Introduction
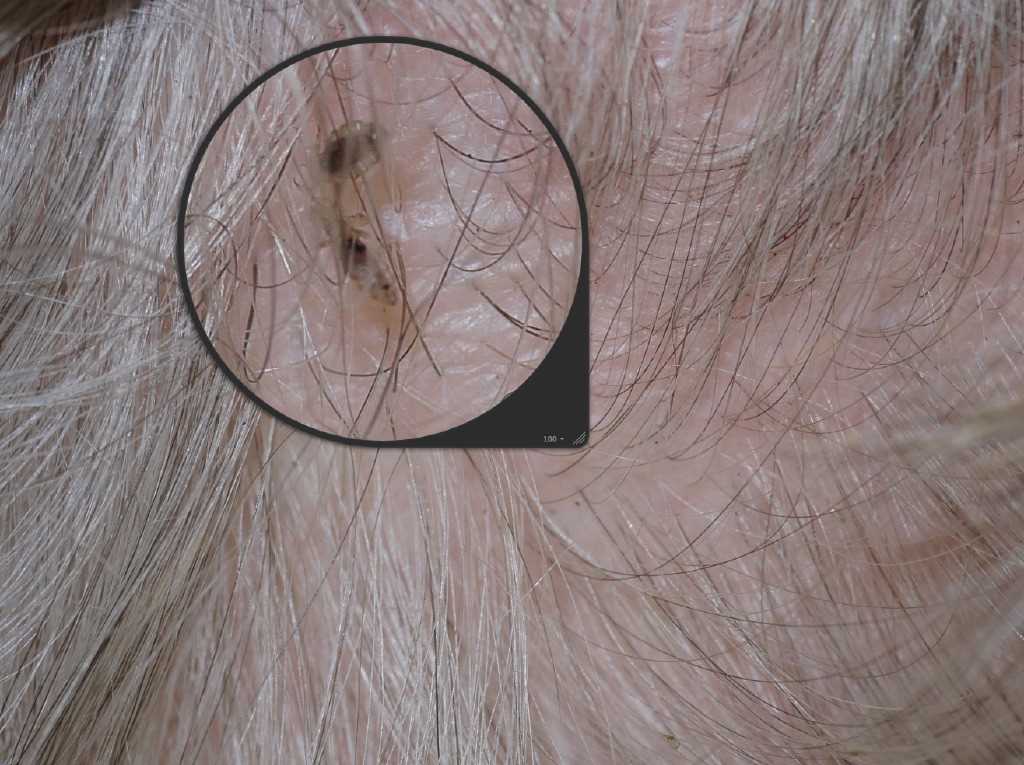
Pediculosis (louse infestation) affects hundreds of millions worldwide yearly and has been reported in all countries and socioeconomic classes. Lice are obligate, parasitic insects that have no free-living stage in their life cycle. They are transmitted by direct skin-to-skin or fomite-to-skin contact, and symptoms do not typically present for 3 to 4 weeks.[1] The 3 varieties that are parasitic to humans are Pediculus humanus capitis (head louse), Pthirus pubis (pubic or crab louse), and Pediculus humanus (body louse). Head lice are the most common lice that cross all socioeconomic barriers. In contrast, body lice more commonly affect homeless and displaced populations and should be suspected when there are signs of scratching, poor hygiene, and in the year's colder months.[2][3] See Image. Head Lice.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
Body and head lice are 1 mm to 3 mm long, while the pubic louse is much smaller.[4] The head louse is an obligate parasite that spends its entire life on the human host. Head lice feed exclusively on blood. Lice are unable to jump or fly, and transmission requires close contact. Transmission of head lice is thought to occur by head-to-head contact, sharing of headgear, or other direct contact with fomites (inanimate objects that harbor the organism, such as movie seats).[1][4] Pubic lice are transmitted through sexual contact with bedding or clothing.[4] Body lice live, lay their eggs in clothing or bedding, and only move to the skin to feed. They spread primarily by direct contact in populations with poor hygiene. However, they can also be transmitted through clothing, bedding, and towels.[3]
Epidemiology
There are limited studies on pediculosis, and further epidemiological research is needed. This is especially true in regions with significant poverty and low health standards.[5] Louse infestations affect hundreds of millions of people worldwide each year. They have been reported in all countries and all levels of society. Pediculus humanus capitis is estimated to affect 6 to 12 million people in the United States every year, but the exact numbers are unknown as it is not a reportable disease. Head lice outbreaks more commonly affect children 3 to 12 years old, with girls being affected more than boys.[6] In industrialized countries, small epidemics typically develop in schoolchildren whose tight social bonds allow for the rapid spread of the infestation. It is also common for several members of the same household to be affected. Infestations of head lice are more common in the warmer months, as well as in areas with higher humidity. Head lice cross all socioeconomic barriers, whereas body lice more commonly affect the homeless and displaced. Body lice are more common in the colder months of the year.[3][7] Pubic lice infestations are more common in sexually active people.[4]
Pathophysiology
Patients frequently present with pruritis, typically from an immune-mediated hypersensitivity reaction. It may take 2 to 6 weeks to develop symptoms after the first exposure, while pruritis can develop 1 or 2 days after re-exposure. The itching induces scratching, which can lead to secondary bacterial infection. This can ultimately lead to complications such as impetigo and pyoderma.[8] Body lice can transmit trench fever, relapsing fever, and epidemic typhus to humans.[3]
Histopathology
Histological analysis of the skin or hair is rarely required. However, sometimes, a skin biopsy reveals sharp wedges with an infiltrate of lymphocytes, excoriation marks, and intradermal hemorrhage.
