Introduction
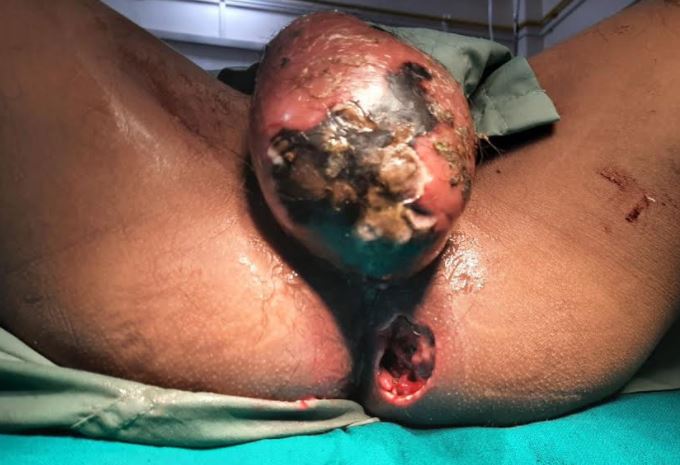
Fournier gangrene is a rare but rapidly progressive form of necrotizing fasciitis that affects the deep and superficial tissues of the perineal, anal, scrotal, and genital regions. Named after Dr Alfred Fournier, a French dermatology and venereal specialist, it was initially described in 1883 as necrotizing fasciitis of the external genitalia, perineal, and perianal regions involving 5 of his patients.[1][2] Named after Dr Alfred Fournier, a French dermatology and venereal specialist, Fournier gangrene was first described in 1883 as "necrotizing fasciitis" of the external genitalia, perineal, and perianal regions in 5 of his patients. The disease involves the rapid spread of severe inflammatory and infectious processes along fascial planes, affecting adjacent soft tissue. Fournier gangrene may go unnoticed or unrecognized in its early stages due to minimal or absent skin manifestations (see Image. Fournier Gangrene).[2][3]
Fournier gangrene is often associated with general signs of sepsis, rapid tissue destruction, and a high fatality rate of 40%.[4][5] The spread of inflammation and infection leads to thrombosis of blood vessels, which in turn causes ischemia and tissue necrosis of the adjacent soft tissue and fascia.[6] The infectious and inflammatory process spreads quickly along the Dartos, Colles, and Scarpa fascias, allowing for the early involvement of the abdominal wall.[6] Due to initial fascial and subcutaneous involvement, clinicians may miss this disease in its early stages, as the overlying soft tissue may appear unremarkable or resemble simple cellulitis.[7][8] Early diagnosis and treatment of this potentially fatal disease are crucial, as it can easily be misdiagnosed in its early stages as a benign condition.[2][3][8][9][10]
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
Fournier gangrene results from a polymicrobial aerobic and anaerobic synergistic infection of the fascia and subcutaneous soft tissue. Wound cultures from Fournier gangrene patients commonly grow a mix of gram-positive bacteria, such as group A Streptococcus and Staphylococcus aureus, and gram-negative bacteria, such as Escherichia coli and Pseudomonas aeruginosa, reflecting the polymicrobial nature of the infection.[11][12] These bacteria can be introduced through several sources, including urinary, bowel, or dermal. Urinary tract infections and other infectious processes of the perineum, such as perianal abscesses or even a simple pimple, may also provide a starting point for the infection.[6]
Surgical manipulation of the genital and perineal area can provide the initial insult needed to develop Fournier gangrene.[6][7] Any traumatic injury or localized skin breakdown in the perineum or scrotum can allow bacteria to access the subcutaneous tissues, which initiates the infection and ultimately results in Fournier gangrene.[3][13][14][15] About 25% of cases have no known or identifiable etiology.[16]
The use of sodium-glucose cotransporter-2 (SGLT2) inhibitors has been linked to Fournier gangrene, although this association remains controversial.[17][18][19] If Fournier gangrene is suspected in users of these medications, the drugs should be discontinued, and treatment for the underlying infection should be initiated immediately.[17]
Epidemiology
Fournier gangrene is a rare infection, accounting for less than 0.02% of all hospital admissions. This condition has a strong male predilection, with a male-to-female ratio of 10:1, although women tend to experience higher morbidity and mortality rates.[20][21][22] The incidence in males is 1.6 cases per 100,000 men.[12][23]
Fournier gangrene most commonly affects men aged 50 to 79, with an incidence of 3.3 cases per 100,000 men.[12][23] The southeastern United States has the highest reported rate of Fournier gangrene at 1.9 cases per 100,000 population.[24] These frequencies appear relatively constant among patients in the United States and worldwide.[24] Although less common in females, women tend to present with more severe illness. They are twice as likely to require mechanical ventilation and dialysis, have a longer average hospital stay, and experience a higher fatality rate compared to male patients.[22][24]
Although Fournier gangrene can occur in healthy individuals (26% to 30%), it is typically associated with a debilitated or immunocompromised state. This condition most commonly affects males aged 50 or older with diabetes and a history of alcohol abuse.[5][25] Patients with multiple comorbidities generally tend to have worse outcomes.[5]
Known risk factors for Fournier gangrene include:
- Atherosclerosis
- Chemotherapy [7]
- Chronic alcohol abuse (25% to 50% of cases)
- Chronic steroid use
- Colorectal malignancy
- Diabetes (20% to 70% of cases) [26]
- Drug abuse (especially if injected directly into inguinal veins or the penis)
- HIV infection [27]
- Immunosuppression
- Inflammatory bowel disease
- Leukemia [28]
- Liver failure and cirrhosis
- Male gender (90% of cases)
- Malnutrition
- Neurogenic bladder [28]
- Obesity
- Perianal abscess
- Peripheral vascular disease
- Prostate cancer
- Recent trauma or surgery (prostate biopsy, catheterization, and cystoscopy) [29]
- Rectal fistula
- Renal failure
- Significant cardiac disease [30]
- Spinal cord injury
- Urethral strictures
- Use of SGLT2 inhibitors (glycosuric medications used in patients with diabetes) [31]
Despite worldwide advances in sepsis treatment, the mortality rate for Fournier gangrene has remained stable at approximately 40%.[5][32][33] Delayed diagnosis and treatment significantly contribute to this high mortality rate, with delays increasing the death rate to 88%.[11][25][33] Time to surgical intervention is the most critical factor influencing mortality, as early surgery can reduce the death rate by half.[11][34][35] Severe diabetes, heart disease, and renal failure significantly increase the mortality rate.[16]
Pathophysiology
The pathophysiology of Fournier gangrene involves a synergistic infection caused by anaerobic and aerobic bacteria. The bacterial infection typically begins with an initial insult, such as a urinary tract infection, perineal abscess, localized cellulitis, recent surgical manipulation of the genital or perineal area, or even a minor scratch or pimple. The synergistic activity of the bacterial infection produces tissue-destructive enzymes, collagenases, and endotoxins, leading to obliterative endarteritis with microthromboses of subcutaneous vessels.[36][37] This results in ischemic gangrene of the affected structures and rapid spread of the infection to adjacent and surrounding tissues.[36][37] The infectious process can spread as fast as 1 inch every hour.[38]
Histopathology
The diagnosis of Fournier gangrene is typically based on a combination of imaging, history, and physical examination. In some cases, a biopsy may be performed to differentiate Fournier gangrene from severe cellulitis. Histopathology of Fournier gangrene typically reveals ulceration of the epidermis, neutrophilic exudate, thrombosed vessels, and necrosis.[39]
History and Physical
Patients with Fournier gangrene typically present with pain in the perineal or genital areas. Early signs may be minimal or subtle, with symptoms intensifying as the condition progresses. Clinicians should remain suspicious of any infection or cellulitis in the perineal or scrotal regions, particularly if the pain is disproportionate to the visible lesion.[6] Infections that appear simple can quickly progress and lead to life-threatening complications. Patients often have a medical history of diabetes mellitus, hypertension, malignancy, or alcohol abuse—risk factors for Fournier gangrene, in addition to being male.[14] Approximately half of all patients with Fournier gangrene have diabetes.[40][41][42]
Patients may also report being immunocompromised, having recently experienced trauma to the area, or undergoing recent surgeries. They may describe redness and swelling in the perineum, scrotum, and genital areas, along with systemic symptoms such as fever, chills, nausea, vomiting, urinary retention, and malaise.[43]
The earliest signs of a possible Fournier gangrene include itching, localized tenderness, edema, and erythema involving the skin of the perineum, scrotum, or labia.[12] These symptoms can easily be confused with more common, simple infections like cellulitis, erysipelas, and impetigo. These benign infections typically have sharp, demarcated borders, while Fournier gangrene often presents with sporadic bulla formation, diffuse edema, and patchy erythema.[8][44] Evidence of abrasions or fluctuance may also be present, though these are usually observed later. In a study, the most common symptom was scrotal swelling (79%), followed by tachycardia (61%), purulent drainage (60%), crepitus (54%), and fever (41%).[45]
In some patients, the earliest sign of Fournier gangrene may be a black perineal skin lesion, which should be considered suspicious for possible early Fournier gangrene.[46] While classically considered a male disease, the incidence of Fournier gangrene in women is increasing.[45] The typical presentation in females involves labial or vulvar cellulitis, with women being more likely to be morbidly obese compared to similarly affected men.[45] Early diagnosis of Fournier gangrene can be challenging, as 40% of patients may present with no symptoms, and up to 75% of cases are initially misdiagnosed, contributing to its persistently high mortality rate.[4][40][47]
Severe pain out of proportion to the physical findings is a classic finding of Fournier gangrene.[12] Additional signs such as crepitation on palpation, purpura, bullae, and patchy black tissue discoloration may appear as the infection progresses.[40] The presence of subcutaneous gas and crepitus often indicates the presence of gas-forming organisms such as Clostridia.[48] The infection spreads along the fascial planes, with erythema and tenderness extending into the anterior abdominal wall.[49] As the infection advances, the skin may turn dusky and emit a musty or putrid odor, primarily due to anaerobic bacterial activity, typically caused by Clostridia.[12]
The area of involvement may extend beyond the visible margins of the affected skin. Late-stage signs include obvious sepsis, shock, hypotension, tachycardia, fever, tachypnea, and organ dysfunction.[12][50] In severe cases, the infection can progress as far as the clavicles.[51] The testicles, spermatic cord structures, urethra, and corpora cavernosa are typically spared unless they were initially involved as the original infection source.[7]
Although typically an acute and rapidly progressive condition, Fournier gangrene can occasionally present more gradually over days or even weeks. On average, the typical case progresses from the onset of the first symptom to hospital admission within about 5 days.[52]
The natural history and presentation of Fournier gangrene have been described as 5 stages:
- Prodromal symptoms: These include lethargy and fever, which may persist from 2 to 7 days.
