Introduction
Glycogen storage diseases (GSDs) are inherited inborn errors of carbohydrate metabolism that result in abnormal glycogen storage. The onset can range from neonatal life to adulthood, and clinical manifestations result either from a failure to convert glycogen into energy or the toxic accumulation of glycogen.[1]
Glycogen is a branched polymer comprised of glucose monomers (see Image. Glycogen, Free Glucose Release, and Glycogen Storage Diseases, Figure 1). After a meal, the plasma glucose level rises, stimulating the storage of the excess in cytoplasmic glycogen.
The liver contains the highest percentage of glycogen by weight (about 10%), whereas muscles can store about 2% by weight. Nevertheless, since the total muscle mass is greater than the liver mass, the total mass of glycogen in muscles is about twice that of the liver. When needed, the glycogen polymer can be broken down into glucose monomers and utilized for energy production. Defects in the enzymes and transporters for these processes cause GSDs. An increasing number of GSDs are being identified, but most are very rare. These subtypes are classified numerically in the order of recognition and identification of the enzyme defect causing the disorder.[2][3]
Classification of Glycogen Storage Disorder
GSDs that primarily affect the liver include the following:
- Glycogen synthase-2 deficiency (GSD type 0a)
- Glucose-6-phosphatase deficiency (GSD type Ia)
- Glucose-6-phosphate transporter deficiency (GSD type Ib)
- Glycogen debrancher deficiency (GSD type III)
- Glycogen branching enzyme deficiency (GSD type IV)
- Liver phosphorylase deficiency (GSD type VI)
- Phosphorylase kinase deficiency (GSD type IXa)
- GLUT2 deficiency or Fanconi-Bickel disease
GSDs that primarily affect the skeletal muscles include the following:
- Muscle phosphorylase deficiency (GSD type V)
- Phosphofructokinase deficiency (GSD type VII)
- Phosphoglycerate mutase deficiency (GSD type X)
- Lactate dehydrogenase A deficiency (GSD type XI)
- Aldolase A deficiency (GSD type XII)
- β-enolase deficiency (GSD type XIII)
- Phosphoglucomutase-1 deficiency (GSD type XIV)
GSDs that affect both skeletal and cardiac muscles include the following:
- Lysosomal acid maltase deficiency (GSD type IIa)
- Lysosome-associated membrane protein 2 deficiency (GSD type IIb)
- Glycogenin-1 deficiency (GSD type XV)
- Muscle glycogen synthase deficiency (GSD type 0b)
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
The etiology of GSDs is best understood by following the metabolic events leading to glycogen synthesis (glycogenesis) and degradation (glycogenolysis). Excess dietary glucose is stored in glycogen, and the synthesis of this molecule is, in part, accomplished by glycogen synthase. As indicated in Table 1, glycogen synthase has 2 distinct forms: one in the liver encoded by the GYS2 gene and another in skeletal muscle encoded by the GYS1 gene (see Image. Glycogen, Free Glucose Release, and Glycogen Storage Diseases, Table 1). Both enzyme forms work by attaching glucose monomers to growing glycogen polymers by creating α-1,4 links. As indicated in Figure 1 (see Image. Glycogen, Free Glucose Release, and Glycogen Storage Diseases, Figure 1), glycogen has α-1,4 and α-1,6 bonds between glucose units.
About 95% of glycogen linkages consist of α-1,4 bonds. Mutations in the GYS2 gene result in the absence or dysfunction of liver glycogen synthase, impairing glycogen synthesis in the liver and causing GSD type 0a. Similarly, mutations in the GYS1 gene lead to the absence or malfunction of muscle glycogen synthase, disrupting glycogen synthesis in muscles and resulting in GSD type 0b.
Glycogen synthase catalyzes the formation of α-1,4 glucose linkages in glycogen, but the glycogen branching enzyme (GBE1) is required to create the branching α-1,6 linkages. Mutations in GBE1 lead to the production of abnormally structured glycogen, known as polyglucosan bodies, which is the hallmark of GSD type IV. These polyglucosan bodies accumulate in liver and muscle cells and do not effectively undergo glycogenolysis. In muscle tissue, this accumulation causes weakness and myopathy, while in the liver, it results in hepatomegaly.
