Introduction
Overview of Stress Reactions and Fractures
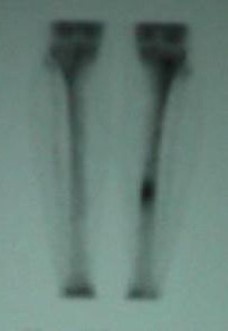
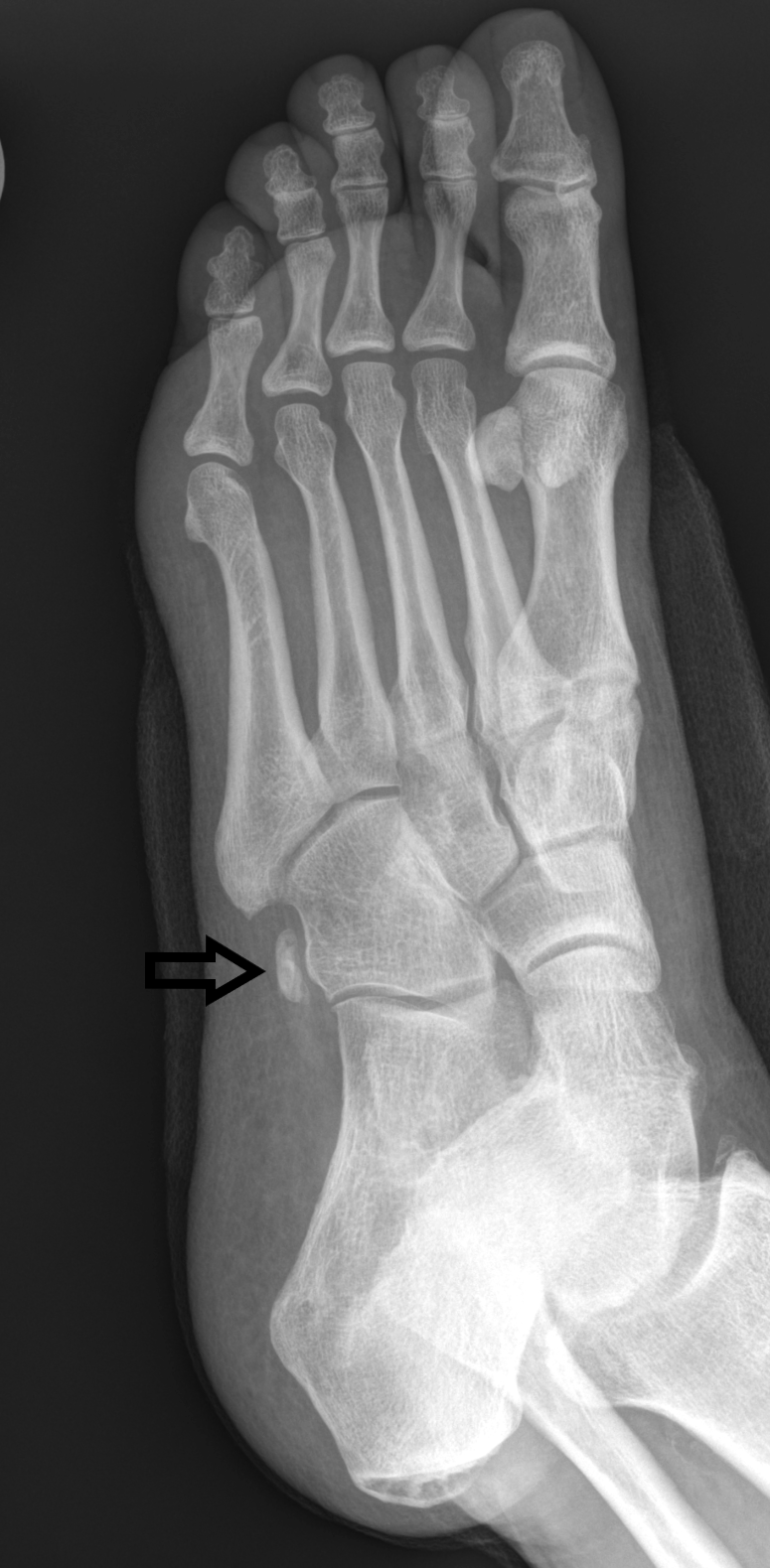
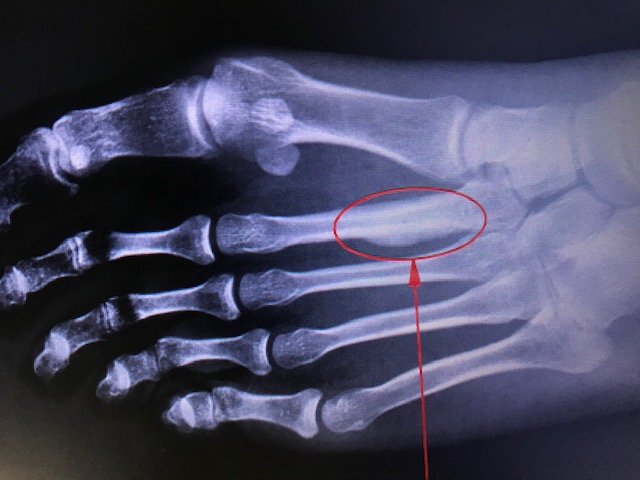
Stress injuries range from periostitis—an inflammatory reaction of the periosteum—to a complete stress fracture involving a full cortical break (see Image. Stress Reaction). These injuries result from repetitive submaximal loading of bone over time and were first documented in the mid-19th century among military recruits, described as “March Fractures” (see Image. March Fracture of Second Metatarsal).[1][2] Julius Wolff’s theory (1836–1902) holds that bones remodel in response to mechanical loads. When repetitive loading surpasses the bone’s adaptive capacity, osteoclast activity outpaces osteoblasts, leading to progressive microdamage and, ultimately, a stress fracture.[3][1]
Patients typically notice symptom onset 2 to 3 weeks after an increase in training volume or intensity, with pain that initially occurs after activity and later persists at rest.[4] Stress injuries occur most commonly in the lower extremities (eg, tibia, femur, metatarsals) and are seen frequently in running and jumping sports. Upper extremity stress injuries (eg, ulnar fractures) are less common but occur in specific populations. Diagnosis requires a high index of suspicion, a detailed history, physical examination, and imaging. Plain radiographs may remain normal for 2 to 4 weeks; thus, advanced imaging such as magnetic resonance imaging (MRI) is often necessary. Most stress fractures respond to conservative management, but high-risk fractures (eg, tension-sided femoral neck or anterior tibial cortex) may require surgical intervention. Early recognition and preventive strategies (eg, gradual increases in training) remain critical to avoiding complications.[4]
Lower Extremity Stress Fractures
The following conditions are various types of injuries affecting lower extremity bones:
Tibia
The tibia is the most frequently affected site of stress reactions and fractures.
- Medial tibial stress syndrome (MTSS): Also known as shin splints, MTSS can be difficult to distinguish from medial tibial stress fractures. MTSS pain worsens with exertion, whereas stress fracture pain often persists even during daily activities.