- Genital tenderness and pain: The overlying skin becomes edematous.
- Intense genital pain and tenderness: Increased erythema of the skin.
- Subcutaneous crepitation: This is evident, and the overlying skin appears dusky.
- Purulent drainage: This may be present, with clear signs of gangrene affecting a portion of the affected area.[53]
Extra attention to the physical examination of the genitalia and perineum is necessary for certain patient groups, as these areas may be examined infrequently. These groups include:
Evaluation
The diagnosis of Fournier gangrene is primarily clinical but can be supported by a combination of blood work and imaging. Clinicians should maintain a high index of suspicion for any inflammatory or infectious process involving the perineum or genitalia, especially in older male patients with diabetics and other patients at increased risk.
Blood work for suspected Fournier gangrene should include a complete blood count (CBC) with differential and a comprehensive metabolic panel (CMP). The CBC often shows an elevated white blood cell count (WBC) with a potential left shift. The CMP may reveal electrolyte abnormalities such as hyponatremia or metabolic acidosis, as well as signs of concurrent renal failure. Serum lactate, C-reactive protein (CRP), and procalcitonin can help assess for associated bacteremia and sepsis.[56] Arterial blood gases may be obtained to evaluate oxygenation and acid/base status, while blood and wound cultures are essential to guide antibiotic therapy.[57][58]
While Fournier gangrene is primarily a clinical diagnosis, imaging can help confirm the disease process and assess the extent of involvement. However, imaging alone cannot establish or rule out the diagnosis of Fournier gangrene and should not delay surgical intervention, especially in hemodynamically unstable patients.[59]
Ultrasound Imaging
Ultrasound is valuable for visualizing subcutaneous gas or emphysema in the underlying soft tissue. This imaging technique may also reveal thickened scrotal walls with linear hypoechoic fluid streaks and increased blood flow. Ultrasound imaging is quick, can detect subcutaneous gas before it is apparent on physical examination, and is particularly useful for evaluating the scrotum.[60] The presence of gas in the scrotum is considered a pathognomonic sign of Fournier gangrene.[61] Ultrasound can also assess edema, gas, increased subcutaneous fluid, enhanced vascularity on color Doppler, and the thickness of affected soft tissue.[49][62][63]
Other typical ultrasonographic findings include "cobblestoning" (individual subcutaneous fat globules surrounded by fluid), the "snow globe" effect (a swirling appearance of heterogeneous subcutaneous material), and "dirty shadowing" (a hazy appearance of infected subcutaneous tissue caused by gas shadowing and reverberation artifacts from hyperechoic foci).[12][49][61][62][64] These findings can help differentiate Fournier gangrene from other, more benign infections.[62]
X-Ray Imaging
X-ray imaging of the affected area may reveal subcutaneous gas, which is present in 90% of all Fournier gangrene cases.[47] Standard x-rays can detect soft tissue gas or emphysema, typically following fascial planes, and may be visible before crepitus is detected on physical examination.[12] While the presence of subcutaneous emphysema is helpful, a negative x-ray should not rule out a diagnosis of Fournier gangrene.[12]
Computed Tomography Imaging
Computed tomography (CT) has demonstrated high sensitivity (88.5%) and specificity (93.3%) for diagnosing Fournier gangrene.[65] CT is the most sensitive and specific imaging modality for diagnosing Fournier gangrene. Typical CT findings include fat stranding around affected structures, subcutaneous emphysema, abscess formation, asymmetrical fascial thickening, and abnormal fluid collections.[64][66][67][68][69]
CT scans are also valuable for identifying the source of scrotal gas and excluding other intra- and retroperitoneal disease processes.[70][71] CT scans are also recommended after surgery to identify new pockets of infection and assess wound healing. While CT should not delay surgery in clear-cut cases, it does not appear to influence the timing of surgical intervention in real-life clinical settings.[72]
Magnetic Resonance Imaging Scans
Magnetic resonance imaging (MRI) provides excellent soft-tissue imaging but is not recommended for the initial diagnosis of suspected Fournier gangrene due to the extended imaging time and high cost.[45][48] Despite this, MRI is considered the gold standard imaging for soft-tissue pathology, including Fournier gangrene.[73]
The presence of gas on imaging is highly specific for Fournier gangrene but has limited sensitivity, with a rate of only 49%.[12][65] This is due to the gas being difficult to visualize in the deep fascia or spreading too thinly, which can lead to a false-negative result.[67]
In cases where the diagnosis is clear and the patient is unstable or septic, surgical treatment should be initiated immediately without waiting for confirmatory imaging or laboratory results. In uncertain cases, it is better to proceed with surgery, even if it later proves unnecessary, rather than delay the procedure and risk allowing a life-threatening infection to progress.
Treatment / Management
Fournier gangrene is a true surgical emergency, requiring both surgical intervention and medical resuscitation, as patients are often septic and in shock.[43] (B3)
Medical management begins with the initiation of empiric broad-spectrum antibiotics while awaiting culture results. Historically, antibiotic therapy has involved triple therapy to cover the gram-positive, gram-negative, and anaerobic organisms commonly associated with Fournier gangrene. These include Staphylococcus, Streptococcus, coliforms, Pseudomonas, Bacteroides, Clostridium, and possibly yeast.[48] A typical combination includes a third-generation cephalosporin, aminoglycoside, penicillin, and metronidazole. Antibiotic therapy generally continues for a duration of at least 2 weeks.
Current Recommended Antibiotic Regimens for Fournier Gangrene
The following antibiotic regimens are currently recommended for the treatment of Fournier gangrene:
- Carbapenems
- Imipenem or meropenem: This should be administered 1 g via the intravenous (IV) route every 6 to 8 hours.
- Ertapenem: This should be administered 1 g IV every 24 hours.[12]
(B3)
OR
- Piperacillin-tazobactam: This should be administered 3.375 g IV every 6 hours or 4.5 g IV every 8 hours.[44]
PLUS
- Clindamycin: This should be administered 600 to 900 mg IV every 8 hours.
PLUS
Daptomycin or linezolid can be used as alternatives to vancomycin.[12] Additionally, antifungal agents such as amphotericin B, fluconazole, or similar options may be added if indicated.[44] Alternate regimens may include aminoglycosides or fluoroquinolones combined with metronidazole.[44] For patients with exposure to fresh or saltwater, doxycycline can be added to cover Aeromonas hydrophila and Vibrio vulnificus.[44][61](B3)
In addition to antibiotic therapy, fluid resuscitation is crucial for patients who may present with hypotension and septic shock.[74][75] Vasopressors may be required to support resuscitation if hypotension does not respond to fluids alone.[75] Electrolyte abnormalities should be corrected, ideally using a balanced crystalloid such as Lactated Ringer solution.[12][75][76][77] Diabetic patients with Fournier gangrene also need to have any blood glucose abnormalities corrected.[66] (B3)
While antibiotic therapy and resuscitation are critical, they should not delay emergent, early, and aggressive surgical exploration and debridement, which remain the definitive and essential treatment for Fournier gangrene. Any significant delay in initiating surgery will lead to increased morbidity and mortality for the patient.[4][34][78](B2)
Surgical intervention involves aggressive, radical, wide resection of all necrotic and gangrenous tissue. The surgical team may include urology, general surgery, plastic surgery, colorectal surgery, and OB-GYN, depending on the specifics of the case. If there is any uncertainty about which specialty should lead, it is crucial for all relevant surgical specialties to be present in the operating room. If the urethra is affected and a suprapubic tube is required, or if the gangrene is confined to the scrotum and genitalia, urology would typically be the primary surgical service.
If the infection originates in the scrotum but extends into the lower abdomen and perineum, and then approaches the rectum, or if a diverting colostomy is necessary, general or colorectal surgery should be involved. However, these considerations should not delay the initiation of surgical treatment.
A shorter time from initial hospital presentation to surgical intervention has been associated with improved prognosis; therefore, efforts should be made to minimize this time and avoid delays.[4][34] Any initial delay of more than 12 hours, or even incremental delays of 3 hours, increases patient mortality.[79] (B2)
Surgical Debridement
Surgical debridement involves removing all dead, infected, and necrotic tissue. The procedure is guided by the separation of the skin and subcutaneous tissue, with debridement stopping when these tissues can no longer be easily separated. The extent of necrosis and the area requiring debridement often surpass the visible skin demarcation. In some cases, removal or excision of otherwise healthy skin—particularly in the scrotum—may be necessary to ensure full exposure and prevent premature skin closure before the underlying tissues have sufficiently healed.