History and Physical
The primary presenting complaint of pediculosis is pruritus. On physical examination, the diagnosis is confirmed by visualization of at least 1 louse on visual inspection. A bright light, magnifying lens, or fine-toothed comb (lice comb) can aid in diagnosis. Misdiagnosis is common. Finding only nits on examination cannot confirm a current infestation, as nits can stay on hair for months after successful treatment. Additionally, dandruff, hair spray debris, and dirt particles can be confused with nits as false positives. When lice are found in 1 member of a family member, all other family members in contact should also be examined for evidence of infestation. Pubic lice are diagnosed by finding lice in the pubic hair and should prompt screening for other sexually transmitted infections. The presence of body lice should be considered in patients with pruritis who live in crowded conditions and/or have evidence of poor hygiene.
Evaluation
The diagnosis is made clinically in most cases. Sticky tape can be used over the infected area to pick up the adult lice and examine them under a microscope. The nits are oval-shaped and firmly attached to the hair shaft. A Wood lamp examination may reveal greenish-yellow fluorescence of the nits. Sometimes, the pubic hair may reveal the presence of lice, which indicates a workup of a sexually transmitted infection.[9][10] Scrapings are often done to rule out a fungal infection when the diagnosis is unclear.
Treatment / Management
Historically, head lice have been removed by hand, shaving affected areas, or by physical removal with a lice comb. Wet combing involves moistening and combing the hair root-to-tip with a lice comb. Cure rates vary widely with this method.[11] Pharmacologic treatment of lice focuses on 2 mechanisms: neurotoxicity resulting in paralysis of the louse and suffocation from topical application. It is important to recognize that available treatments kill lice but not reliably destroy eggs. Repeat treatment is often required for complete eradication. A second treatment 7 to 10 days after the initial treatment is typically sufficient to eradicate most nonresistant lice.
Multiple topical pediculicides are considered first-line treatments for lice infestation. These include pyrethroids, malathion, lindane, benzyl alcohol, topical and oral ivermectin, and spinosad.[12] Pyrethroids are 1 of the most frequently used treatments for lice among topical agents. Permethrin 1%, a synthetic pyrethroid, is widely used as a treatment and is available over-the-counter in the United States. Permethrin affects sodium transport across neuronal membranes, causing respiratory paralysis in arthropods.[13] Recent evidence suggests that resistance to permethrin has been increasing. It is retained on the hair after application and has a residual effect for up to 3 weeks, although a retreatment at 1 week is recommended. Although there is evidence of resistance, its generous safety profile with low toxicity makes it a favorable first-line agent.[11] Malathion 0.5% is an organophosphate cholinesterase inhibitor that causes respiratory paralysis in arthropods. It has a good margin of safety but has an unappealing odor and requires an 8 to 12-hour treatment period. Lindane 1% is an organochloride that kills lice by respiratory paralysis. It is absorbed into the blood, slowly metabolized, and should not be used repeatedly. This agent has the potential for neurotoxicity and has been taken off the market in California. It may be used as a second-line agent in adults but should be avoided in children, the elderly, or adults weighing less than 50 kg. Benzyl alcohol 5% lotion was approved in 2009 as a topical suffocation treatment that prevents lice from closing their respiratory spiracles. It appears to have an efficacy comparable to pyrethrins. Spinosad 0.9% is a topical pediculicidal agent that was approved in 2011. It works by provoking hyperexcitation, causing death by paralysis. It was found to have twice the eradication rate of permethrin at 14 days and is effective after a single dose. It may be beneficial for patients who are not adherent to other therapies.