- Anterior cortex tibial stress fractures: These are less common and affect jumping or leaping athletes. They may present radiographically as a “dreaded black line” and carry a high risk of nonunion. Aggressive conservative measures or surgical fixation with intramedullary rods or flexible plates may be necessary.
- Medial tibial plateau stress fractures: These are rare, often mistaken for meniscal injuries or pes anserine bursitis, and require a high index of suspicion.
Femur
- Femoral neck stress fractures: These constitute approximately 11% of stress injuries in athletes and predominantly affect runners. Two subtypes exist:
- Tension-type (distraction) fractures: Involve the superior-lateral femoral neck and present the highest risk for complete fracture. Early detection is paramount.
- Compression-type fractures: Involve the inferior-medial femoral neck and occur more often in younger athletes. If no fracture line is visible, nonsurgical management may suffice.
- Femoral shaft stress fractures: These account for 22.5% of stress fractures in military recruits. Patients report vague, insidious leg pain. The “fulcrum test” may help localize pain. Nondisplaced lesions often respond well to conservative care.
Fibula
Fibular stress fractures usually occur in the distal third of the fibula, proximal to the tibiofibular ligament. Pain is reproducible on palpation.
Patella
Rare patellar stress fractures can be transverse or vertical. Transverse fractures carry a greater risk of displacement, often requiring immobilization or surgical fixation.
Medial Malleolus
Vertical stress fractures at the junction of the medial malleolus and tibial plafond appear in running and jumping athletes. Full cortical disruption usually necessitates surgical intervention.
Pelvis
Pelvic stress fractures can present vaguely, often mimicking adductor strains, osteitis pubis, or sacroiliitis. Common sites include the ischiopubic ramus and sacrum, especially in runners.
Foot and Ankle
- Calcaneus: Patients show tenderness posterior to the talus and a positive squeeze test.
- Navicular: Common in runners and basketball players, these fractures carry a high risk of nonunion due to poor blood supply. Tenderness over the navicular is a key clinical clue.
- Metatarsals: Represent about 9% of stress fractures in athletes, usually occurring in the second or third metatarsal. Swelling, point tenderness, and pain exacerbated by weight-bearing are typical. A “dancer’s fracture” occurs at the base of the second metatarsal, while fractures distal to the tuberosity of the fifth metatarsal are called “Jones fractures.”
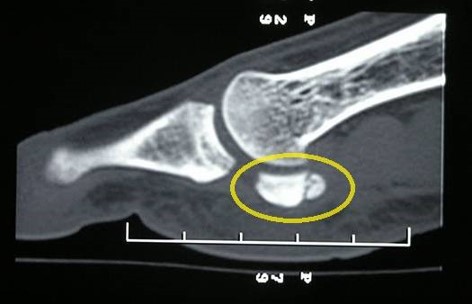
- Sesamoids: Stress fractures of the great toe sesamoids present with gradual unilateral plantar pain, commonly affecting the medial sesamoid (see Image. Sesamoid Stress Fracture).
Upper Extremity and Rib Stress Fractures
Upper extremity stress fractures are uncommon and most often occur in the ulna. Rib stress fractures, though rare, can be seen in specific groups:
- First rib: Seen in pitchers, basketball players, weightlifters, and ballet dancers.
- Ribs 4 to 9: Common in competitive rowers; posteromedial fractures can occur in golfers.
Etiology
Register For Free And Read The Full Article
Search engine and full access to all medical articles
10 free questions in your specialty
Free CME/CE Activities
Free daily question in your email
Save favorite articles to your dashboard
Emails offering discounts
Learn more about a Subscription to StatPearls Point-of-Care
Etiology
Mechanism of Stress Fractures
Stress fractures result from repeated submaximal loading. Traditionally, engineers compare these failures to fatigue fractures in materials like bridges; however, human bone undergoes constant remodeling, adding complexity to this analogy.[5][6] An imbalance between osteoclast and osteoblast activity triggers microdamage accumulation. High-risk stress fractures—tension-sided femoral neck, anterior tibial cortex, talar neck, and navicular—are prone to displacement or nonunion, possibly requiring surgical intervention. Low-risk fractures, including those in the fibula, posteromedial tibia, and metatarsal shafts, typically respond to activity modification.[7]
Types of Activities Associated with Stress Fractures
Different sports predispose athletes to specific stress fractures. Runners frequently sustain tibial and metatarsal fractures, whereas hurdlers have a higher patella fracture risk. Gymnasts and weightlifters are prone to spondylolysis, which results from repeated spinal hyperextension.[8] March fractures usually affect the second and third metatarsals, due to repetitive weight-bearing forces on relatively rigid segments.
Stress reactions and fractures result from repetitive microtrauma rather than acute injuries.[9] Stress fractures are common among runners and military recruits, often associated with changes in training intensity, footwear, or surfaces. Rapid changes in training programs, including increased distance, pace, volume, or cross-training without adequate time for adaptation, can contribute. Failure to follow intense training days with easy ones for recovery can also contribute to injury.[10] Therefore, prevention strategies focus on gradual activity increases, proper footwear, and sufficient recovery time.
Additionally, weekly distances exceeding 32 km (20 miles) significantly increase stress fracture risk for runners. These injuries typically arise during basic training or increased running and marching among military recruits. Female athletes and those with a prior history of stress fractures are at higher risk, especially when subjected to the same training regimens as male counterparts.[11][12] The higher incidence in females may reflect hormonal influences, lower bone density, or anatomical differences.[13]
Biomechanical and Nutritional Factors of Stress Fractures
Certain structural or gait abnormalities (eg, cavovarus foot alignment or narrow tibial width) may increase stress on specific bones. Contrasting earlier beliefs, ground reaction forces alone do not consistently predict stress fracture risk; rather, the vertical loading rate during heel strikes appears to correlate with injury incidence. Smaller tibial cross-sectional areas and lower muscle mass in the lower leg have also been linked to higher risk.[14]
Insufficient energy intake compromises recovery and bone health. In the female athlete triad (now often termed Relative Energy Deficiency in Sport, or RED-S), disordered eating, amenorrhea, and low bone mineral density can lead to recurrent fractures. Male endurance athletes with high training volumes and restricted caloric intake may experience decreased testosterone and subsequent osteopenia or osteoporosis. Vitamin D also appears critical: low levels correlate with higher stress fracture risk, and supplementation may prevent some fractures, especially in military recruits.[15]
Risk Factors for Stress Reaction and Fractures
The most common risk factor is a sudden increase in activity levels, with longitudinal studies showing that higher pretraining activity levels may confer some protection. Other risk factors for stress fractures include the following intrinsic and extrinsic elements:
- Intrinsic factors:
- Extrinsic factors:
Epidemiology
Stress fractures represent up to 20% of sports medicine clinic visits and appear commonly in athletes and military recruits.[16][17] In high school sports, they account for 0.8% of all injuries, with cross-country runners experiencing the highest incidence.[18] Overall, 40% of athletes will sustain a stress fracture at some point in their careers.[19] The lower leg (40.3%) and foot (34.9%) represent the majority of stress injuries in this group. Up to 16% of running injuries are stress fractures, with those exceeding 25 miles per week at higher risk. Among military members, repetitive training activities led to a stress fracture rate of 5.69 per 1,000 person-years between 2009 and 2012. Metatarsal stress fractures are prevalent, representing 25% of all stress fractures and 20% of sports medicine visits, with the second metatarsal being the most frequently affected due to its limited motion and structural characteristics. Approximately 78% of elite soccer-related stress fractures involve the fifth metatarsal.[20] Military recruits show even higher rates, especially among women, who develop stress fractures at a ratio of roughly 4:1 compared to men in similar training.