Other specialties involved in these complex cases include anesthesiology, critical care, emergency medicine, endocrinology, infectious disease, internal medicine (hospitalists), nephrology, and wound care.
The testicles have a separate blood supply via the spermatic cord, so they are typically spared, even with extensive scrotal involvement.[59] In such cases, the testicles can be temporarily placed in a subcutaneous pouch, often created in the upper inner thighs, to help preserve their function and surface hydration. Permanent localization of the testicles can be achieved using a scrotal advancement flap, though long-term complications are minimized by utilizing a pudendal thigh flap for one or both sides.[5][80][81](B2)
The penile corpora cavernosa and urethra are usually preserved, although the penile skin may become involved.[82](B3)
Surgical debridement is typically performed in stages, with severe cases of Fournier gangrene often requiring 3 separate procedures.[66][83] A vacuum-assisted closure (VAC) system dressing is frequently used following debridement and reconstruction procedures to minimize fluid accumulation, reduce skin defects, and promote tissue healing.[39][84][85][86][87] This enhancement is based on applying subatmospheric pressure to the tissue for extended periods, facilitating debridement and enhancing healing.[66][88][87](B2)
Following surgical debridement and the formation of granulation tissue, patients require reconstructive surgery of the affected area. The extent of skin involvement determines the approach, which may include one or more of the following—skin flaps or grafts using local tissue, stem cell therapy, and/or split-thickness skin grafting.
Patients with significant perineal involvement often require a colostomy or fecal management system for fecal diversion to support local healing. Fecal management systems are based on bowel management catheters, which involve inserting a catheter into the rectum, using a syringe for irrigation, and connecting a collection bag. A diverting colostomy is indicated when the infectious process originates from the anorectal area and extends to the anal sphincter. Other indications include rectal perforation, large rectal wounds, or systemic sepsis.
A diverting colostomy is often performed using the Trephine technique, which involves using a flexible sigmoidoscope to transilluminate and locate the sigmoid colon. The stoma site is determined intraoperatively. After performing the trephine, the colon is held in place as the sigmoidoscope is withdrawn. The colon is then delivered into the wound, and an end colostomy is formed. Fecal management systems are associated with a shorter length of hospitalization (24.1 days) compared to colostomy (40.5 days).[89][90][91] However, a diverting colostomy is typically associated with a poorer prognosis and has not been shown to reduce mortality.[92][93] Therefore, its use should be considered carefully based on individual patient circumstances, disease severity, the degree of rectal or anal damage, and sphincter involvement.(A1)
The use of hyperbaric oxygen, topical therapy, immunotherapy, and therapeutic plasma exchange are potential adjunctive treatments for Fournier gangrene. However, medical management and, most importantly, surgical intervention remain the primary approaches. Hyperbaric oxygen therapy is a supplemental postoperative treatment typically used after initial surgical debridement. Evidence suggests that it improves survival and reduces morbidity.[94][95][96][97][98][99] (A1)
Hyperbaric oxygen therapy improves tissue oxygenation, enhancing antibiotic delivery, efficacy, and wound healing.[94] Although some reports suggest an increased mortality rate in Fournier gangrene patients receiving hyperbaric oxygen, this is typically linked to its use in the most severe cases.[100][101] Hyperbaric therapy should be reserved for postoperative use and must never delay surgical intervention.[100](A1)
The application of honey to the affected areas has also been reported to improve wound healing, although no studies have validated this therapy to date.[47][66][102] IV immunoglobulins have been proposed to help neutralize streptococcal toxins, but data supporting their effectiveness in Fournier gangrene remain insufficient.[103][104] Similarly, therapeutic plasma exchange has been suggested to remove toxins and inflammatory mediators from patients. However, there is currently insufficient evidence to recommend it.[103]
Treatment Summary
- Successful therapy for Fournier gangrene relies on early recognition and prompt surgical debridement.
- This should be accompanied by hemodynamic resuscitation and broad-spectrum antibiotics without undue delay.
- Imaging and laboratory testing should not delay the start of surgery in obvious or critical cases, as early surgical intervention is the most significant factor in determining survival.
- Extensive, aggressive, and early surgical debridement remains the primary mainstay of treatment.
- Wounds are managed with sterile dressings and vacuum-assisted wound pressure systems after the surgery.
- Testicles are usually preserved due to their unaffected blood supply and can be placed in subcutaneous pockets on the upper inner thighs or in pudendal thigh pouches.
- A suprapubic tube can be placed if the urethra is involved.
- A diverting colostomy or an equivalent fecal management system may be required if the rectum or anus is involved.
- Suprapubic tubes and colostomies should be minimized, as they do not improve mortality rates and are associated with increased patient morbidity.
- Hyperbaric oxygen therapy seems to help reduce morbidity and mortality.
- Reconstructive surgery can provide reasonably satisfactory results when fully healed.[59] (B3)
Differential Diagnosis
The differential diagnoses for Fournier gangrene include:
- Acute renal colic and urolithiasis
- Cellulitis
- Chancre
- Deep vein thrombosis
- Epididymitis
- Erysipelas
- Gangrenous balanitis
- Gangrenous vulvitis
- Gas gangrene (clostridial myonecrosis)
- Herpes simplex
- Inguinal lymphogranulomatosis
- Invasive candidiasis
- Mucormycosis
- Orchitis
- Perianal or periurethral abscess
- Pyoderma gangrenosum
- Pyomyositis
- Pyonephrosis
- Scrotal abscess
- Scrotal edema
- Stevens-Johnson syndrome
- Syphilis
- Testicular torsion
- Toxic epidermal necrolysis
- Toxic shock syndrome
- Vasculitis [43][66]
Prognosis
The prognosis of Fournier gangrene is multifactorial. Despite broad-spectrum antibiotics and aggressive surgical debridement, the overall mortality rate remains as high as 40%.[5][32][33][105] Prognostic factors that increase mortality include multiple comorbidities (such as poorly controlled diabetes), septic conditions, spread into the abdomen, admission to an intensive care unit, alcoholism, end-stage kidney or liver failure, obesity (BMI >30), HIV infection, female gender, fungal infections, and delayed diagnosis.[105][106][107] Coagulation disorders and multi-antibiotic–resistant bacterial infections are also poor prognostic factors.[108]
A study published in 1995 by Laor et al demonstrated that the Fournier Gangrene Severity Index (FGSI) is useful in predicting prognosis in patients with the disease.[109] The index considers temperature, heart rate, respiratory rate, serum potassium and sodium, creatinine, bicarbonate levels, hematocrit, and white blood cell count. A score greater than 9 was associated with a mortality rate of over 75%, while patients with a score below 9 had a 78% chance of survival. Other electrolyte abnormalities, such as elevated calcium and low magnesium levels, are also linked to a worse prognosis.[57]
A patient's age and the extent of tissue involvement are key factors in determining prognosis. Prognosis worsens with advancing age, and a greater degree of tissue involvement is similarly associated with a poorer outcome. In 2010, Yilmazlar et al developed the Uludag FGSI (UFGSI) scoring system, which incorporates both of these factors. Using this newly developed scoring system, a score greater than 9 was associated with a 94% likelihood of death, while a score below 9 correlated with an 81% probability of survival.[110]
The surgical APGAR score and the age-adjusted Charleston comorbidity index (ACCI) are the 2 general surgical scoring systems that can help determine the prognosis of patients with Fournier gangrene. The ACCI is a prognostic classification system that assigns points to 19 different comorbidities, with each comorbidity given a score of 1, 2, 3, or 6. Higher scores are linked to an increased risk of mortality. The sAPGAR score is used to assess the likelihood of complications in postoperative patients.
The sAPGAR score is based on estimated blood loss, the lowest mean arterial pressure, and the lowest heart rate. A lower sAPGAR score indicates a higher risk of complications. While not specific to Fournier gangrene, both sAPGAR and ACCI scores are generally comparable to the FGSI and UFGSI in predicting patient outcomes.[111] In studies comparing these scoring systems, the ACCI system demonstrated the highest sensitivity and specificity overall and was also among the easiest to use clinically.[111][112]
The time from disease onset to surgical treatment is critical, as patients who present earlier and receive prompt, emergent surgical debridement tend to have better outcomes.[4][34] Diabetic patients with a hemoglobin A1c (HbA1c) greater than 7 have also been found to have a worse prognosis.[109][113] A high neutrophil-to-lymphocyte ratio (>9) and a low lymphocyte-to-CRP ratio have been suggested as reliable indicators of increased mortality from Fournier gangrene.[114][115][116]
Complications
Due to the devastating effects of Fournier gangrene and its high mortality rate, complications can arise in both the short and long term.