While GSD 0a and GSD 0b result from insufficient glycogen storage, most GSDs arise from defects in glycogenolysis, leading to glycogen accumulation. The initial step of glycogenolysis involves glycogen phosphorylase, which releases glucose-1-phosphate from glycogen. Mutations in the muscle-specific glycogen phosphorylase gene (PYGM) cause GSD type V, while mutations in the liver-specific glycogen phosphorylase gene (PYGL) result in GSD type VI.[4] The glucose-1-phosphate produced is subsequently converted to glucose-6-phosphate by phosphoglucomutase. In the liver, glucose-6-phosphatase, encoded by the G6PC gene, converts glucose-6-phosphate into free glucose, which is released into the bloodstream as an energy source for other tissues and organs (see Image. Glycogen, Free Glucose Release, and Glycogen Storage Diseases, Figure 2).
Notably, skeletal muscles lack glucose-6-phosphatase and cannot release glucose into the bloodstream. GSD type I arises from genetic defects in glucose-6-phosphatase metabolism. GSD type Ia, also known as von Gierke disease, is caused by mutations in the G6PC gene. In hepatocytes, glucose-6-phosphate is synthesized in the cytoplasm and transported into the lumen of the endoplasmic reticulum, where glucose-6-phosphatase converts it into glucose. The glucose is then transported back to the cytoplasm and subsequently released into the bloodstream via the hepatic GLUT2 transporter.[5]
Glucose-6-phosphate translocase 1 (G6PT1) is the transporter protein that facilitates the movement of glucose-6-phosphate between the cytoplasm and the endoplasmic reticulum. The G6PT protein consists of 3 subunits: G6PT1, G6PT2, and G6PT3 (see Image. Glycogen, Free Glucose Release, and Glycogen Storage Diseases, Figure 2). Mutations in the SLC37A4 gene, which encodes the G6PT1 protein, cause GSD type Ib (see Image. Glycogen, Free Glucose Release, and Glycogen Storage Diseases, Table 1). Fanconi-Bickel disease, a rare glycogen storage disorder, results from GLUT2 deficiency due to mutations in the SLC2A2 gene. GLUT2 deficiency impairs glucose export, increases intracellular glucose levels, and reduces glycogen degradation, leading to excessive glycogen storage and hepatomegaly.
Glycogen is a branched polymer, with glycogen phosphorylase removing glucose from α-1,4 linkages but unable to act on α-1,6 linkages at branch points. A glycogen debranching enzyme (GDE) is required to remove these branch points. In mammals, this enzyme is called "amylo-α-1,6-glucosidase, 4-α-glucanotransferase," encoded by the AGL gene. Mutations in the AGL gene cause GSD type III, resulting in either a nonfunctional GDE (GSD type IIIa or IIIb) or a GDE with reduced function (GSD type IIIc or IIId).[6]
GSD type II is unique among glycogen storage diseases, as it is also classified as a lysosomal storage disease.[7] Lysosomes are subcellular organelles responsible for recycling cellular macromolecules. Lysosomal storage diseases arise from the absence or dysfunction of a lysosomal enzyme. In GSD type II, the deficient enzyme is lysosomal acid α-glucosidase, encoded by the GAA gene. This enzyme breaks down glycogen into glucose for cellular energy. Mutations in the GAA gene lead to toxic glycogen accumulation within lysosomes.
Epidemiology
The true incidence of metabolic diseases is difficult to determine, given the lack of uniform, universal screening at birth. While GSD type IX has been found to be the most common subtype, the individual incidence of specific GSD types is further complicated due to overlapping symptoms and the lack of standardized specific testing in most areas of the world.
A study evaluating the incidence of inborn errors of metabolism in British Columbia in the 1990s reported that the incidence of these diseases was approximately 30 cases per 100,000 live births.[8] This figure represented a mix of metabolic disorders and was not restricted to GSDs. Approximately 2.3 children per 100,000 births were thought to have GSD in this study. Current literature suggests the incidence of GSDs is approximately 1 case per 20,000 to 43,000 live births, although incidence rates are found to be higher in specific population groups, such as non-Ashkenazi Jews.[9]
Pathophysiology
As mentioned, glycogen is the storage form of glucose and consists of long polymers of α-1,4-linked glucose, with branch points formed by α-1,6-linked glucose molecules. Glycogen's primary physiologic function is to provide glucose via glycogenolysis for glucose homeostasis. Liver stores are used to maintain glucose homeostasis in the serum, and muscle stores provide glucose for the muscles during periods of high demand, especially exercise, as a source of energy.
