of the American Association of Occupational Health Nurses. 2001 May:49(5):226-30 [PubMed PMID: 11760304]
Keel S, Müller A, Block S, Bourne R, Burton MJ, Chatterji S, He M, Lansingh VC, Mathenge W, Mariotti S, Muirhead D, Rabiu MM, Ravilla TD, Resnikoff S, Silva JC, Tapply I, Vos T, Wang N, Cieza A. Keeping an eye on eye care: monitoring progress towards effective coverage. The Lancet. Global health. 2021 Oct:9(10):e1460-e1464. doi: 10.1016/S2214-109X(21)00212-6. Epub 2021 Jul 5 [PubMed PMID: 34237266]
Mutie D, Mwangi N. Assessing an eye injury patient. Community eye health. 2015:28(91):46-8 [PubMed PMID: 26989310]
Jung HC,Lee SY,Yoon CK,Park UC,Heo JW,Lee EK, Intraocular Foreign Body: Diagnostic Protocols and Treatment Strategies in Ocular Trauma Patients. Journal of clinical medicine. 2021 Apr 25 [PubMed PMID: 33923011]
Margo JA, Feldman S, Addis H, Bodanapally UK, Ellish N, Saeedi O. Open Globe Injuries Presenting With Normal or High Intraocular Pressure. Eye & contact lens. 2016 Jul:42(4):256-61. doi: 10.1097/ICL.0000000000000188. Epub [PubMed PMID: 26372477]
Siempis T. Urgent Eye Care in the UK Increased Demand and Challenges for the Future. Medical hypothesis, discovery & innovation ophthalmology journal. 2014 Winter:3(4):103-10 [PubMed PMID: 25756059]
Newell SW. Management of corneal foreign bodies. American family physician. 1985 Feb:31(2):149-56 [PubMed PMID: 3883720]
Dickerson LM, Mainous AG 3rd, Carek PJ. The pharmacist's role in promoting optimal antimicrobial use. Pharmacotherapy. 2000 Jun:20(6):711-23 [PubMed PMID: 10853627]
Long KL, Ingraham AM, Wendt EM, Saucke MC, Balentine C, Orne J, Pitt SC. Informed Consent and Informed Decision-Making in High-Risk Surgery: A Quantitative Analysis. Journal of the American College of Surgeons. 2021 Sep:233(3):337-345. doi: 10.1016/j.jamcollsurg.2021.05.029. Epub 2021 Jun 5 [PubMed PMID: 34102279]