Short-term systemic complications of Fournier gangrene result from the body’s inflammatory response to this aggressive infection. These systemic complications include acute renal failure, acute respiratory distress syndrome, cardiac arrhythmias, heart failure, multiple organ failure, and bacteremia. Bacteremia can cause acute thromboembolic events, such as strokes and arterial occlusion in the lower extremities, potentially leading to amputations. Also, patients may develop ileus due to multiple surgeries they undergo. Wound infections can also occur after debridement; however, as previously discussed, adjunctive treatments, such as hyperbaric oxygen, help reduce the rate of wound infections.[117]
Patients with significant disease involvement of the perineum may develop fecal incontinence due to involvement of the anal sphincter, necessitating debridement. These patients often require a colostomy to prevent fecal contamination of the wound. However, the formation of a colostomy carries several potential complications, including stoma evisceration and stomal infection. As the penis is frequently involved, urinary tract infections are common complications of Fournier gangrene. Urinary retention may occur due to periurethral swelling, which obstructs the ability to void. Treatment typically includes urinary catheterization, and cystostomy may be required in certain patient groups.[66]
Psychological complications are prevalent in patients who suffer from Fournier gangrene due to the profound impact the disease has on the genitals. Many patients experience long-term pain, leading to a decreased quality of life and an increased risk of depression. Disfiguring scars associated with the recovery process further contribute to psychological distress. Sexual dysfunction is also prevalent, resulting from impaired penile function, penile deviation, and penile torsion. Additionally, loss of penile skin sensitivity and pain during erections contribute to sexual dysfunction.[7][118]
Deterrence and Patient Education
Fournier gangrene is a rare but deadly infection of the genital and perineal areas. Symptoms of this infectious process include swelling of the genitals and perineal region associated with significant pain. Systemic symptoms are also common. Although no specific preventive measures exist, certain actions can minimize the risk of developing the disease. Diabetic patients should regularly examine the groin area for any signs of redness, swelling, or pain.
In addition, proper management of diabetes with optimal medication adherence is also beneficial. Diabetic patients with an HbA1c below 7 have a better prognosis if they develop Fournier gangrene. Also, maintaining proper hygiene and skin care is crucial, as skin breakdown can be an initial step in developing the disease.[113]
Pearls and Other Issues
Key facts regarding Fournier gangrene include:
- Fournier gangrene is a rapidly progressive, life-threatening infection of the genitals and perineum with a very high mortality rate, even with optimal modern medical treatment.
- Special care and attention should be provided to patients presenting with unexplained groin or scrotal pain, cellulitis, or localized infections, as misdiagnosis can prove fatal.
- Particular attention is needed for patients with diabetes, a history of hypertension, alcohol abuse, spinal cord injury (with paraplegia or quadriplegia), morbid obesity, or immunocompromised status, as these factors increase the risk of developing Fournier gangrene or may cause delays in diagnosis.
- On physical examination, the patient may experience pain disproportionate to the visible findings, as there may be minimal or no significant cutaneous manifestations. In such cases, a high degree of suspicion is essential.
- Management of these complex cases often requires the involvement of multiple medical and surgical specialties, including colorectal surgery, critical care, emergency medicine, endocrinology, general surgery, infectious disease, internal medicine, nephrology, OB-GYN, plastic surgery, wound care, and urology.
- Medical treatment focuses on resuscitation with IV fluids and antibiotics; however, priority must be given to emergent surgical exploration and aggressive debridement.
- Medical resuscitation measures, laboratory studies, and diagnostic imaging should not be permitted to delay surgical exploration in obvious or clear-cut cases.
- Rapid surgical intervention is the most critical factor in improving overall patient survival in Fournier gangrene.
- The use of suprapubic tubes and diverting colostomies should be minimized, as they do not appear to improve mortality and may increase morbidity.
- Testicular preservation is often possible since their blood supply comes from the spermatic cord. Relocating them to pudendal thigh pouches may be the most effective approach.
- Despite the severe complications, many patients ultimately report satisfaction with their quality of life.
Enhancing Healthcare Team Outcomes
The treatment and management of Fournier gangrene necessitate an interprofessional approach. Patients typically present to the emergency department or their primary care physician. Once diagnosed and admitted to the hospital, the management of Fournier gangrene is most effective when handled by a team of healthcare professionals, including an intensivist, urologist, pharmacist, infectious disease specialist, and nursing staff.
In the emergency department, timely identification of Fournier gangrene is crucial. The sooner a patient is evaluated and their workup initiated, the faster they can receive an accurate diagnosis and appropriate treatment. Once diagnosed, the patient should be admitted for urological consultation and prompt surgical debridement. These patients typically require admission to an intensive care unit, where their vital signs will be closely monitored by nursing staff, who will promptly report any concerns about patient deterioration to the intensivist.
Pharmacy and infectious disease specialists are critical in selecting the appropriate antibiotics, which should be adjusted based on culture sensitivities. If the wound remains open, a wound care nurse should be involved in managing dressing changes. A stoma nurse should evaluate the appliance and ensure that the skin surrounding the stoma is well-protected. These patients require vigilant monitoring, and any member of the interprofessional healthcare team who notices a change in status—such as relapse, therapeutic failure, or adverse drug events or interactions—must document their observations and notify the appropriate team members promptly to initiate necessary interventions. This comprehensive, interprofessional approach to treating patients with Fournier gangrene is essential for reducing the associated mortality.[39]
Fournier gangrene is a potentially fatal condition with an overall mortality rate of up to 40%.[5][14][32][33][105] Mortality is influenced by factors such as age, time to surgical intervention, and predisposing conditions such as diabetes mellitus, hypertension, and immunocompromise. With timely diagnosis and proper management, most survivors are generally satisfied with their quality of life and cosmetic outcomes, despite complications such as chronic pain, sexual dysfunction, and fecal incontinence.[119]
Media
References
Carroll PR, Cattolica EV, Turzan CW, McAninch JW. Necrotizing soft-tissue infections of the perineum and genitalia. Etiology and early reconstruction. The Western journal of medicine. 1986 Feb:144(2):174-8 [PubMed PMID: 3953086]
Short B. Fournier gangrene: an historical reappraisal. Internal medicine journal. 2018 Sep:48(9):1157-1160. doi: 10.1111/imj.14031. Epub [PubMed PMID: 30182399]
Taken K, Oncu MR, Ergun M, Eryilmaz R, Demir CY, Demir M, Gunes M. Fournier's gangrene: Causes, presentation and survival of sixty-five patients. Pakistan journal of medical sciences. 2016 May-Jun:32(3):746-50. doi: 10.12669/pjms.323.9798. Epub [PubMed PMID: 27375726]
Wong CH, Chang HC, Pasupathy S, Khin LW, Tan JL, Low CO. Necrotizing fasciitis: clinical presentation, microbiology, and determinants of mortality. The Journal of bone and joint surgery. American volume. 2003 Aug:85(8):1454-60 [PubMed PMID: 12925624]