Hypoglycemia, hepatomegaly, muscle cramps, exercise intolerance, and weakness develop when these physiological functions are defective. Some disorders also affect the myocardial tissue and can lead to cardiomyopathy and cardiac conduction defects.[10] Failure to maintain glucose homeostasis triggers alternate pathways to meet metabolic demands. In GSD type 1, for example, failure of glycogenolysis in the liver results in increased lactic acid production, resulting in lactic acidosis due to the intracellular accumulation of glucose-6-phosphate, which stimulates the glycolytic pathway.
History and Physical
GSDs are a diverse set of rare inborn errors of carbohydrate metabolism that can have variable phenotypic presentations even within the same GSD type. Obtaining a family pedigree is useful in establishing the mode of inheritance. Most GSDs show an autosomal recessive inheritance, but a few, like GSD type IX, show an X-linked inheritance. Common presenting symptoms include growth retardation and poor weight gain in children, exercise intolerance, hypoglycemia, hepatomegaly, low muscle tone, acidosis, and hyperlipidemia. The most common manifestations of these disorders are hypoglycemia and exercise intolerance.
Patients with defects in hepatic glycogen metabolism typically present with fasting hypoglycemia and ketosis, with symptoms improving after glucose administration. The duration of fasting required to trigger hypoglycemia is a critical aspect of the history in patients with GSD. Hypoglycemia occurring after a short fasting period suggests glycogen storage disorders type I or III. In contrast, symptoms arising after an overnight fast indicate glycogen storage disorders type 0, VI, or IX.
All patients with GSDs should have anthropometric measurements obtained and graphed to assess their overall growth pattern. Short stature or poor linear growth and motor latency, especially in a child with hypoglycemia, warrant a GSD workup.
The inability to properly release glucose from glycogen can result in the abnormal accumulation of glycogen. In the liver, this failure results in hepatomegaly with the potential development of cirrhosis.
Defects in skeletal muscle glycogen metabolism lead to fatigue, muscle cramps, and exercise intolerance after brief periods of moderate-to-intense exercise, in contrast to defects in fatty acid metabolism, where symptoms typically appear after prolonged exercise. Individuals with skeletal muscle-associated GSDs may also present with rhabdomyolysis or myoglobinuria. In rare instances, these disorders may present as weakness instead of muscle cramps, which can progress to fixed weakness over time.[11] Patients with defects affecting cardiac muscles usually develop symptoms of cardiomyopathy, left ventricular hypertrophy, and, rarely, conduction defects.[12]
Evaluation
Laboratory Testing
Hypoglycemia should be documented by measuring serum glucose levels. In patients where hypoglycemia is suspected, a diagnostic fasting glucose test can be performed but should only be considered in a monitored inpatient setting.[13] Hepatic GSDs (type 0, III, VI, and IX) are characterized by ketosis and usually yield a β-hydroxybutyrate level greater than 2.5 mmol/L. These diseases also typically present with hypertriglyceridemia and elevated liver function tests. Patients with skeletal muscle-associated GSDs may also have elevated creatine kinase levels and urinary myoglobin levels. GSD type I is associated with elevated levels of lactic acid and acidosis.[14]
Biopsy
Although specific genetic testing is now available for diagnosing most GSDs, histologic examination of liver or muscle biopsy is still used in specific scenarios. In GSD type 0, a liver biopsy typically shows decreased hepatic glycogen and can make a definitive diagnosis for this disease.[15] In GSD type I, a liver biopsy should reveal pale-staining, swollen hepatocytes, steatosis, and nuclear hyper-glycogenation. Fibrosis is another common finding on liver biopsy in patients with GSDs and is predominant in patients with GSD type III, IV, and VI. In GSD type III, periportal fibrosis and micronodular cirrhosis are often seen with distended hepatocytes due to excess glycogen accumulation.[16]
Muscle biopsies typically reveal diastase-sensitive vacuoles that yield a positive staining result with periodic acid-Schiff (PAS) and acid phosphatase in GSD type IV.[17] In GSD type V, a muscle biopsy should demonstrate negative histochemical staining for phosphorylase activity. In the absence of phosphorylase activity, the specimen remains brown instead of taking up a deep blue hue. In addition, the biopsy should reveal subsarcolemmal deposits of glycogen detected by PAS staining.[18] In patients with GSD type XV, muscle biopsies often show PAS-positive inclusions that are not digested with α-amylase treatment and, on electron microscopy, may be seen as filamentous material corresponding to polyglucosan bodies.[19]
Molecular Testing
Molecular genetic testing is noninvasive and, for the most part, available for diagnosing these rare genetic disorders. In some cases, genetic tests have eliminated the need for invasive muscle and liver biopsies. The table below outlines the genetic foci of mutations for these disorders.