Stress fractures are predominantly seen in weight-bearing limbs. The most common stress fractures, in decreasing order of occurrence, include the tibia (23.6%), tarsal navicular (17.6%), metatarsals (16.2%), femur (6.6%), and pelvis (1.6%).[21] Medial tibial stress syndrome, or shin splints, is the earliest manifestation of stress injuries and represents a spectrum of medial tibial pain that may progress to a fracture if not addressed. The specific location of stress fractures often varies by sport. For example, navicular, tibia, and metatarsal fractures are common in track athletes, while tibia and fibula fractures are prevalent among distance runners. Dancers predominantly suffer from metatarsal fractures, and military recruits often experience fractures in the calcaneus and metatarsals. The ulna is the most frequently affected upper extremity bone.[22] Despite generally favorable healing, recurrence rates can approach 60%, emphasizing the need for comprehensive prevention strategies.[23]
Pathophysiology
Bone Remodeling Pathophysiologic Mechanisms
Stress injuries occur when a mismatch between the bone's innate strength and the mechanical load it endures is present, leading to a gradual weakening of the bone structure. This mismatch can result from 2 primary mechanisms: fatigue fractures, where abnormal stress is applied to healthy bone, and insufficiency fractures, where normal stress is exerted on a compromised bone, specifically at muscle insertion points where repetitive load and stress are highest.[9][24] Insufficiency fractures may sometimes be referred to as pathological fractures, though this term traditionally describes fractures arising from focal bony abnormalities.
In normal healthy bone, osteoblastic activity repairs microdamage caused by regular physical activity. A stress fracture occurs when osteoclastic resorption exceeds osteoblastic repair, causing structural weakness. According to Wolff's law, bone adapts to repetitive loads, but excessive loading can disrupt osteocyte signaling, which allows microdamage to accumulate.[17] When osteocyte signaling falters, bone repair mechanisms fail to keep pace. This imbalance leads to stress fractures because the typical 3- to 4-month bone remodeling cycle cannot handle chronic excessive stress.[25]
Biomechanic Pathophysiologic Mechanisms
Biomechanical factors also influence stress fracture development. Compression fractures often run parallel to the bone's axis on the concave side, whereas tension fractures lie perpendicular on the convex side.[26] Foot biomechanics, with longer or more plantarflexed metatarsals bearing a disproportionate load, can significantly impact fracture risk. Certain foot types (eg, cavovarus) increase stress on the lateral column and predispose individuals to fractures of the fourth and fifth metatarsals.[27][28] External factors, including training type, intensity, environmental conditions, and footwear, all further contribute to stress fracture risk.
Histopathology
Animal studies reveal that, at the cellular level, stress fractures involve irregular bone changes. Histologic studies of stress fractures show that repetitive stress triggers increased osteoclastic activity that surpasses the rate of osteoblastic activity and new bone formation. As a result, the bone weakens. After 2 weeks, woven bone develops islands of cartilage and active resorption cavities along the periosteal margin. By 4 weeks, remodeling begins at the periosteal surface and continues along the fracture plane into the medullary cavity. The formation of a periosteal hard callus is a hallmark of healing.[29][30]
History and Physical
Clinical History
Patients typically report a gradual, dull ache that worsens with weight-bearing and often follows recent spikes in training intensity or changes in terrain or footwear.[31] Pain initially occurs only during exercise but can progress to discomfort during daily tasks and may persist upon waking.[32] Evaluating the past 6 to 8 weeks of training (changes in frequency, duration, or intensity), biomechanics, and intrinsic risk factors (eg, age, body composition, female athlete triad, or prior stress fractures) is critical. Certain medications (eg, glucocorticoids, bisphosphonates) also elevate fracture risk. Extrinsic contributors include dietary deficiencies and structural abnormalities in foot or gait mechanics.[19][33]
Physical Examination
Focal tenderness over the affected area is common and may be accompanied by soft tissue swelling. Differentiating muscle injury or early stress reactions from a true stress fracture is critical: soft tissue tenderness usually indicates strain or early reaction, whereas bony tenderness strongly suggests a fracture. Certain anatomical sites, eg, the pelvis and sacrum, can be diagnostically challenging due to their subtle presentations.[23] Several clinical tests aid in diagnosis, including:
- One-leg hop test: This test helps distinguish medial tibial stress syndrome from tibial stress fractures. Patients with fractures often cannot hop without pain, especially on landing.
- Fulcrum test: The fulcrum test evaluates possible femoral shaft stress fractures. The examiner places an arm under the thigh and applies pressure to the knee; pain or apprehension indicates a positive result.
- Lumbar extension or single-leg hyperextension (Stork test): This test assesses spondylolysis but has limited sensitivity and specificity. Spondylolysis may be asymptomatic and found incidentally on imaging, while spondylolisthesis involves anterior displacement of the vertebral body due to an unhealed pars defect.[34][8]
A biomechanical evaluation is also important; for instance, a supinated foot increases forefoot loading and the risk of second metatarsal fractures. Pain localization through palpation and assessing joint motion can guide diagnosis, and patients may exhibit a limping gait when weight-bearing if the joint is involved.[35]
Evaluation
Plain Radiographs
Plain radiographs are typically the first imaging modality for suspected stress injuries because they are widely available, affordable, and involve low radiation exposure. However, they frequently appear normal early in the injury process, resulting in low sensitivity.[11] Subtle signs—such as periosteal elevation, cortical thickening, sclerosis, or a fracture line—often take 2 to 3 weeks to become visible. A "dreaded black line" may signal a high-risk fracture in areas like the tibia or femur.[36][37] Spondylolysis poses an additional diagnostic challenge, sometimes requiring 5 specialized views to visualize the pars interarticularis properly.[34] Even with multiple views, early lesions can be missed, so further imaging, particularly MRI, is warranted if clinical suspicion remains high despite normal radiographs.