Level 2 (mid-level) evidenceJoury A, Mahendra A, Alshehri M, Downing A. Extensive necrotizing fasciitis from Fournier's gangrene. Urology case reports. 2019 Sep:26():100943. doi: 10.1016/j.eucr.2019.100943. Epub 2019 Jun 9 [PubMed PMID: 31236328]
Level 3 (low-level) evidenceMishra SP, Singh S, Gupta SK. Necrotizing Soft Tissue Infections: Surgeon's Prospective. International journal of inflammation. 2013:2013():609628. doi: 10.1155/2013/609628. Epub 2013 Dec 24 [PubMed PMID: 24455410]
Thwaini A, Khan A, Malik A, Cherian J, Barua J, Shergill I, Mammen K. Fournier's gangrene and its emergency management. Postgraduate medical journal. 2006 Aug:82(970):516-9 [PubMed PMID: 16891442]
Voelzke BB, Hagedorn JC. Presentation and Diagnosis of Fournier Gangrene. Urology. 2018 Apr:114():8-13. doi: 10.1016/j.urology.2017.10.031. Epub 2017 Nov 13 [PubMed PMID: 29146218]
Bellapianta JM, Ljungquist K, Tobin E, Uhl R. Necrotizing fasciitis. The Journal of the American Academy of Orthopaedic Surgeons. 2009 Mar:17(3):174-82 [PubMed PMID: 19264710]
Wróblewska M, Kuzaka B, Borkowski T, Kuzaka P, Kawecki D, Radziszewski P. Fournier's gangrene--current concepts. Polish journal of microbiology. 2014:63(3):267-73 [PubMed PMID: 25546936]
Bjurlin MA, O'Grady T, Kim DY, Divakaruni N, Drago A, Blumetti J, Hollowell CM. Causative pathogens, antibiotic sensitivity, resistance patterns, and severity in a contemporary series of Fournier's gangrene. Urology. 2013 Apr:81(4):752-8. doi: 10.1016/j.urology.2012.12.041. Epub 2013 Feb 20 [PubMed PMID: 23434087]
Auerbach J, Bornstein K, Ramzy M, Cabrera J, Montrief T, Long B. Fournier Gangrene in the Emergency Department: Diagnostic Dilemmas, Treatments and Current Perspectives. Open access emergency medicine : OAEM. 2020:12():353-364. doi: 10.2147/OAEM.S238699. Epub 2020 Nov 9 [PubMed PMID: 33204184]
Level 3 (low-level) evidenceHeijkoop B, Parker N, Spernat D. Fournier's gangrene: not as lethal as previously thought? A case series. ANZ journal of surgery. 2019 Apr:89(4):350-352. doi: 10.1111/ans.14760. Epub 2018 Sep 2 [PubMed PMID: 30173412]
Level 2 (mid-level) evidenceSparenborg JD, Brems JA, Wood AM, Hwang JJ, Venkatesan K. Fournier's gangrene: a modern analysis of predictors of outcomes. Translational andrology and urology. 2019 Aug:8(4):374-378. doi: 10.21037/tau.2019.03.09. Epub [PubMed PMID: 31555561]
Kuzaka B, Wróblewska MM, Borkowski T, Kawecki D, Kuzaka P, Młynarczyk G, Radziszewski P. Fournier's Gangrene: Clinical Presentation of 13 Cases. Medical science monitor : international medical journal of experimental and clinical research. 2018 Jan 28:24():548-555 [PubMed PMID: 29374769]
Level 3 (low-level) evidenceEl-Qushayri AE, Khalaf KM, Dahy A, Mahmoud AR, Benmelouka AY, Ghozy S, Mahmoud MU, Bin-Jumah M, Alkahtani S, Abdel-Daim MM. Fournier's gangrene mortality: A 17-year systematic review and meta-analysis. International journal of infectious diseases : IJID : official publication of the International Society for Infectious Diseases. 2020 Mar:92():218-225. doi: 10.1016/j.ijid.2019.12.030. Epub 2020 Jan 18 [PubMed PMID: 31962181]
Level 1 (high-level) evidenceLiu H. Case literature analysis of Fournier's gangrene caused by sodium-glucose protein-2 inhibitors. Frontiers in medicine. 2024:11():1301105. doi: 10.3389/fmed.2024.1301105. Epub 2024 Apr 12 [PubMed PMID: 38681048]
Level 3 (low-level) evidenceCroft BJ, Ali N, Aslam W. Fournier Gangrene due to Sodium-Glucose Transport Protein-2 Inhibitor Use. American journal of therapeutics. 2024 Mar-Apr 01:31(2):e203-e205. doi: 10.1097/MJT.0000000000001611. Epub 2023 Apr 19 [PubMed PMID: 37476857]
Imai T, Kato N, Kanda N, Hashimoto H, Yamana H, Hatakeyama S. Risk of Urogenital Bacterial Infection with Sodium-Glucose Cotransporter-2 Inhibitors: A Retrospective Cohort Study Using a Claims Database. Diabetes therapy : research, treatment and education of diabetes and related disorders. 2024 Aug:15(8):1821-1830. doi: 10.1007/s13300-024-01613-7. Epub 2024 Jul 3 [PubMed PMID: 38958909]
Level 2 (mid-level) evidenceAlexakis C, Zacharis K, Chondros S, Kravvaritis S, Charitos T. A Rare Case of Necrotizing Fasciitis in a Female With Diabetes Mellitus. Cureus. 2024 Jul:16(7):e64905. doi: 10.7759/cureus.64905. Epub 2024 Jul 19 [PubMed PMID: 39156365]
Level 3 (low-level) evidenceBarnes EN, Arvelo E, Fountain MW. An Uncommon Case of Fournier's Gangrene in a Female Patient. Cureus. 2023 Dec:15(12):e50906. doi: 10.7759/cureus.50906. Epub 2023 Dec 21 [PubMed PMID: 38249253]
Level 3 (low-level) evidenceAbbasi B, Hacker E, Ghaffar U, Hakam N, Li KD, Alazzawi S, Fernandez A, Patel HV, Breyer BN. Higher Morbidity and Mortality in Females With Fournier Gangrene Compared With Males: Insights From National Inpatient Sample Data. The Journal of urology. 2025 Jan:213(1):99-109. doi: 10.1097/JU.0000000000004264. Epub 2024 Oct 2 [PubMed PMID: 39357026]
Gadler T, Huey S, Hunt K. Recognizing Fournier's Gangrene in the Emergency Department. Advanced emergency nursing journal. 2019 Jan/Mar:41(1):33-38. doi: 10.1097/TME.0000000000000221. Epub [PubMed PMID: 30702531]
Sorensen MD, Krieger JN. Fournier's Gangrene: Epidemiology and Outcomes in the General US Population. Urologia internationalis. 2016:97(3):249-259 [PubMed PMID: 27172977]
Sorensen MD, Krieger JN, Rivara FP, Broghammer JA, Klein MB, Mack CD, Wessells H. Fournier's Gangrene: population based epidemiology and outcomes. The Journal of urology. 2009 May:181(5):2120-6. doi: 10.1016/j.juro.2009.01.034. Epub 2009 Mar 14 [PubMed PMID: 19286224]
Level 2 (mid-level) evidenceElem B, Ranjan P. Impact of immunodeficiency virus (HIV) on Fournier's gangrene: observations in Zambia. Annals of the Royal College of Surgeons of England. 1995 Jul:77(4):283-6 [PubMed PMID: 7574321]
Moussa M, Abou Chakra M. Isolated Penile Fournier's gangrene: A case report and literature review. International journal of surgery case reports. 2019:62():65-68. doi: 10.1016/j.ijscr.2019.08.012. Epub 2019 Aug 17 [PubMed PMID: 31450216]
Level 3 (low-level) evidenceMouraviev VB, Pautler SE, Hayman WP. Fournier's gangrene following penile self-injection with cocaine. Scandinavian journal of urology and nephrology. 2002:36(4):317-8 [PubMed PMID: 12201928]
Level 3 (low-level) evidenceBloomgarden Z, Einhorn D, Grunberger G, Handelsman Y. Fournier's gangrene and sodium-glucose cotransporter 2 inhibitors: Is there a causal association? Journal of diabetes. 2019 May:11(5):340-341. doi: 10.1111/1753-0407.12897. Epub 2019 Feb 3 [PubMed PMID: 30600643]
Perkins TA, Bieniek JM, Sumfest JM. Solitary Candida albicans Infection Causing Fournier Gangrene and Review of Fungal Etiologies. Reviews in urology. 2014:16(2):95-8 [PubMed PMID: 25009452]
Serrano Olave A, Bueno Moral AI, Martínez Bañón C, González Mesa E, Jiménez López JS. Fournier's Gangrene under Sodium-Glucose Cotransporter-2 Inhibitors Therapy in Gynecological Patients. International journal of environmental research and public health. 2022 May 21:19(10):. doi: 10.3390/ijerph19106261. Epub 2022 May 21 [PubMed PMID: 35627798]
Level 2 (mid-level) evidenceRudd KE, Johnson SC, Agesa KM, Shackelford KA, Tsoi D, Kievlan DR, Colombara DV, Ikuta KS, Kissoon N, Finfer S, Fleischmann-Struzek C, Machado FR, Reinhart KK, Rowan K, Seymour CW, Watson RS, West TE, Marinho F, Hay SI, Lozano R, Lopez AD, Angus DC, Murray CJL, Naghavi M. Global, regional, and national sepsis incidence and mortality, 1990-2017: analysis for the Global Burden of Disease Study. Lancet (London, England). 2020 Jan 18:395(10219):200-211. doi: 10.1016/S0140-6736(19)32989-7. Epub [PubMed PMID: 31954465]
Radcliffe RS, Khan MA. Mortality associated with Fournier's gangrene remains unchanged over 25 years. BJU international. 2020 Apr:125(4):610-616. doi: 10.1111/bju.14998. Epub 2020 Feb 17 [PubMed PMID: 31975540]
Peetermans M, de Prost N, Eckmann C, Norrby-Teglund A, Skrede S, De Waele JJ. Necrotizing skin and soft-tissue infections in the intensive care unit. Clinical microbiology and infection : the official publication of the European Society of Clinical Microbiology and Infectious Diseases. 2020 Jan:26(1):8-17. doi: 10.1016/j.cmi.2019.06.031. Epub 2019 Jul 5 [PubMed PMID: 31284035]