Table 2. Enzyme Deficiencies and Genes Involved in Various Glycogen Storage Diseases
| Condition | Gene Involved |
| Glycogen synthase-2 deficiency (GSD type 0a) | GYS2 |
| Glucose-6-phosphatase deficiency (GSD type Ia) | G6Pase gene mutations or G6PC1 catalytic activity |
| Glucose-6-phosphate transporter deficiency (GSD type Ib) | SLC37A4 |
| Glycogen debrancher deficiency (GSD type III) | AGL |
| Glycogen branching enzyme deficiency (GSD type IV) | GBE1 |
| Liver phosphorylase deficiency (GSD type VI) | PYGL |
| Phosphorylase kinase deficiency (GSD type IXa) | PHKA2 |
| GLUT2 deficiency or Fanconi-Bickel disease | SLC2A2 |
| Muscle phosphorylase deficiency (GSD type V) | PYGM |
| Phosphofructokinase deficiency (GSD type VII) | PFKM |
| Phosphoglycerate mutase deficiency (GSD type X) | PGAM |
| Lactate dehydrogenase A deficiency (GSD type XI) | LDHA |
| Aldolase A deficiency (GSD type XII) | ALDOA |
| β-enolase deficiency (GSD type XIII) | ENO3 |
| Phosphoglucomutase-1 deficiency (GSD type XIV) | PGM1 |
| Lysosomal acid maltase deficiency (GSD type IIa) | GAA α-glucosidase enzyme (GAA) activity or GAA gene mutation |
| Lysosome-associated membrane protein 2 deficiency (GSD type IIb) | LAMP2 |
| Glycogenin-1 deficiency (GSD type XV) | GYG1 |
| Muscle glycogen synthase deficiency (GSD type 0b) | GYS2 [20] |
Treatment / Management
GSDs currently have no cure, and most treatments aim to alleviate signs and symptoms. Critical goals include preventing and managing hypoglycemia, hyperlactatemia, hyperuricemia, and hyperlipidemia. Hypoglycemia may be avoided through starch consumption, with a commercially available, physically modified form now in use. In patients with GLUT2 deficiency, maintaining an antiketogenic diet leads to a significant decrease in liver size and glycogen content.[21] Hyperuricemia is managed with allopurinol, while hyperlipidemia is treated with statins. Some GSDs, such as GSD type II, can now be treated with enzyme replacement therapy (ERT) using recombinant alglucosidase alfa, which helps degrade lysosomal glycogen.[22] Ongoing research explores the potential use of ERT for other forms of GSD.
Liver transplantation should be considered for patients with certain GSDs that have progressed to hepatic malignancy or failure. While this procedure can correct hepatic failure and hypoglycemia, it does not address the cardiomyopathy associated with the GSD, which may continue to progress.