Metatarsal stress fractures ("march fractures") require particular attention. Plain radiographs may initially be negative or show only subtle periosteal reactions or cortical blurring. The "gray cortex" sign—poorly defined cortical lucency—may indicate early stress fractures.[38] Over time, radiographic signs such as callus formation or cortical lucency may become apparent.[39]
Magnetic Resonance Imaging
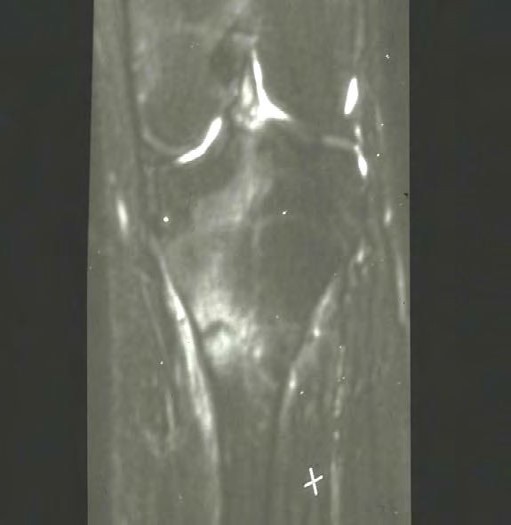
MRI is the most sensitive (80%–100%) and specific (100%) imaging modality for diagnosing stress injuries and is thus considered the gold standard.[22] Typical MRI findings include periosteal and bone marrow edema, fracture lines extending into the medullary canal, and adjacent soft tissue involvement (see Image. Stress Fracture on MRI). MRI offers the advantage of evaluating concurrent injuries to muscles, ligaments, or cartilage without radiation exposure.[40][41]
Computed Tomography
Computed tomography (CT) imaging provides detailed visualization of sclerosis, new bone formation, periosteal reactions, or fracture lines. CT is particularly useful in evaluating occult fractures and distinguishing between healing bone and fibrous unions. However, it involves greater radiation exposure and lower sensitivity than MRI.
Additional Imaging Studies
Other imaging techniques, such as single-photon emission computed tomography (SPECT) and 3-phase bone scans with technetium-99, are also used to detect early stress reactions not visible on plain radiographs.[2] Bone scintigraphy is moderately sensitive at 74%. These scans are highly sensitive but less specific, often showing increased uptake in areas of high bone turnover. Conditions like avascular necrosis, infections, or malignancies can also produce similar findings, limiting their diagnostic utility. These modalities are not typically used for follow-up imaging due to their lower specificity.
Laboratory Studies
Laboratory tests play a limited role in diagnosing stress fractures but are valuable in recurrent or frequent cases. Vitamin D deficiency (serum levels below 20 ng/mL) has been linked to higher stress fracture incidence.[40] In recurrent fracture scenarios, assessing thyroid-stimulating hormone, parathyroid hormone, and bone mineral density may be beneficial.[17]
Classification Systems
Stress fractures are broadly categorized into high-risk and low-risk injuries. Metatarsal stress fractures, for example, are classified as low-risk due to their generally favorable prognosis with activity modification and weight-bearing management.[24] Multiple imaging-based classification systems have been developed to define injury severity and prognosis more clearly.
Radiographic Grading System
The following 5-tiered grading system for stress fracture developed by Kaeding and Miller is associated with specific radiographic findings:
- Asymptomatic radiographic findings
- Pain with no fracture on imaging
- Nondisplaced fracture on imaging
- Displaced fracture on imaging
- Sclerotic nonunion on imaging [42]
Magnetic Resonance Imaging Grading System
Nattiv et al developed a classification for stress fractures in athletes, similar to the grading system suggested by Fredericson et al, involving the evaluation of bone marrow edema and periosteal reaction in bone stress injuries on MRI (see Image. T1 and T2 Images of Stress Fracture).[21][43] The following findings are associated with each grade:
- Grade 1: mild marrow edema or periosteal edema on fat-suppressed T2WI (but not on T1WI)
- Grade 2: moderate marrow edema or periosteal edema on fat-suppressed T2WI (but not on T1WI)
- Grade 3: severe marrow edema or periosteal edema on both fat-suppressed T2WI and T1WI, without a fracture line on T1WI or T2WI
- Grade 4: severe marrow edema or periosteal edema on both fat-suppressed T2WI and T1WI, with a fracture line on T1WI or T2WI (see Image. Grade 4 Stress Fracture)
Treatment / Management
The treatment of stress injuries depends on whether the lesion is a stress reaction or fracture, its anatomical location, and the potential for rehabilitation. Clinicians must identify fractures at risk for delayed union, nonunion, displacement, or intra-articular extension. General management principles include partial or nonweight-bearing for 2 to 6 weeks, followed by gradual activity resumption. Early detection is essential since prompt intervention facilitates quicker recovery.
Low-Risk Fracture Management
Low-risk stress fractures typically receive conservative treatment using a 2-phase approach. Low-risk locations include the posterior tibia, second to fourth metatarsals, femur, pubic rami, sacrum, and fibula. Phase 1 involves analgesia, modified weight-bearing, and cessation of inciting activities. Temporary immobilization is appropriate if ambulation is painful. Recommended alternative activities include water fitness, cycling, and elliptical training to preserve fitness and strength.[23][9][40] Phase 2 commences after a pain-free period and features a graduated return to activity supported by ongoing physical therapy. For instance, runners should initially resume running at a reduced pace and distance on alternating days. Patients gradually progress toward baseline intensity, frequency, and duration over several weeks. The length of each phase varies. A practical guideline is to match the duration of pain resolution with an equal duration of graduated return to activity. Footwear modifications and orthotics may benefit athletes with pronounced foot pronation or supination. Shoes should ideally provide adequate heel width, firm midsole support, and a straight last. Regular shoe replacement every 300 to 350 miles, along with gait analysis and running form adjustments, can further minimize reinjury risk.[44]
High-Risk Fracture Management
High-risk stress fractures occur at sites with poor vascular supply, maximal tensile loading, or a predisposition to nonunion.[21][45] These injuries require a high index of suspicion and can pose diagnostic challenges. High-risk locations include the femoral neck, anterior tibia, tarsal navicular, talus, sesamoids, and the first and fifth metatarsals. These fractures often fail conservative management and can cause significant morbidity due to the risk of displacement from tensile forces at muscular attachments, causing bony distraction.[45] Femoral neck fractures constitute a distinct subgroup. Magnetic resonance imaging is recommended due to low radiographic sensitivity. Superior (tension-sided) femoral neck stress fractures require surgical consultation, whereas inferior (compression-sided) fractures involving <50% bone width may initially receive conservative treatment with close monitoring. Increasing pain or fracture size necessitates orthopedic referral, and displacement requires immediate operative intervention to prevent femoral head avascular necrosis.[46]
Spondylolysis Management
Spondylolysis represents a unique stress injury, with limited clinical trial data guiding management.[8] Conservative treatment typically involves activity modification, core strengthening, and potentially bracing. Activity restriction ranges from 2 weeks to 6 months, depending on symptom resolution. The efficacy of bracing, while controversial, is supported by some evidence showing >80% pain-free return with rigid orthoses limiting lumbar extension, worn 23 hours daily for up to 6 months.[34][47] Persistent symptoms may necessitate surgical intervention, with several effective techniques described, though this is outside the scope of this review.(A1)
Nutritional Supplementation
Calcium and vitamin D supplementation may reduce stress fracture incidence, though evidence supporting faster healing is limited. A study of female United States Navy recruits found a 20% fracture rate reduction using daily supplements of 2000 mg of calcium and 800 IU of vitamin D.[48] Generalizability remains unclear, as other studies suggest increased fracture risk with supplementation.[12] Female athletes with delayed menarche, infrequent menstruation, or decreased bone mineral density warrant endocrine evaluation and targeted supplementation. Routine vitamin D and calcium supplementation should be restricted to athletes with documented deficiencies or repeated stress fractures. Evaluation for eating disorders, along with psychiatric and nutritional intervention, is recommended where indicated. Bisphosphonates show preliminary promise but require further research validation.(A1)
Bone Specific Management
Recommendations for the management of specific types of stress fractures include:
- Rib: Managed nonoperatively with rest, analgesics, and training adjustments to correct mechanics.