Sugihara T, Yasunaga H, Horiguchi H, Fujimura T, Ohe K, Matsuda S, Fushimi K, Homma Y. Impact of surgical intervention timing on the case fatality rate for Fournier's gangrene: an analysis of 379 cases. BJU international. 2012 Dec:110(11 Pt C):E1096-100. doi: 10.1111/j.1464-410X.2012.11291.x. Epub 2012 Jun 21 [PubMed PMID: 22726768]
Level 2 (mid-level) evidenceSmith GL, Bunker CB, Dinneen MD. Fournier's gangrene. British journal of urology. 1998 Mar:81(3):347-55 [PubMed PMID: 9523650]
Wetterauer C, Ebbing J, Halla A, Kuehl R, Erb S, Egli A, Schaefer DJ, Seifert HH. A contemporary case series of Fournier's gangrene at a Swiss tertiary care center-can scoring systems accurately predict mortality and morbidity? World journal of emergency surgery : WJES. 2018:13():25. doi: 10.1186/s13017-018-0187-0. Epub 2018 Jun 22 [PubMed PMID: 29977327]
Level 2 (mid-level) evidenceThayer J, Mailey BA. Two-stage Neoscrotum Reconstruction Using Porcine Bladder Extracellular Matrix after Fournier's Gangrene. Plastic and reconstructive surgery. Global open. 2020 Aug:8(8):e3034. doi: 10.1097/GOX.0000000000003034. Epub 2020 Aug 25 [PubMed PMID: 32983789]
Ioannidis O, Kitsikosta L, Tatsis D, Skandalos I, Cheva A, Gkioti A, Varnalidis I, Symeonidis S, Savvala NA, Parpoudi S, Paraskevas GK, Pramateftakis MG, Kotidis E, Mantzoros I, Tsalis KG. Fournier's Gangrene: Lessons Learned from Multimodal and Multidisciplinary Management of Perineal Necrotizing Fasciitis. Frontiers in surgery. 2017:4():36. doi: 10.3389/fsurg.2017.00036. Epub 2017 Jul 10 [PubMed PMID: 28740847]
Goh T, Goh LG, Ang CH, Wong CH. Early diagnosis of necrotizing fasciitis. The British journal of surgery. 2014 Jan:101(1):e119-25. doi: 10.1002/bjs.9371. Epub 2013 Nov 29 [PubMed PMID: 24338771]
Level 1 (high-level) evidenceDemir CY, Yuzkat N, Ozsular Y, Kocak OF, Soyalp C, Demirkiran H. Fournier Gangrene: Association of Mortality with the Complete Blood Count Parameters. Plastic and reconstructive surgery. 2018 Jul:142(1):68e-75e. doi: 10.1097/PRS.0000000000004516. Epub [PubMed PMID: 29952902]
Roje Z, Roje Z, Matić D, Librenjak D, Dokuzović S, Varvodić J. Necrotizing fasciitis: literature review of contemporary strategies for diagnosing and management with three case reports: torso, abdominal wall, upper and lower limbs. World journal of emergency surgery : WJES. 2011 Dec 23:6(1):46. doi: 10.1186/1749-7922-6-46. Epub 2011 Dec 23 [PubMed PMID: 22196774]
Level 3 (low-level) evidenceChernyadyev SA, Ufimtseva MA, Vishnevskaya IF, Bochkarev YM, Ushakov AA, Beresneva TA, Galimzyanov FV, Khodakov VV. Fournier's Gangrene: Literature Review and Clinical Cases. Urologia internationalis. 2018:101(1):91-97. doi: 10.1159/000490108. Epub 2018 Jun 27 [PubMed PMID: 29949811]
Level 3 (low-level) evidenceMontrief T, Long B, Koyfman A, Auerbach J. Fournier Gangrene: A Review for Emergency Clinicians. The Journal of emergency medicine. 2019 Oct:57(4):488-500. doi: 10.1016/j.jemermed.2019.06.023. Epub 2019 Aug 28 [PubMed PMID: 31472943]
Ballard DH, Mazaheri P, Raptis CA, Lubner MG, Menias CO, Pickhardt PJ, Mellnick VM. Fournier Gangrene in Men and Women: Appearance on CT, Ultrasound, and MRI and What the Surgeon Wants to Know. Canadian Association of Radiologists journal = Journal l'Association canadienne des radiologistes. 2020 Feb:71(1):30-39. doi: 10.1177/0846537119888396. Epub 2020 Jan 28 [PubMed PMID: 32063012]
Urushidani S, Oka N. A black perineal skin lesion: a sign of Fournier gangrene. CMAJ : Canadian Medical Association journal = journal de l'Association medicale canadienne. 2023 Jul 24:195(28):E957. doi: 10.1503/cmaj.230658. Epub [PubMed PMID: 37487617]
Singh A, Ahmed K, Aydin A, Khan MS, Dasgupta P. Fournier's gangrene. A clinical review. Archivio italiano di urologia, andrologia : organo ufficiale [di] Societa italiana di ecografia urologica e nefrologica. 2016 Oct 5:88(3):157-164. doi: 10.4081/aiua.2016.3.157. Epub 2016 Oct 5 [PubMed PMID: 27711086]
Hakkarainen TW, Kopari NM, Pham TN, Evans HL. Necrotizing soft tissue infections: review and current concepts in treatment, systems of care, and outcomes. Current problems in surgery. 2014 Aug:51(8):344-62. doi: 10.1067/j.cpsurg.2014.06.001. Epub 2014 Jun 12 [PubMed PMID: 25069713]
Castleberg E, Jenson N, Dinh VA. Diagnosis of necrotizing faciitis with bedside ultrasound: the STAFF Exam. The western journal of emergency medicine. 2014 Feb:15(1):111-3. doi: 10.5811/westjem.2013.8.18303. Epub [PubMed PMID: 24578776]
Level 3 (low-level) evidenceSingam P, Wei KT, Ruffey A, Lee J, Chou TG. Fournier's Gangrene: A Case of Neglected Symptoms with Devastating Physical Loss. The Malaysian journal of medical sciences : MJMS. 2012 Jul:19(3):81-4 [PubMed PMID: 23610554]
Level 3 (low-level) evidenceSaijo S, Kuramoto Y, Yoshinari M, Tagami H. Extremely extended Fournier's gangrene. Dermatologica. 1990:181(3):228-32 [PubMed PMID: 2269383]
Level 3 (low-level) evidenceFerreira PC, Reis JC, Amarante JM, Silva ÁC, Pinho CJ, Oliveira IC, da Silva PN. Fournier's gangrene: a review of 43 reconstructive cases. Plastic and reconstructive surgery. 2007 Jan:119(1):175-184. doi: 10.1097/01.prs.0000244925.80290.57. Epub [PubMed PMID: 17255671]
Level 2 (mid-level) evidenceTalwar A, Puri N, Singh M. Fournier's Gangrene of the Penis: A Rare Entity. Journal of cutaneous and aesthetic surgery. 2010 Jan:3(1):41-4. doi: 10.4103/0974-2077.63394. Epub [PubMed PMID: 20606995]
Level 3 (low-level) evidenceFerretti M, Saji AA, Phillips J. Fournier's Gangrene: A Review and Outcome Comparison from 2009 to 2016. Advances in wound care. 2017 Sep 1:6(9):289-295. doi: 10.1089/wound.2017.0730. Epub [PubMed PMID: 28894636]
Level 3 (low-level) evidenceNigam V, Halim TA, Chhabra HS. Fournier's gangrene in a female with spinal cord injury: a case report. Spinal cord. 2010 Mar:48(3):268-9. doi: 10.1038/sc.2009.127. Epub 2009 Sep 29 [PubMed PMID: 19786974]
Level 3 (low-level) evidenceFan SL, Miller NS, Lee J, Remick DG. Diagnosing sepsis - The role of laboratory medicine. Clinica chimica acta; international journal of clinical chemistry. 2016 Sep 1:460():203-10. doi: 10.1016/j.cca.2016.07.002. Epub 2016 Jul 4 [PubMed PMID: 27387712]
Verma S, Sayana A, Kala S, Rai S. Evaluation of the Utility of the Fournier's Gangrene Severity Index in the Management of Fournier's Gangrene in North India: A Multicentre Retrospective Study. Journal of cutaneous and aesthetic surgery. 2012 Oct:5(4):273-6. doi: 10.4103/0974-2077.104916. Epub [PubMed PMID: 23378710]
Level 2 (mid-level) evidenceEke N. Fournier's gangrene: a review of 1726 cases. The British journal of surgery. 2000 Jun:87(6):718-28 [PubMed PMID: 10848848]
Level 3 (low-level) evidenceChennamsetty A, Khourdaji I, Burks F, Killinger KA. Contemporary diagnosis and management of Fournier's gangrene. Therapeutic advances in urology. 2015 Aug:7(4):203-15. doi: 10.1177/1756287215584740. Epub [PubMed PMID: 26445600]
Level 3 (low-level) evidenceVargas-Roa JC, Quintero-Vanegas S, Zuluaga-Gómez M, Gómez-Ortiz D, González-Arroyave D, Ardila CM. PoCUS for the management of Fournier's gangrene in the emergency department: A case report. Biomedical reports. 2023 Oct:19(4):67. doi: 10.3892/br.2023.1649. Epub 2023 Aug 11 [PubMed PMID: 37719679]
Level 3 (low-level) evidenceDi Serafino M, Gullotto C, Gregorini C, Nocentini C. A clinical case of Fournier's gangrene: imaging ultrasound. Journal of ultrasound. 2014 Dec:17(4):303-6. doi: 10.1007/s40477-014-0106-5. Epub 2014 Jul 1 [PubMed PMID: 25368689]
Level 3 (low-level) evidenceYen ZS, Wang HP, Ma HM, Chen SC, Chen WJ. Ultrasonographic screening of clinically-suspected necrotizing fasciitis. Academic emergency medicine : official journal of the Society for Academic Emergency Medicine. 2002 Dec:9(12):1448-51 [PubMed PMID: 12460854]
Chen F, Neill E, Graglia S. Point-of-care ultrasound for the diagnosis of Fournier gangrene. Emergency medicine journal : EMJ. 2023 Sep:40(9):682-685. doi: 10.1136/emermed-2023-213262. Epub 2023 Jul 25 [PubMed PMID: 37491154]