The immediate management of acute hypoglycemia involves rapid correction with oral carbohydrates or parenteral glucose. Glucagon is effective only in insulin-mediated hypoglycemia and will not help patients with hypoglycemia caused by a GSD.[23]
The following table provides a brief overview of therapeutic management for each GSD:
Table 3. Management Strategies for Glycogen Storage Diseases
| GSD type 0, III, IV, VI, IXA, | Uncooked or modified cornstarch to prevent hypoglycemia and liver failure in severe cases |
| GSD type Ia, Ib | Uncooked or modified cornstarch for hypoglycemia, allopurinol for hyperuricemia, and liver transplantation in severe cases |
| GLUT2 deficiency or Fanconi-Bickel disease | Frequent small meals to prevent hypoglycemia, uncooked or modified cornstarch, and restriction of galactose |
| Muscle phosphorylase deficiency (GSD type V) | Glucose loading prior to exercise |
| Lysosomal acid maltase deficiency (GSD type IIa) | Enzyme replacement therapy, modified cornstarch to prevent hypoglycemia, and liver transplantation if needed |
| GSD type IIb, VII, X, XI, XII, XIII, XIV, XV | No specific treatment |
Differential Diagnosis
The differential diagnosis of GSDs includes the following conditions:
- Charcot-Marie-Tooth disease
- Congenital disorders of glycosylation
- Congenital lactic acidosis
- Deficiencies of phosphofructokinase
- Disorders of uric acid metabolism
- DNA depletion syndrome
- Duchenne muscular dystrophy
- Duchenne-Becker muscular dystrophy
- Endocardial fibroelastosis
- Fatty acid oxidation disorders
- Fructose-1-phosphate aldolase deficiency
- Fructose-1,6-biphosphatase deficiency
- Galactosemia
- Hyperlipoproteinemia
- Limb-girdle muscular dystrophy
- Limb-girdle muscular dystrophy
- Lysosome-associated membrane protein 2 deficiency
- Mitochondrial DNA depletion syndromes
- Mitochondrial myopathies
- Neurovisceral sphingolipidosis
- Niemann-Pick disease
- Organic acidurias
- Organic acidurias
- Polymyositis
- Sphingomyelinase deficiency
- Spinal muscular atrophy
- Werdnig-Hoffman disease
- Zellweger syndrome
A comprehensive differential diagnosis is key to differentiating GSDs from other conditions with similar presentations. Prompt and accurate diagnosis can guide appropriate therapeutic approaches and prevent unnecessary treatments.
Prognosis
The prognosis of GSDs varies widely and depends on the enzyme defect and the type of GSD. Severe infantile forms are often associated with early mortality, while milder adult-onset cases have normal life spans. With early diagnosis and proper management, the prognosis of most GSDs remains favorable. The advent of ERT is expected to further improve outcomes in these patients.
Complications
Even with appropriate dietary modifications, GSDs are associated with a wide range of serious complications. In early childhood, individuals with GSDs are at risk of hypoglycemia-associated seizures and cardiac arrest. In patients with GSD type Ia, growth delay with short stature, osteopenia, renal dysfunction, hypertriglyceridemia, and hepatocellular carcinoma can occur. In GSD type Ib, recurrent bacterial infections secondary to neutropenia may be seen. In GSD type IV, progressive liver failure with cirrhosis can occur. Cardiomyopathy and limb-girdle dystrophy can be seen in patients with GSD type II. Hypertrophic cardiomyopathy is a classic complication of GSD type III.
Growth retardation and short status are also seen in GSD types IX (a, b, c, d) and XII, but a cognitive-developmental delay is also a feature of the latter. In GSD types V and XIII, exercise intolerance and rhabdomyolysis with an associated renal injury can occur. Rarely, end-stage renal disease requiring kidney transplantation may develop in patients with GSD type Ib.[24]
Deterrence and Patient Education
Patient and parent education about dietary modifications and feeding frequency is of utmost importance in optimizing the clinical outcomes for individuals affected by these diseases. Patients and parents need specific education to monitor for signs of hypoglycemia and the increased glucose and carbohydrate requirements during an acute illness, such as an infection. Patients with skeletal muscle-associated GSDs must be cautioned against overexertion while exercising and advised to increase carbohydrate intake before they start the exercise for enhanced capacity.[25]
Additional education regarding oral replacement of electrolytes lost via the kidneys is essential in patients with GLUT2 deficiency. These individuals will also need dietary instructions to avoid galactose and follow a diet consisting of frequent small meals with adequate caloric intake to ensure optimal growth.
Emphasis on the importance of routine follow-up and frequent lab monitoring is crucial for these patients. Genetic counseling and education regarding the inheritance pattern of GSDs are also essential.
Enhancing Healthcare Team Outcomes
GSDs are a group of complex metabolic disorders best managed by an interprofessional team of clinicians, nurses, pharmacists, and dietitians. GSD currently lacks a definitive cure, and most treatments aim to address its manifestations. However, even this symptomatic management requires vigorous patient and parent education to ensure dietary restrictions and carbohydrate administration frequency are appropriately managed.