- Pelvis: Conservatively treated with rest, protected weight bearing, and gradual activity resumption.
- Femoral neck: Compression-sided fractures with less than 50% bone width involvement receive conservative treatment with nonweight-bearing and activity restrictions. Tension-sided or extensive compression fractures (>50% width) typically require percutaneous screw fixation.
- Femoral shaft: Usually managed conservatively with rest, modified weight-bearing, and activity restriction. Surgical fixation with intramedullary nailing is indicated for fracture displacement, low bone density, or age over 60.
- Patella: Treated conservatively with immobilization followed by progressive activity.
- Tibia: Conservatively managed with protected weight-bearing and activity modification. The presence of an anterior cortical "dreaded black line" typically necessitates surgical intervention with intramedullary nailing or plating based on patient-specific considerations. Medial tibial plateau fractures usually receive conservative treatment. Medial malleolar fractures may require operative intervention depending on ankle stability.
- Fibula: Conservative management includes rest, immobilization, and progressive activity resumption.
- Tarsals: Calcaneal stress fractures generally heal rapidly with conservative treatment. Navicular fractures carry high nonunion risk, requiring nonweight-bearing for up to 12 weeks, with surgical fixation indicated for completed fracture lines. Talus and medial cuneiform fractures often respond to conservative management.
- Metatarsals: Typically conservatively managed, with metatarsal padding as necessary. Dancer fractures (base of the second metatarsal) require nonweight-bearing immobilization. Fifth metatarsal fractures carry significant nonunion risk, often requiring immobilization and surgical management. Sesamoid fractures necessitate rest, immobilization, and offloading from offending activities.
Differential Diagnosis
The differential diagnosis for stress reactions and fractures is broad but can be refined based on anatomical location and clinical features. Conditions with similar presentations include:
- Bone contusion: Typically related to acute trauma rather than repetitive loading.
- Cellulitis: Presents with superficial skin erythema, warmth, and significant soft tissue swelling.
- Osteomyelitis/infection: Often accompanied by systemic symptoms (eg, fever and elevated inflammatory markers).
- Tendonitis/tendinopathy: This condition usually presents as pain localized along the tendon and worsens with specific tendon loading rather than bone palpation.
- Bursitis: Localized tenderness over bursae, with pain exacerbated by direct pressure, is typical in this condition.
- Degenerative changes/arthropathy: Pain is often associated with joint stiffness and limited motion and worsens with joint use rather than weight-bearing on bone.
- Exertional compartment syndrome: This condition is characterized by progressive, activity-induced muscle tightness relieved quickly after cessation.
- Acute compartment syndrome: Presents acutely after trauma with severe pain disproportionate to exam findings and neurovascular compromise.
- Neuropathic pain: This type of pain is typically sharp, burning, or electric in nature and has sensory abnormalities.
- Complex regional pain syndrome (CRPS): CRPS is associated with abnormal skin changes, autonomic dysfunction, and severe disproportionate pain.
- Radiculopathy: Pain radiates along a dermatome and worsens with spinal movements rather than localized bone stress.
- Nerve entrapment: Pain accompanied by numbness or tingling in specific nerve distributions.
- Arterial entrapment: This condition is characterized by exertional limb pain with vascular symptoms (pallor, reduced pulses) during activity.
- Coagulation disorders: These conditions usually present with spontaneous or easy bruising and often systemic bleeding issues.
- Avascular necrosis: Avascular necrosis often involves deep, dull joint pain unrelated to repetitive loading, frequently with risk factors such as corticosteroid use.
- Benign or malignant bone tumors (osteosarcoma, Ewing sarcoma, metastasis): Often show progressive night pain, unrelieved by rest, possible palpable mass, and abnormal imaging appearance.
Depending on anatomical location, nonmusculoskeletal conditions (eg, dermatologic, vascular, neurologic, genitourinary, reproductive, and gastrointestinal) may also be considered, including:
- Pelvic or femoral stress injuries may mimic reproductive or gastrointestinal disorders.
- Tibial stress injuries require differentiation from chronic exertional compartment syndrome (CECS) and popliteal artery entrapment syndrome.
Advanced imaging (particularly MRI) is valuable in distinguishing stress fractures from malignancies, osteomyelitis, and osteoid osteomas, with reported accuracy between 93% and 98%.[24]
Prognosis
The prognosis for patients with stress reactions or fractures largely depends on early recognition, injury severity, anatomical location, and adherence to appropriate management strategies. Patients diagnosed in the stress reaction stage—defined by bone marrow edema without cortical disruption—typically experience favorable outcomes with conservative measures, such as activity modification, offloading, and nutritional optimization. Recovery generally occurs within 6 to 8 weeks if mechanical stress is adequately reduced. For patients whose injuries progress to stress fractures, the prognosis varies significantly according to the fracture site and displacement severity.
Low-risk fractures, eg, those involving the tibia, fibula, or metatarsals, usually heal well with conservative care, including protected weight-bearing and a gradual return to activity. These injuries typically resolve within 6 to 12 weeks, with most patients regaining full function.[49] In contrast, high-risk fractures—including those involving the femoral neck, anterior tibial cortex, and navicular bone—have a greater risk of delayed union, nonunion, or progression to complete fractures if managed inadequately. Such injuries often require prolonged immobilization or surgical intervention. Poor prognostic indicators include ongoing mechanical loading, inadequate nutritional status, osteoporosis, and conditions such as relative energy deficiency in sport (RED-S).[50]
Overall, long-term outcomes are generally favorable with timely intervention. However, recurrence is common if underlying biomechanical issues or training errors remain unaddressed. Preventive strategies such as progressive training schedules, optimized footwear, sufficient calcium and vitamin D intake, and patient education on symptom recognition are essential for reducing recurrence risk. With early diagnosis and appropriate evidence-based management, most patients can fully recover and resume prior activity levels without significant long-term impairment.
Complications
Stress reactions and fractures, if not identified and managed promptly, can lead to acute and chronic complications affecting long-term function. Complication risks depend on injury severity, location, and treatment adequacy. An interprofessional approach addressing biomechanics, nutrition, and training practices is essential to minimize these risks and ensure optimal musculoskeletal recovery.
Acute Complications
Progression to complete fracture
One of the most significant risks of untreated or poorly managed stress reactions is the progression to a complete fracture. Continued mechanical loading on an already weakened bone can result in a full-thickness cortical break, necessitating prolonged immobilization or surgical intervention. High-risk sites, such as the femoral neck, anterior tibia, and navicular bone, are particularly prone to this complication.
Delayed union
Stress fractures that fail to heal within the expected timeframe (typically 6–12 weeks) may be classified as delayed unions. This can occur due to inadequate immobilization, premature return to activity, poor nutritional status, or underlying metabolic conditions. Delayed healing prolongs recovery and increases the likelihood of chronic pain and dysfunction.