Levenson RB, Singh AK, Novelline RA. Fournier gangrene: role of imaging. Radiographics : a review publication of the Radiological Society of North America, Inc. 2008 Mar-Apr:28(2):519-28. doi: 10.1148/rg.282075048. Epub [PubMed PMID: 18349455]
Fernando SM, Tran A, Cheng W, Rochwerg B, Kyeremanteng K, Seely AJE, Inaba K, Perry JJ. Necrotizing Soft Tissue Infection: Diagnostic Accuracy of Physical Examination, Imaging, and LRINEC Score: A Systematic Review and Meta-Analysis. Annals of surgery. 2019 Jan:269(1):58-65. doi: 10.1097/SLA.0000000000002774. Epub [PubMed PMID: 29672405]
Level 1 (high-level) evidenceMallikarjuna MN, Vijayakumar A, Patil VS, Shivswamy BS. Fournier's Gangrene: Current Practices. ISRN surgery. 2012:2012():942437. doi: 10.5402/2012/942437. Epub 2012 Dec 3 [PubMed PMID: 23251819]
Wysoki MG, Santora TA, Shah RM, Friedman AC. Necrotizing fasciitis: CT characteristics. Radiology. 1997 Jun:203(3):859-63 [PubMed PMID: 9169717]
Level 2 (mid-level) evidenceRajan DK, Scharer KA. Radiology of Fournier's gangrene. AJR. American journal of roentgenology. 1998 Jan:170(1):163-8 [PubMed PMID: 9423625]
Piedra T, Ruíz E, González FJ, Arnaiz J, Lastra P, López-Rasines G. Fournier's gangrene: a radiologic emergency. Abdominal imaging. 2006 Jul-Aug:31(4):500-2 [PubMed PMID: 16947074]
Level 3 (low-level) evidenceElmi AM, Kusbeci M, Osoble Osman FA. A case report of Fournier's gangrene: Imaging ultrasound and computed tomography (CT) scan. Radiology case reports. 2022 Mar:17(3):959-962. doi: 10.1016/j.radcr.2021.12.057. Epub 2022 Jan 18 [PubMed PMID: 35106103]
Level 3 (low-level) evidenceNepal P, Ojili V, Kaur N, Tirumani SH, Nagar A. Gas Where It Shouldn't Be! Imaging Spectrum of Emphysematous Infections in the Abdomen and Pelvis. AJR. American journal of roentgenology. 2021 Mar:216(3):812-823. doi: 10.2214/AJR.20.23545. Epub 2021 Jan 13 [PubMed PMID: 33439049]
Ganapathy A, Ballard DH, Chen DZ, Schneider M, Lanier MH, Mazaheri P, Ilahi O, Kirby JP, Raptis CA, Mellnick VM. Preoperative computed tomography in Fournier's gangrene does not delay time to surgery. Emergency radiology. 2023 Dec:30(6):711-717. doi: 10.1007/s10140-023-02177-y. Epub 2023 Oct 19 [PubMed PMID: 37857761]
Kochkine S, Payne DL, Chung K, Chen D, Bernstein MP, Baxter AB, McMenamy JM. Imaging of necrotizing fasciitis. Clinical imaging. 2024 Dec:116():110331. doi: 10.1016/j.clinimag.2024.110331. Epub 2024 Oct 23 [PubMed PMID: 39500213]
Morgan MS. Diagnosis and management of necrotising fasciitis: a multiparametric approach. The Journal of hospital infection. 2010 Aug:75(4):249-57. doi: 10.1016/j.jhin.2010.01.028. Epub 2010 Jun 9 [PubMed PMID: 20542593]
Evans L, Rhodes A, Alhazzani W, Antonelli M, Coopersmith CM, French C, Machado FR, Mcintyre L, Ostermann M, Prescott HC, Schorr C, Simpson S, Wiersinga WJ, Alshamsi F, Angus DC, Arabi Y, Azevedo L, Beale R, Beilman G, Belley-Cote E, Burry L, Cecconi M, Centofanti J, Coz Yataco A, De Waele J, Dellinger RP, Doi K, Du B, Estenssoro E, Ferrer R, Gomersall C, Hodgson C, Hylander Møller M, Iwashyna T, Jacob S, Kleinpell R, Klompas M, Koh Y, Kumar A, Kwizera A, Lobo S, Masur H, McGloughlin S, Mehta S, Mehta Y, Mer M, Nunnally M, Oczkowski S, Osborn T, Papathanassoglou E, Perner A, Puskarich M, Roberts J, Schweickert W, Seckel M, Sevransky J, Sprung CL, Welte T, Zimmerman J, Levy M. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock 2021. Critical care medicine. 2021 Nov 1:49(11):e1063-e1143. doi: 10.1097/CCM.0000000000005337. Epub [PubMed PMID: 34605781]
Toporek AH, Semler MW, Self WH, Bernard GR, Wang L, Siew ED, Stollings JL, Wanderer JP, Rice TW, Casey JD, SMART Investigators and the Pragmatic Critical Care Research Group. Balanced Crystalloids versus Saline in Critically Ill Adults with Hyperkalemia or Acute Kidney Injury: Secondary Analysis of a Clinical Trial. American journal of respiratory and critical care medicine. 2021 May 15:203(10):1322-1325. doi: 10.1164/rccm.202011-4122LE. Epub [PubMed PMID: 33503391]
Level 3 (low-level) evidenceBenjelloun el B, Souiki T, Yakla N, Ousadden A, Mazaz K, Louchi A, Kanjaa N, Taleb KA. Fournier's gangrene: our experience with 50 patients and analysis of factors affecting mortality. World journal of emergency surgery : WJES. 2013 Apr 1:8(1):13. doi: 10.1186/1749-7922-8-13. Epub 2013 Apr 1 [PubMed PMID: 23547796]
Kabay S, Yucel M, Yaylak F, Algin MC, Hacioglu A, Kabay B, Muslumanoglu AY. The clinical features of Fournier's gangrene and the predictivity of the Fournier's Gangrene Severity Index on the outcomes. International urology and nephrology. 2008:40(4):997-1004. doi: 10.1007/s11255-008-9401-4. Epub 2008 Jun 19 [PubMed PMID: 18563618]
Level 2 (mid-level) evidenceVanguardia MKR, Lew C, Prabhakaran S, Kong JCH. Fournier's gangrene: 15-year retrospective study at a tertiary hospital. BJS open. 2024 Mar 1:8(2):. doi: 10.1093/bjsopen/zrae022. Epub [PubMed PMID: 38626185]
Level 2 (mid-level) evidenceKincius M, Telksnys T, Trumbeckas D, Jievaltas M, Milonas D. Evaluation of LRINEC Scale Feasibility for Predicting Outcomes of Fournier Gangrene. Surgical infections. 2016 Aug:17(4):448-53. doi: 10.1089/sur.2015.076. Epub 2016 Mar 29 [PubMed PMID: 27023717]
Level 2 (mid-level) evidenceEl-Sabbagh AH. Coverage of the scrotum after Fournier's gangrene. GMS Interdisciplinary plastic and reconstructive surgery DGPW. 2018:7():Doc01. doi: 10.3205/iprs000121. Epub 2018 Jan 15 [PubMed PMID: 29423355]
Campos JA, Martos JA, Gutiérrez del Pozo R, Carretero P. Synchronous caverno-spongious thrombosis and Fournier's gangrene. Archivos espanoles de urologia. 1990 May:43(4):423-6 [PubMed PMID: 2383054]
Level 3 (low-level) evidenceChawla SN, Gallop C, Mydlo JH. Fournier's gangrene: an analysis of repeated surgical debridement. European urology. 2003 May:43(5):572-5 [PubMed PMID: 12706005]
Level 2 (mid-level) evidenceHong KS, Yi HJ, Lee RA, Kim KH, Chung SS. Prognostic factors and treatment outcomes for patients with Fournier's gangrene: a retrospective study. International wound journal. 2017 Dec:14(6):1352-1358. doi: 10.1111/iwj.12812. Epub 2017 Sep 25 [PubMed PMID: 28944569]
Level 2 (mid-level) evidenceOzkan OF, Koksal N, Altinli E, Celik A, Uzun MA, Cıkman O, Akbas A, Ergun E, Kiraz HA, Karaayvaz M. Fournier's gangrene current approaches. International wound journal. 2016 Oct:13(5):713-6. doi: 10.1111/iwj.12357. Epub 2014 Aug 22 [PubMed PMID: 25145578]
Level 2 (mid-level) evidenceChen JH, Li YB, Li DG, Zeng XM, Yao QY, Fu J, Wang GH, Huang XY. Vacuum sealing drainage to treat Fournier's gangrene. BMC surgery. 2023 Jul 26:23(1):211. doi: 10.1186/s12893-023-02109-0. Epub 2023 Jul 26 [PubMed PMID: 37496026]
Tanwar S, Paruthy SB, Singh A, Pandurangappa V, Kumar D, Pal S. Evaluation of Negative Pressure Wound Therapy in the Management of Fournier's Gangrene. Cureus. 2023 Nov:15(11):e48300. doi: 10.7759/cureus.48300. Epub 2023 Nov 5 [PubMed PMID: 38058329]
Weinfeld AB, Kelley P, Yuksel E, Tiwari P, Hsu P, Choo J, Hollier LH. Circumferential negative-pressure dressing (VAC) to bolster skin grafts in the reconstruction of the penile shaft and scrotum. Annals of plastic surgery. 2005 Feb:54(2):178-83 [PubMed PMID: 15655470]
Level 3 (low-level) evidenceOguz A, Gümüş M, Turkoglu A, Bozdağ Z, Ülger BV, Agaçayak E, Böyük A. Fournier's Gangrene: A Summary of 10 Years of Clinical Experience. International surgery. 2015 May:100(5):934-41. doi: 10.9738/INTSURG-D-15-00036.1. Epub 2015 Apr 10 [PubMed PMID: 25859652]
Lordan JT, Rawal J, Simson JN. Safe and simple trephine loop colostomy. Annals of the Royal College of Surgeons of England. 2007 Sep:89(6):634-5 [PubMed PMID: 18213741]
Eray IC, Alabaz O, Akcam AT, Ulku A, Parsak CK, Sakman G, Seydaoglu G. Comparison of Diverting Colostomy and Bowel Management Catheter Applications in Fournier Gangrene Cases Requiring Fecal Diversion. The Indian journal of surgery. 2015 Dec:77(Suppl 2):438-41. doi: 10.1007/s12262-013-0868-6. Epub 2013 Jan 27 [PubMed PMID: 26730041]
Level 3 (low-level) evidenceSarofim M, Di Re A, Descallar J, Toh JWT. Relationship between diversional stoma and mortality rate in Fournier's gangrene: a systematic review and meta-analysis. Langenbeck's archives of surgery. 2021 Dec:406(8):2581-2590. doi: 10.1007/s00423-021-02175-z. Epub 2021 Apr 16 [PubMed PMID: 33864128]