Registered dieticians and specialty nurses play a key role in educating patients and their caregivers to ensure hypoglycemia is avoided. This measure not only ameliorates the risk of hypoglycemia-associated complications but also prevents long-term disease sequelae in most GSDs. Specialty pharmacists play a pivotal role in managing GSD type II to ensure enzyme replacement therapy is carried out adequately and that the medication is administered under optimal circumstances. Primary care clinicians, which include physicians, midlevel practitioners, and pediatricians, in coordination with specialists, help ensure patients have adequate growth and function with minimal risk of severe complications, such as renal or liver failure.
All interprofessional team members should be vigilant in monitoring these patients and alert the other team members if any complications develop or the patient's condition worsens. Such efforts require meticulous documentation and open communication between everyone on the care team. The key overall goal is to avoid and treat hypoglycemia, hyperlactatemia, hyperuricemia, and hyperlipidemia. A well-coordinated interprofessional team can help manage patients with these diseases adequately and ensure they live a normal life. The development of experimental therapies, such as gene therapy, may eventually provide curative options for patients with these diseases in the future.[26]
Media
(Click Image to Enlarge)
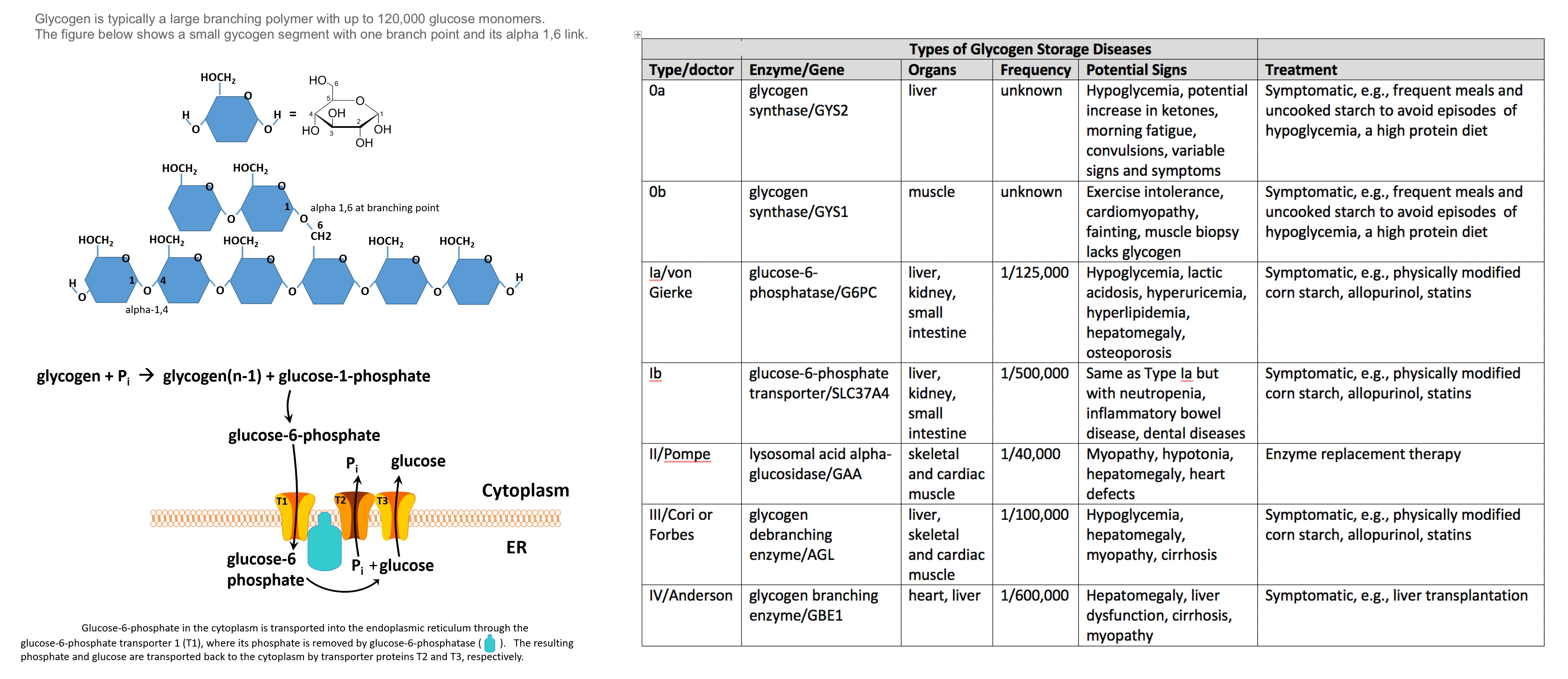
Glycogen, Free Glucose Release, and Glycogen Storage Diseases. The blue figure shows the α-1,4 and α-1,6 links in the glycogen molecule. The second figure shows how glucose-6-phosphate enters the endoplasmic reticulum and transforms into free glucose, which exits the organelle to go back to the cytoplasm. The table outlines the molecular bases and clinical manifestations of the different glycogen storage diseases.