Soft tissue injury
Persistent stress on the affected bone may also lead to compensatory overuse injuries in surrounding muscles, tendons, or ligaments. This includes conditions such as tendinopathy, plantar fasciitis, or muscle strains.
Chronic Complications
Nonunion
Nonunion occurs when a stress fracture fails to heal completely, often requiring surgical intervention, including bone grafting or internal fixation. This is more common in high-risk fractures, particularly in locations with limited vascular supply, such as the navicular and anterior tibia.
Chronic pain and functional limitations
Despite radiographic healing, persistent pain can occur due to incomplete bone remodeling, residual biomechanical abnormalities, or secondary soft tissue dysfunction. This may lead to chronic activity restrictions and reduced athletic performance.
Recurrent stress fractures
Inadequate rehabilitation, improper return-to-sport protocols, or failure to address underlying biomechanical and nutritional factors can result in recurrent stress fractures. Individuals with poor bone mineral density or those engaged in high-impact sports are particularly susceptible.
Joint degeneration and osteoarthritis
Recurrent stress fractures, particularly in weight-bearing joints, may accelerate cartilage wear and contribute to early-onset osteoarthritis. This is especially concerning in fractures involving the femoral neck or tibial plateau.
Postoperative and Rehabilitation Care
Nonoperative Rehabilitation
Postoperative and rehabilitation care for stress injuries or fractures depends on injury severity, anatomical location, and the type of intervention performed. Following a structured rehabilitation program can help achieve optimal outcomes, minimize recurrence risk, and allow safe resumption of preinjury activities. Key treatment goals include pain control, optimal bone healing, complication prevention, and a structured return to activity. Nonoperative management aims to promote bone healing, prevent progression to complete fractures, and facilitate a safe return to activity. Rehabilitation occurs in structured phases, advancing according to symptom resolution and radiographic healing evidence.
Acute phase (0-2 Weeks)
The initial phase focuses on pain management, mechanical offloading, and inflammation control. Activity modification is essential for stress reactions and low-risk fractures, with cessation of high-impact activities to prevent further bone stress. Immobilization may be required for high-risk stress fractures, such as those involving the anterior tibia, navicular, or femoral neck, necessitating a period of nonweight-bearing with crutches or a walking boot. Nonsteroidal anti-inflammatory drugs (NSAIDs) are used cautiously, as excessive use may impair bone remodeling.
Nutritional optimization plays a crucial role in early healing. Adequate calcium and vitamin D intake and addressing any underlying energy deficits are essential for bone repair. Patients with suspected relative energy deficiency in sport (RED-S) or osteopenia may require further dietary interventions.
Subacute phase (2-6 Weeks)
As pain subsides, gradual reintroduction of weight-bearing is initiated based on fracture location and healing progression. Low-risk stress fractures, such as those of the fibula or metatarsals, may transition to partial weight-bearing earlier, while high-risk fractures require more prolonged immobilization.
Physical therapy is introduced to maintain mobility and prevent muscular atrophy. Nonimpact exercises, such as swimming and cycling, help preserve cardiovascular fitness without compromising healing. Core and hip strengthening exercises are emphasized, particularly in cases where biomechanical deficiencies contribute to injury risk.
Progressive rehabilitation phase (6-12 Weeks)
Upon radiographic or clinical confirmation of healing, progressive weight-bearing is introduced. Patients are transitioned to full weight-bearing activities while avoiding high-impact loading. Strength training, proprioceptive exercises, and flexibility programs are implemented to restore neuromuscular control. Gait analysis may be performed to address any biomechanical abnormalities that contributed to injury onset.
Return-to-sport and prevention phase (12+ Weeks)
A gradual return-to-sport program is essential to minimize recurrence risk. Progressive impact loading, such as controlled jogging and plyometric drills, is introduced before full participation in high-impact sports. Footwear assessment and training modifications, including surface changes and workload periodization, help prevent reinjury.
Long-term monitoring is crucial for individuals with recurrent stress injuries or underlying bone health concerns. Education on symptom recognition and early intervention strategies remains a key component of preventing future stress injuries, ensuring sustained athletic performance and overall bone health.
Operative Management of a Stress Fracture
For patients requiring operative management of a stress fracture, a postoperative rehabilitation protocol is typically followed.
Immediate postoperative phase (0-2 Weeks)
For patients requiring surgical intervention, immediate postoperative care focuses on pain control, edema management, and surgical site protection. Nonsteroidal anti-inflammatory drugs (NSAIDs) should be used cautiously due to potential adverse effects on bone healing. Immobilization through casting, bracing, or internal fixation is often necessary, particularly for high-risk fractures such as those of the femoral neck, anterior tibia, or navicular bone. Weight-bearing restrictions are dictated by fracture location and healing potential, with non-weight-bearing or partial weight-bearing commonly required in the early phase.
Early rehabilitation phase (2-6 Weeks)
During this phase, progressive loading strategies are introduced to facilitate bone remodeling while preventing reinjury. For surgically managed fractures, radiographic or MRI assessment is often used to monitor healing progression before weight-bearing is advanced. Patients may transition from non-weight-bearing to partial weight-bearing using assistive devices, eg, crutches or a walking boot. Physical therapy is initiated with a focus on maintaining joint mobility, improving circulation, and preventing muscular atrophy through nonimpact strengthening exercises, such as isometric contractions and aquatic therapy.
Progressive loading and functional rehabilitation (6-12 Weeks)
Once radiographic evidence of bone healing is observed, gradual weight-bearing progression is introduced, emphasizing restoring gait mechanics and lower-extremity strength. Low-impact exercises, eg, stationary cycling or elliptical training, may be initiated before progressing to weight-bearing activities. Proprioceptive and neuromuscular training are incorporated to improve balance and prevent future injuries. Nutritional optimization, including sufficient calcium, vitamin D, and protein intake, remains essential to facilitate bone repair.
Return-to-sport and long-term monitoring (12+ Weeks)
A structured return-to-sport protocol is necessary to prevent recurrence. Progressive impact loading is introduced, beginning with walking, followed by jogging, and ultimately resuming full athletic activity. Biomechanical analysis, including gait assessment and footwear evaluation, may be performed to identify risk factors contributing to the initial injury. Strength deficits and muscular imbalances are addressed to minimize future stress injuries. Patients recovering from high-risk fractures require ongoing monitoring to assess for delayed healing or reinjury risk.
Consultations
Uncomplicated low-risk stress injuries can generally be managed without consultation of an orthopedic surgeon or sports medicine clinician. Low-risk stress injuries include pubic ramus, sacrum, ribs, proximal humerus or humeral shaft, posteromedial tibial shaft, fibula, and second through fourth metatarsal shafts. High-risk stress fractures should be managed in consultation with an orthopedic surgeon or sports medicine physician. High-risk injuries include the calcaneus, fifth metatarsal, second through the fourth metatarsal neck, sesamoid, talar neck, tarsal navicular, anterior tibial cortex, medial malleolus, femoral neck, femoral head, patella, and pars interarticularis of the lumbar spine.