Level 1 (high-level) evidenceRosen DR, Brown ME, Cologne KG, Ault GT, Strumwasser AM. Long-term follow-up of Fournier's Gangrene in a tertiary care center. The Journal of surgical research. 2016 Nov:206(1):175-181. doi: 10.1016/j.jss.2016.06.091. Epub 2016 Jul 15 [PubMed PMID: 27916359]
Rosa I, Guerreiro F. Hyperbaric Oxygen Therapy for the Treatment of Fournier's Gangrene: A Review of 34 Cases. Acta medica portuguesa. 2015 Sep-Oct:28(5):619-23 [PubMed PMID: 26667866]
Level 3 (low-level) evidenceFeres O, Feitosa MR, Ribeiro da Rocha JJ, Miranda JM, Dos Santos LE, Féres AC, de Camargo HP, Parra RS. Hyperbaric oxygen therapy decreases mortality due to Fournier's gangrene: a retrospective comparative study. Medical gas research. 2021 Jan-Mar:11(1):18-23. doi: 10.4103/2045-9912.310055. Epub [PubMed PMID: 33642333]
Level 2 (mid-level) evidenceCreta M, Longo N, Arcaniolo D, Giannella R, Cai T, Cicalese A, De Nunzio C, Grimaldi G, Cicalese V, De Sio M, Autorino R, Lima E, Fedelini P, Marmo M, Capece M, La Rocca R, Tubaro A, Imbimbo C, Mirone V, Fusco F. Hyperbaric oxygen therapy reduces mortality in patients with Fournier's Gangrene. Results from a multi-institutional observational study. Minerva urologica e nefrologica = The Italian journal of urology and nephrology. 2020 Apr:72(2):223-228. doi: 10.23736/S0393-2249.20.03696-6. Epub 2020 Feb 19 [PubMed PMID: 32083420]
Level 2 (mid-level) evidenceHedetoft M, Bennett MH, Hyldegaard O. Adjunctive hyperbaric oxygen treatment for necrotising soft-tissue infections: A systematic review and meta-analysis. Diving and hyperbaric medicine. 2021 Mar 31:51(1):34-43. doi: 10.28920/dhm51.1.34-43. Epub [PubMed PMID: 33761539]
Level 1 (high-level) evidenceMindrup SR, Kealey GP, Fallon B. Hyperbaric oxygen for the treatment of fournier's gangrene. The Journal of urology. 2005 Jun:173(6):1975-7 [PubMed PMID: 15879795]
Level 2 (mid-level) evidenceRaizandha MA, Hidayatullah F, Kloping YP, Rahman IA, Djatisoesanto W, Rizaldi F. The role of hyperbaric oxygen therapy in Fournier's Gangrene: A systematic review and meta-analysis of observational studies. International braz j urol : official journal of the Brazilian Society of Urology. 2022 Sep-Oct:48(5):771-781. doi: 10.1590/S1677-5538.IBJU.2022.0119. Epub [PubMed PMID: 35594328]
Level 1 (high-level) evidenceLewis GD, Majeed M, Olang CA, Patel A, Gorantla VR, Davis N, Gluschitz S. Fournier's Gangrene Diagnosis and Treatment: A Systematic Review. Cureus. 2021 Oct:13(10):e18948. doi: 10.7759/cureus.18948. Epub 2021 Oct 21 [PubMed PMID: 34815897]
Level 1 (high-level) evidenceSchneidewind L, Anheuser P, Schönburg S, Wagenlehner FME, Kranz J. Hyperbaric Oxygenation in the Treatment of Fournier's Gangrene: A Systematic Review. Urologia internationalis. 2021:105(3-4):247-256. doi: 10.1159/000511615. Epub 2020 Dec 7 [PubMed PMID: 33285541]
Level 1 (high-level) evidenceCapelli-Schellpfeffer M, Gerber GS. The use of hyperbaric oxygen in urology. The Journal of urology. 1999 Sep:162(3 Pt 1):647-54 [PubMed PMID: 10458334]
Saifee NH, Evans HL, Magaret AS, Hess JR, Delaney M, O'Keefe GE, Pham TN, Foy H, Bulger E, Pagano MB. Outcomes in necrotizing soft tissue infections treated with therapeutic plasma exchange. Transfusion. 2017 Jun:57(6):1407-1413. doi: 10.1111/trf.14067. Epub 2017 Mar 7 [PubMed PMID: 28266045]
Norrby-Teglund A, Muller MP, Mcgeer A, Gan BS, Guru V, Bohnen J, Thulin P, Low DE. Successful management of severe group A streptococcal soft tissue infections using an aggressive medical regimen including intravenous polyspecific immunoglobulin together with a conservative surgical approach. Scandinavian journal of infectious diseases. 2005:37(3):166-72 [PubMed PMID: 15849047]
Al-Kohlany K, Baker K, Ahmed F, Mohamed M, Alshami M, Badheeb M. Treatment outcome of Fournier's gangrene and its associated factors: A retrospective study. Archivio italiano di urologia, andrologia : organo ufficiale [di] Societa italiana di ecografia urologica e nefrologica. 2023 May 29:95(2):11318. doi: 10.4081/aiua.2023.11318. Epub 2023 May 29 [PubMed PMID: 37254929]
Dupont M, Leal C, Tenreiro N, Marques R, Pinto-de-Sousa J. Fournier Gangrene Management: Is a Stoma Mandatory? Cureus. 2023 May:15(5):e39450. doi: 10.7759/cureus.39450. Epub 2023 May 24 [PubMed PMID: 37378202]
Shet P, Mustafa AD, Varshney K, Rao L, Sawdagar S, McLennan F, Ansari S, Shet D, Sivathamboo N, Campbell S. Risk Factors for Mortality Among Patients With Fournier Gangrene: A Systematic Review. Surgical infections. 2024 May:25(4):261-271. doi: 10.1089/sur.2023.372. Epub 2024 Apr 16 [PubMed PMID: 38625013]
Level 1 (high-level) evidenceHong HB, Lee JW, Park CH. Prognostic factors and clinical outcomes in Fournier's Gangrene: a retrospective study of 35 patients. BMC infectious diseases. 2024 Sep 11:24(1):958. doi: 10.1186/s12879-024-09900-1. Epub 2024 Sep 11 [PubMed PMID: 39261759]
Level 2 (mid-level) evidenceLaor E, Palmer LS, Tolia BM, Reid RE, Winter HI. Outcome prediction in patients with Fournier's gangrene. The Journal of urology. 1995 Jul:154(1):89-92 [PubMed PMID: 7776464]
Yilmazlar T, Ozturk E, Ozguc H, Ercan I, Vuruskan H, Oktay B. Fournier's gangrene: an analysis of 80 patients and a novel scoring system. Techniques in coloproctology. 2010 Sep:14(3):217-23. doi: 10.1007/s10151-010-0592-1. Epub 2010 Jun 18 [PubMed PMID: 20559857]
Level 2 (mid-level) evidenceRoghmann F, von Bodman C, Löppenberg B, Hinkel A, Palisaar J, Noldus J. Is there a need for the Fournier's gangrene severity index? Comparison of scoring systems for outcome prediction in patients with Fournier's gangrene. BJU international. 2012 Nov:110(9):1359-65. doi: 10.1111/j.1464-410X.2012.11082.x. Epub 2012 Apr 11 [PubMed PMID: 22494217]
Level 2 (mid-level) evidenceZhu XD, Ding F, Wang GD, Shao Q. [Different scoring systems to evaluate the prognosis of Fournier's gangrene: A comparative study]. Zhonghua nan ke xue = National journal of andrology. 2015 Aug:21(8):720-3 [PubMed PMID: 26442300]
Level 2 (mid-level) evidenceSen H, Bayrak O, Erturhan S, Borazan E, Koc MN. Is hemoglobin A1c level effective in predicting the prognosis of Fournier gangrene? Urology annals. 2016 Jul-Sep:8(3):343-7. doi: 10.4103/0974-7796.184905. Epub [PubMed PMID: 27453658]
Wirjopranoto S. Comparison between neutrophil-to-lymphocyte ratio and platelet-to-lymphocyte ratio as predictors of mortality on Fournier's gangrene cases. Indian journal of urology : IJU : journal of the Urological Society of India. 2023 Apr-Jun:39(2):121-125. doi: 10.4103/iju.iju_256_22. Epub 2023 Mar 31 [PubMed PMID: 37304980]
Level 3 (low-level) evidenceYim SU, Kim SW, Ahn JH, Cho YH, Chung H, Hwang EC, Yu HS, Oh KJ, Kim SO, Jung SI, Kang TW, Kwon DD, Park K. Neutrophil to Lymphocyte and Platelet to Lymphocyte Ratios Are More Effective than the Fournier's Gangrene Severity Index for Predicting Poor Prognosis in Fournier's Gangrene. Surgical infections. 2016 Apr:17(2):217-23. doi: 10.1089/sur.2015.126. Epub 2016 Feb 2 [PubMed PMID: 26835748]
Yildirim M, Gul SC, Angın YS, Saglam AI, Ozsoy U, Koca B, Ozkan N. Lymphocyte-to-C-reactive protein ratio as a new biomarker for predicting mortality and morbidity in Fournier's gangrene. Cirugia y cirujanos. 2024:92(2):181-188. doi: 10.24875/CIRU.22000529. Epub [PubMed PMID: 38782374]
Wolach MD, MacDermott JP, Stone AR, deVere White RW. Treatment and complications of Fournier's gangrene. British journal of urology. 1989 Sep:64(3):310-4 [PubMed PMID: 2804566]
Level 3 (low-level) evidenceCzymek R, Kujath P, Bruch HP, Pfeiffer D, Nebrig M, Seehofer D, Guckelberger O. Treatment, outcome and quality of life after Fournier's gangrene: a multicentre study. Colorectal disease : the official journal of the Association of Coloproctology of Great Britain and Ireland. 2013 Dec:15(12):1529-36. doi: 10.1111/codi.12396. Epub [PubMed PMID: 24034257]
Level 2 (mid-level) evidenceTheiss M, Hofmockel G, Eckert P, Frohmüller H. [Cosmetic and functional long-term outcome after operation of Fournier gangrene]. Der Urologe. Ausg. A. 1996 Jul:35(4):338-41 [PubMed PMID: 8928365]