Contributed by W Stone, MD
References
Hicks J, Wartchow E, Mierau G. Glycogen storage diseases: a brief review and update on clinical features, genetic abnormalities, pathologic features, and treatment. Ultrastructural pathology. 2011 Oct:35(5):183-96. doi: 10.3109/01913123.2011.601404. Epub [PubMed PMID: 21910565]
Level 3 (low-level) evidenceOzen H. Glycogen storage diseases: new perspectives. World journal of gastroenterology. 2007 May 14:13(18):2541-53 [PubMed PMID: 17552001]
Level 3 (low-level) evidenceKanungo S, Wells K, Tribett T, El-Gharbawy A. Glycogen metabolism and glycogen storage disorders. Annals of translational medicine. 2018 Dec:6(24):474. doi: 10.21037/atm.2018.10.59. Epub [PubMed PMID: 30740405]
Kannourakis G. Glycogen storage disease. Seminars in hematology. 2002 Apr:39(2):103-6 [PubMed PMID: 11957192]
Parikh NS, Ahlawat R. Glycogen Storage Disease Type I. StatPearls. 2025 Jan:(): [PubMed PMID: 30480935]
Adam MP, Feldman J, Mirzaa GM, Pagon RA, Wallace SE, Amemiya A, Schreuder AB, Rossi A, Grünert SC, Derks TGJ. Glycogen Storage Disease Type III. GeneReviews(®). 1993:(): [PubMed PMID: 20301788]
Chan J, Desai AK, Kazi ZB, Corey K, Austin S, Hobson-Webb LD, Case LE, Jones HN, Kishnani PS. The emerging phenotype of late-onset Pompe disease: A systematic literature review. Molecular genetics and metabolism. 2017 Mar:120(3):163-172. doi: 10.1016/j.ymgme.2016.12.004. Epub 2016 Dec 11 [PubMed PMID: 28185884]
Level 3 (low-level) evidenceApplegarth DA, Toone JR, Lowry RB. Incidence of inborn errors of metabolism in British Columbia, 1969-1996. Pediatrics. 2000 Jan:105(1):e10 [PubMed PMID: 10617747]
OCKERMAN PA. GLYCOGEN STORAGE DISEASE IN SWEDEN. Acta paediatrica Scandinavica. 1965:87():SUPPL 160:1-31 [PubMed PMID: 14331931]
Tarnopolsky MA. Metabolic Myopathies. Continuum (Minneapolis, Minn.). 2016 Dec:22(6, Muscle and Neuromuscular Junction Disorders):1829-1851 [PubMed PMID: 27922496]
Oldfors A, DiMauro S. New insights in the field of muscle glycogenoses. Current opinion in neurology. 2013 Oct:26(5):544-53. doi: 10.1097/WCO.0b013e328364dbdc. Epub [PubMed PMID: 23995275]
Level 3 (low-level) evidenceHijazi G, Paschall A, Young SP, Smith B, Case LE, Boggs T, Amarasekara S, Austin SL, Pendyal S, El-Gharbawy A, Deak KL, Muir AJ, Kishnani PS. A retrospective longitudinal study and comprehensive review of adult patients with glycogen storage disease type III. Molecular genetics and metabolism reports. 2021 Dec:29():100821. doi: 10.1016/j.ymgmr.2021.100821. Epub 2021 Nov 11 [PubMed PMID: 34820282]
Level 2 (mid-level) evidenceMorris AA, Thekekara A, Wilks Z, Clayton PT, Leonard JV, Aynsley-Green A. Evaluation of fasts for investigating hypoglycaemia or suspected metabolic disease. Archives of disease in childhood. 1996 Aug:75(2):115-9 [PubMed PMID: 8869190]
Weinstein DA, Steuerwald U, De Souza CFM, Derks TGJ. Inborn Errors of Metabolism with Hypoglycemia: Glycogen Storage Diseases and Inherited Disorders of Gluconeogenesis. Pediatric clinics of North America. 2018 Apr:65(2):247-265. doi: 10.1016/j.pcl.2017.11.005. Epub [PubMed PMID: 29502912]