Topical ivermectin 0.5% lotion increases chloride in muscle cells, causing hyperpolarization and paralysis. It works with a single application. There is only a small amount of systemic absorption after topical application. However, it should be used as a third-line agent due to its limited clinical experience and cost.[14] The only currently used oral treatment for pediculosis is ivermectin. Ivermectin also has a risk of neurotoxicity. It has demonstrated effectiveness in clinical trials but is not FDA-approved for treating pediculosis. It may be an appropriate second-line therapy when the lice resist topical treatments.[15] Body lice are eradicated through proper hygiene, laundering, or insecticide application to affected clothing. Pubic lice are commonly susceptible to agents used to treat head lice, although they vary in sensitivity. Permethrin and lindane can be used, but due to their risk of neurotoxicity, lindane should only be used in resistant cases. Malathion has been used but is not approved by the FDA. Because lice can be present on inanimate fomites, heating infested clothing and bedding with hot water is necessary to destroy all stages of lice. The heat is necessary to destroy lice and nits at 52° Celcius for 30 minutes. Lice have been found to become heat resistant through hormonal mechanisms, sometimes tolerating temperatures over 100° Celcius.(B3)
Differential Diagnosis
Differential diagnosis for pediculosis includes:
- Dandruff
- Seborrhea
- Superficial fungal infection
- Eczema
- Folliculitis
- Scabies
Prognosis
The prognosis of louse infestations is generally good. When used appropriately, the medications are very effective in eradicating nymphs and mature lice. Treatment failure can be the result of several causes, including lack of ovicidal activity, failure to remove live nits, non-compliance-especially with retreatment in 7-10 days, inadequate application of the pediculicide (ie, duration, amount), failure to treat close contacts, insufficient environmental eradication, and drug resistance to the pediculicide. Some patients with body lice may contract a louse-borne infection such as trench fever, typhus, or relapsing/recurrent fever, but these are rare.
Complications
The complications that can manifest with pediculosis include the following:
- Social embarrassment
- Loss of school days
- Loss of skin integrity leading to secondary bacterial infection (impetigo and pyoderma)
- Transmission of trench fever, relapsing fever, and epidemic typhus to humans (body lice only) [3]
Deterrence and Patient Education
Treatment failure is frequently the result of noncompliance. Patients should be educated about the appropriate methods to apply the medications, including the amount to be used and the duration of treatment. They should also be informed of the importance of re-treatment in 7-10 days. Patients and caregivers should also be counseled that their infested bedding, clothing, and towels should be washed in hot water and dried on the high heat setting. Parents and children should be instructed not to share headgear such as hats and hair bows. Steps to help prevent body lice re-infestation after eradication include proper body hygiene, clothing changes weekly at a minimum, and proper clothing laundering. Sexual partners of patients with pubic lice should be treated as well.
Pearls and Other Issues
Head lice infestation can lead to mental strain and distress in patients as popular media portray affected individuals as unclean. Lice have existed for thousands of years, and pediculosis remains a prevalent disease. Treatment failure is common and usually due to inappropriate treatment, lack of compliance, failure to remove live nits, sharing personal care products, failure to treat close contacts, resistance to the drug, and failure to clean up the environment.
Enhancing Healthcare Team Outcomes
Pediculosis is a major public health problem affecting millions and is best managed with an interprofessional team approach. The problem is encountered in many schools, and unfortunately, many children often present late, and the cycle of infestation continues in the home. While lice are managed by clinicians in the emergency department and in primary care, the nurse and pharmacist play a critical role in lice management and prevention outside the hospital as part of the interprofessional healthcare team. The key is the education of patients and parents who need to know that all individuals in the family need to be examined and treated. Even family members who have no lice but share personal care products or even share a bed need prophylactic treatment. There is solid evidence that education can lower lice infestation in schools. Education is far more important than having "no nit" school policies. The pharmacist should