Deterrence and Patient Education
Nearly all stress injuries result from overuse and insufficient recovery. Prevention strategies should emphasize appropriate biomechanics, gradual increases in training intensity and volume, proper footwear, and suitable training surfaces. Extrinsic factors, eg, optimizing calcium and vitamin D levels, maintaining a balanced diet, incorporating cross-training, and avoiding smoking, are relatively simple to address. Intrinsic factors, including physical conditioning, hormonal or menstrual disturbances, low bone density, and muscle mass deficits, can also be improved with targeted interventions. Nonmodifiable intrinsic factors such as female sex, genu valgum, and leg-length discrepancies should be acknowledged and accommodated when planning training programs.[2]
Pearls and Other Issues
Key facts regarding stress reaction and fractures that should be kept in mind include:
- Stress fractures commonly affect athletes and military recruits.
- Low-risk fractures typically respond well to conservative management.
- High-risk locations demand early imaging and possible surgical consultation.
- Recurrent fractures warrant evaluation for metabolic, nutritional, or biomechanical contributors.
- Early detection and patient education markedly reduce morbidity and expedite return to sports.
Enhancing Healthcare Team Outcomes
Managing stress reactions and fractures requires a coordinated, interprofessional approach to ensure optimal patient outcomes, safety, and team performance. Physicians and advanced practitioners play a critical role in diagnosing these injuries and establishing individualized treatment plans, often incorporating imaging and biomechanical assessments to identify contributing factors. Physical therapists and athletic trainers oversee rehabilitation, focusing on restoring strength, correcting movement patterns, and implementing gait training to prevent reinjury. Nurses facilitate care coordination by educating patients on proper recovery techniques, reinforcing adherence to treatment protocols, and ensuring that all clinicians remain aligned in their approach. Pharmacists contribute by managing pain and anti-inflammatory medication regimens, ensuring appropriate use while minimizing risks such as gastrointestinal or renal complications. Sports nutritionists further enhance recovery by addressing dietary deficiencies and energy imbalances, particularly in cases involving the female athlete triad, where inadequate nutrition, menstrual dysfunction, and low bone density contribute to stress injuries.
Effective interprofessional communication is essential to streamline care, prevent misinformation, and encourage patient adherence to treatment recommendations. Regular team meetings, shared electronic health records, and direct communication between clinicians support seamless coordination. Gynecologists and sports medicine specialists may provide additional expertise, particularly when hormonal factors influence bone health. Patient education remains a shared responsibility across all disciplines, ensuring individuals understand injury prevention strategies, proper stretching techniques, and the benefits of supportive devices like arch supports. A unified message from the healthcare team reinforces the importance of gradual return-to-activity protocols, reducing the risk of recurrence. Since stress injuries have a high recurrence rate, continued monitoring and long-term preventive strategies are essential. By working collaboratively, healthcare professionals optimize recovery, enhance patient safety, and improve overall team performance in managing stress reactions and fractures.
Media
(Click Image to Enlarge)
(Click Image to Enlarge)
(Click Image to Enlarge)
(Click Video to Play)
T1 and T2 Images of Stress Fracture. MRI showing the changes in T1 and T2 images of a stress fracture.
Contributed by T May, DO
(Click Image to Enlarge)
(Click Image to Enlarge)
References
Matheson GO, Clement DB, McKenzie DC, Taunton JE, Lloyd-Smith DR, MacIntyre JG. Stress fractures in athletes. A study of 320 cases. The American journal of sports medicine. 1987 Jan-Feb:15(1):46-58 [PubMed PMID: 3812860]
Level 3 (low-level) evidenceMcCormick F, Nwachukwu BU, Provencher MT. Stress fractures in runners. Clinics in sports medicine. 2012 Apr:31(2):291-306. doi: 10.1016/j.csm.2011.09.012. Epub [PubMed PMID: 22341018]
Teichtahl AJ, Wluka AE, Wijethilake P, Wang Y, Ghasem-Zadeh A, Cicuttini FM. Wolff's law in action: a mechanism for early knee osteoarthritis. Arthritis research & therapy. 2015 Sep 1:17(1):207. doi: 10.1186/s13075-015-0738-7. Epub 2015 Sep 1 [PubMed PMID: 26324398]
Patel DR. Stress fractures: diagnosis and management in the primary care setting. Pediatric clinics of North America. 2010 Jun:57(3):819-27. doi: 10.1016/j.pcl.2010.03.004. Epub [PubMed PMID: 20538158]
Abe K, Hashiguchi H, Sonoki K, Iwashita S, Takai S. Tarsal Navicular Stress Fracture in a Young Athlete: A Case Report. Journal of Nippon Medical School = Nippon Ika Daigaku zasshi. 2019:86(2):122-125. doi: 10.1272/jnms.JNMS.2019_86-208. Epub [PubMed PMID: 31130563]
Level 3 (low-level) evidenceStein CJ, Sugimoto D, Slick NR, Lanois CJ, Dahlberg BW, Zwicker RL, Micheli LJ. Hallux sesamoid fractures in young athletes. The Physician and sportsmedicine. 2019 Nov:47(4):441-447. doi: 10.1080/00913847.2019.1622246. Epub 2019 Jun 5 [PubMed PMID: 31109214]
Bärtschi N, Scheibler A, Schweizer A. Symptomatic epiphyseal sprains and stress fractures of the finger phalanges in adolescent sport climbers. Hand surgery & rehabilitation. 2019 Sep:38(4):251-256. doi: 10.1016/j.hansur.2019.05.003. Epub 2019 May 16 [PubMed PMID: 31103479]
Gagnet P, Kern K, Andrews K, Elgafy H, Ebraheim N. Spondylolysis and spondylolisthesis: A review of the literature. Journal of orthopaedics. 2018 Jun:15(2):404-407. doi: 10.1016/j.jor.2018.03.008. Epub 2018 Mar 17 [PubMed PMID: 29881164]
Sanderlin BW, Raspa RF. Common stress fractures. American family physician. 2003 Oct 15:68(8):1527-32 [PubMed PMID: 14596439]
Schilcher J, Bernhardsson M, Aspenberg P. Chronic anterior tibial stress fractures in athletes: No crack but intense remodeling. Scandinavian journal of medicine & science in sports. 2019 Oct:29(10):1521-1528. doi: 10.1111/sms.13466. Epub 2019 Jun 2 [PubMed PMID: 31102562]