Orho M, Bosshard NU, Buist NR, Gitzelmann R, Aynsley-Green A, Blümel P, Gannon MC, Nuttall FQ, Groop LC. Mutations in the liver glycogen synthase gene in children with hypoglycemia due to glycogen storage disease type 0. The Journal of clinical investigation. 1998 Aug 1:102(3):507-15 [PubMed PMID: 9691087]
Level 3 (low-level) evidenceColeman RA, Winter HS, Wolf B, Chen YT. Glycogen debranching enzyme deficiency: long-term study of serum enzyme activities and clinical features. Journal of inherited metabolic disease. 1992:15(6):869-81 [PubMed PMID: 1293383]
Level 3 (low-level) evidenceKohler L, Puertollano R, Raben N. Pompe Disease: From Basic Science to Therapy. Neurotherapeutics : the journal of the American Society for Experimental NeuroTherapeutics. 2018 Oct:15(4):928-942. doi: 10.1007/s13311-018-0655-y. Epub [PubMed PMID: 30117059]
Bartram C, Edwards RH, Beynon RJ. McArdle's disease-muscle glycogen phosphorylase deficiency. Biochimica et biophysica acta. 1995 Aug 15:1272(1):1-13 [PubMed PMID: 7662715]
Level 3 (low-level) evidenceLefeuvre C, Schaeffer S, Carlier RY, Fournier M, Chapon F, Biancalana V, Nicolas G, Malfatti E, Laforêt P. Glycogenin-1 deficiency mimicking limb-girdle muscular dystrophy. Molecular genetics and metabolism reports. 2020 Sep:24():100597. doi: 10.1016/j.ymgmr.2020.100597. Epub 2020 May 24 [PubMed PMID: 32477874]
Molares-Vila A, Corbalán-Rivas A, Carnero-Gregorio M, González-Cespón JL, Rodríguez-Cerdeira C. Biomarkers in Glycogen Storage Diseases: An Update. International journal of molecular sciences. 2021 Apr 22:22(9):. doi: 10.3390/ijms22094381. Epub 2021 Apr 22 [PubMed PMID: 33922238]
Saltik-Temizel IN, Coşkun T, Yüce A, Koçak N. Fanconi-Bickel syndrome in three Turkish patients with different homozygous mutations. The Turkish journal of pediatrics. 2005 Apr-Jun:47(2):167-9 [PubMed PMID: 16052858]
Ferreira CR, Gahl WA. Lysosomal storage diseases. Translational science of rare diseases. 2017 May 25:2(1-2):1-71. doi: 10.3233/TRD-160005. Epub 2017 May 25 [PubMed PMID: 29152458]
WHITEHOUSE FW, BRYAN HG. Glucagon for treatment of insulin hypoglycemia: its use in the patient with diabetes. American practitioner and digest of treatment. 1959 Aug:10():1326-30 [PubMed PMID: 13844432]
Martin AP, Bartels M, Schreiber S, Buehrdel P, Hauss J, Fangmann J. Successful staged kidney and liver transplantation for glycogen storage disease type Ib: A case report. Transplantation proceedings. 2006 Dec:38(10):3615-9 [PubMed PMID: 17175348]
Level 3 (low-level) evidenceValenzuela PL, Santalla A, Alejo LB, Merlo A, Bustos A, Castellote-Bellés L, Ferrer-Costa R, Maffiuletti NA, Barranco-Gil D, Pinós T, Lucia A. Dose-response effect of pre-exercise carbohydrates under muscle glycogen unavailability: Insights from McArdle disease. Journal of sport and health science. 2024 May:13(3):398-408. doi: 10.1016/j.jshs.2023.11.006. Epub 2023 Nov 27 [PubMed PMID: 38030066]
Koeberl DD, Kishnani PS, Chen YT. Glycogen storage disease types I and II: treatment updates. Journal of inherited metabolic disease. 2007 Apr:30(2):159-64 [PubMed PMID: 17308886]
Level 3 (low-level) evidence