emphasize the importance of treatment compliance and provide the parents with detailed information about how and when to use the medication. Nurses should monitor and follow up on subsequent visits, verify compliance, answer questions, and report any concerns to the prescriber. To minimize head lice infestations, the child and parent must be told not to share combs, brushes, hats, or scarves. While shaving the hair is an effective treatment, it is not acceptable today. Further, if pubic lice are found, then both partners need treatment, and they should be investigated for other sexually transmitted infections. Finally, parents should be educated on washing clothing, linens, and other garments. A cohesive interprofessional team approach best enacts all these steps.[9][16] Lice treatment is very effective, with high cure rates, especially when mature lice are identified. However, the current treatment does not kill eggs; repeat treatment is often required. Frequent lice treatment is also known to cause severe itching, which can lead to skin breakdown and secondary bacterial infections. A major problem with lice today is social embarrassment.[15][17]
Media
(Click Image to Enlarge)
References
Peterson AR, Nash E, Anderson BJ. Infectious Disease in Contact Sports. Sports health. 2019 Jan/Feb:11(1):47-58. doi: 10.1177/1941738118789954. Epub 2018 Aug 14 [PubMed PMID: 30106670]
Portillo A, Ruiz-Arrondo I, Oteo JA. Arthropods as vectors of transmisible diseases in Spain. Medicina clinica. 2018 Dec 14:151(11):450-459. doi: 10.1016/j.medcli.2018.06.021. Epub 2018 Aug 28 [PubMed PMID: 30170738]
Powers J, Badri T, Syed HA. Pediculosis Corporis. StatPearls. 2025 Jan:(): [PubMed PMID: 29489282]
Shakya M,Jayraw AK,Singh M, Pubic lice infestation in man from Mhow, Madhya Pradesh. Journal of parasitic diseases : official organ of the Indian Society for Parasitology. 2018 Sep [PubMed PMID: 30166787]
Sweileh WM. Global output of research on epidermal parasitic skin diseases from 1967 to 2017. Infectious diseases of poverty. 2018 Aug 6:7(1):74. doi: 10.1186/s40249-018-0456-x. Epub 2018 Aug 6 [PubMed PMID: 30078380]
Çetinkaya Ü, Şahin S, Ulutabanca RÖ. The Epidemiology of Scabies and Pediculosis in Kayseri. Turkiye parazitolojii dergisi. 2018 Jun:42(2):134-137. doi: 10.5152/tpd.2018.5602. Epub [PubMed PMID: 29780005]
Dagrosa AT, Elston DM. What's eating you? head lice (Pediculus humanus capitis). Cutis. 2017 Dec:100(6):389-392 [PubMed PMID: 29360900]
Veraldi S,Rossi LC,Pontini P, Head lice in African children. Giornale italiano di dermatologia e venereologia : organo ufficiale, Societa italiana di dermatologia e sifilografia. 2018 Aug [PubMed PMID: 29767485]
Yingklang M, Sengthong C, Haonon O, Dangtakot R, Pinlaor P, Sota C, Pinlaor S. Effect of a health education program on reduction of pediculosis in school girls at Amphoe Muang, Khon Kaen Province, Thailand. PloS one. 2018:13(6):e0198599. doi: 10.1371/journal.pone.0198599. Epub 2018 Jun 11 [PubMed PMID: 29889851]
Fölster-Holst R. Itch Management in Childhood. Current problems in dermatology. 2016:50():173-91. doi: 10.1159/000446090. Epub 2016 Aug 23 [PubMed PMID: 27578087]
Packer H, Heiberger AL. Getting Ahead of Head Lice: Treatment in the Setting of Resistance. South Dakota medicine : the journal of the South Dakota State Medical Association. 2016 Oct:69(10):468-470 [PubMed PMID: 28806014]
Salavastru CM, Chosidow O, Janier M, Tiplica GS. European guideline for the management of pediculosis pubis. Journal of the European Academy of Dermatology and Venereology : JEADV. 2017 Sep:31(9):1425-1428. doi: 10.1111/jdv.14420. Epub 2017 Jul 16 [PubMed PMID: 28714128]
Nanda J, Patel P, Juergens AL. Permethrin. StatPearls. 2025 Jan:(): [PubMed PMID: 31985943]
Deeks LS, Naunton M, Currie MJ, Bowden FJ. Topical ivermectin 0.5% lotion for treatment of head lice. The Annals of pharmacotherapy. 2013 Sep:47(9):1161-7. doi: 10.1177/1060028013500645. Epub [PubMed PMID: 24259731]
Level 3 (low-level) evidenceSanchezruiz WL, Nuzum DS, Kouzi SA. Oral ivermectin for the treatment of head lice infestation. American journal of health-system pharmacy : AJHP : official journal of the American Society of Health-System Pharmacists. 2018 Jul 1:75(13):937-943. doi: 10.2146/ajhp170464. Epub 2018 May 22 [PubMed PMID: 29789316]
Moshki M, Zamani-Alavijeh F, Mojadam M. Correction: Efficacy of Peer Education for Adopting Preventive Behaviors against Head Lice Infestation in Female Elementary School Students: A Randomised Controlled Trial. PloS one. 2017:12(9):e0185299. doi: 10.1371/journal.pone.0185299. Epub 2017 Sep 19 [PubMed PMID: 28926612]
Level 1 (high-level) evidenceBurgess IF, Silverston P. Head lice. BMJ clinical evidence. 2015 Jan 14:2015():. pii: 1703. Epub 2015 Jan 14 [PubMed PMID: 25587918]
Level 3 (low-level) evidence