Matcuk GR Jr, Mahanty SR, Skalski MR, Patel DB, White EA, Gottsegen CJ. Stress fractures: pathophysiology, clinical presentation, imaging features, and treatment options. Emergency radiology. 2016 Aug:23(4):365-75. doi: 10.1007/s10140-016-1390-5. Epub 2016 Mar 22 [PubMed PMID: 27002328]
Wright AA, Taylor JB, Ford KR, Siska L, Smoliga JM. Risk factors associated with lower extremity stress fractures in runners: a systematic review with meta-analysis. British journal of sports medicine. 2015 Dec:49(23):1517-23. doi: 10.1136/bjsports-2015-094828. Epub 2015 Jul 17 [PubMed PMID: 26582192]
Level 1 (high-level) evidenceFredericson M, Kent K. Normalization of bone density in a previously amenorrheic runner with osteoporosis. Medicine and science in sports and exercise. 2005 Sep:37(9):1481-6 [PubMed PMID: 16177598]
Level 3 (low-level) evidenceZadpoor AA, Nikooyan AA. The relationship between lower-extremity stress fractures and the ground reaction force: a systematic review. Clinical biomechanics (Bristol, Avon). 2011 Jan:26(1):23-8. doi: 10.1016/j.clinbiomech.2010.08.005. Epub 2010 Sep 16 [PubMed PMID: 20846765]
Level 2 (mid-level) evidenceMiller TL, Best TM. Taking a holistic approach to managing difficult stress fractures. Journal of orthopaedic surgery and research. 2016 Sep 9:11(1):98. doi: 10.1186/s13018-016-0431-9. Epub 2016 Sep 9 [PubMed PMID: 27608681]
Yang J, Tibbetts AS, Covassin T, Cheng G, Nayar S, Heiden E. Epidemiology of overuse and acute injuries among competitive collegiate athletes. Journal of athletic training. 2012 Mar-Apr:47(2):198-204 [PubMed PMID: 22488286]
Level 2 (mid-level) evidenceMoreira CA, Bilezikian JP. Stress Fractures: Concepts and Therapeutics. The Journal of clinical endocrinology and metabolism. 2017 Feb 1:102(2):525-534. doi: 10.1210/jc.2016-2720. Epub [PubMed PMID: 27732325]
Changstrom BG, Brou L, Khodaee M, Braund C, Comstock RD. Epidemiology of stress fracture injuries among US high school athletes, 2005-2006 through 2012-2013. The American journal of sports medicine. 2015 Jan:43(1):26-33. doi: 10.1177/0363546514562739. Epub 2014 Dec 5 [PubMed PMID: 25480834]
Abbott A, Bird ML, Wild E, Brown SM, Stewart G, Mulcahey MK. Part I: epidemiology and risk factors for stress fractures in female athletes. The Physician and sportsmedicine. 2020 Feb:48(1):17-24. doi: 10.1080/00913847.2019.1632158. Epub 2019 Jul 11 [PubMed PMID: 31213104]
Ekstrand J, Torstveit MK. Stress fractures in elite male football players. Scandinavian journal of medicine & science in sports. 2012 Jun:22(3):341-6. doi: 10.1111/j.1600-0838.2010.01171.x. Epub 2010 Aug 30 [PubMed PMID: 20807388]
Kahanov L, Eberman LE, Games KE, Wasik M. Diagnosis, treatment, and rehabilitation of stress fractures in the lower extremity in runners. Open access journal of sports medicine. 2015:6():87-95. doi: 10.2147/OAJSM.S39512. Epub 2015 Mar 27 [PubMed PMID: 25848327]
Fredericson M, Jennings F, Beaulieu C, Matheson GO. Stress fractures in athletes. Topics in magnetic resonance imaging : TMRI. 2006 Oct:17(5):309-25 [PubMed PMID: 17414993]
Patel DS, Roth M, Kapil N. Stress fractures: diagnosis, treatment, and prevention. American family physician. 2011 Jan 1:83(1):39-46 [PubMed PMID: 21888126]
Mandell JC, Khurana B, Smith SE. Stress fractures of the foot and ankle, part 2: site-specific etiology, imaging, and treatment, and differential diagnosis. Skeletal radiology. 2017 Sep:46(9):1165-1186. doi: 10.1007/s00256-017-2632-7. Epub 2017 Mar 25 [PubMed PMID: 28343329]
Denay KL. Stress Fractures. Current sports medicine reports. 2017 Jan/Feb:16(1):7-8. doi: 10.1249/JSR.0000000000000320. Epub [PubMed PMID: 28067732]
Saunier J, Chapurlat R. Stress fracture in athletes. Joint bone spine. 2018 May:85(3):307-310. doi: 10.1016/j.jbspin.2017.04.013. Epub 2017 May 13 [PubMed PMID: 28512006]
Rongstad KM, Tueting J, Rongstad M, Garrels K, Meis R. Fourth metatarsal base stress fractures in athletes: a case series. Foot & ankle international. 2013 Jul:34(7):962-8. doi: 10.1177/1071100713475613. Epub 2013 Feb 5 [PubMed PMID: 23386752]
Level 2 (mid-level) evidenceSaxena A, Krisdakumtorn T, Erickson S. Proximal fourth metatarsal injuries in athletes: similarity to proximal fifth metatarsal injury. Foot & ankle international. 2001 Jul:22(7):603-8 [PubMed PMID: 11503989]
Level 3 (low-level) evidenceUthgenannt BA, Kramer MH, Hwu JA, Wopenka B, Silva MJ. Skeletal self-repair: stress fracture healing by rapid formation and densification of woven bone. Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research. 2007 Oct:22(10):1548-56 [PubMed PMID: 17576168]
Level 3 (low-level) evidenceKidd LJ, Stephens AS, Kuliwaba JS, Fazzalari NL, Wu AC, Forwood MR. Temporal pattern of gene expression and histology of stress fracture healing. Bone. 2010 Feb:46(2):369-78. doi: 10.1016/j.bone.2009.10.009. Epub 2009 Oct 15 [PubMed PMID: 19836476]
Level 3 (low-level) evidenceShi E, Oloff LM, Todd NW. Stress Injuries in the Athlete. Clinics in podiatric medicine and surgery. 2023 Jan:40(1):181-191. doi: 10.1016/j.cpm.2022.07.012. Epub 2022 Oct 13 [PubMed PMID: 36368842]
Welck MJ, Hayes T, Pastides P, Khan W, Rudge B. Stress fractures of the foot and ankle. Injury. 2017 Aug:48(8):1722-1726. doi: 10.1016/j.injury.2015.06.015. Epub 2015 Sep 15 [PubMed PMID: 26412591]
West TA, Pollard JD, Chandra M, Hui RL, Weintraub MR, King CM, Grimsrud CD, Lo JC. The Epidemiology of Metatarsal Fractures Among Older Females With Bisphosphonate Exposure. The Journal of foot and ankle surgery : official publication of the American College of Foot and Ankle Surgeons. 2020 Mar-Apr:59(2):269-273. doi: 10.1053/j.jfas.2019.02.008. Epub [PubMed PMID: 32130989]
Lawrence KJ, Elser T, Stromberg R. Lumbar spondylolysis in the adolescent athlete. Physical therapy in sport : official journal of the Association of Chartered Physiotherapists in Sports Medicine. 2016 Jul:20():56-60. doi: 10.1016/j.ptsp.2016.04.003. Epub 2016 Apr 13 [PubMed PMID: 27234265]
Dixon S, Nunns M, House C, Rice H, Mostazir M, Stiles V, Davey T, Fallowfield J, Allsopp A. Prospective study of biomechanical risk factors for second and third metatarsal stress fractures in military recruits. Journal of science and medicine in sport. 2019 Feb:22(2):135-139. doi: 10.1016/j.jsams.2018.06.015. Epub 2018 Jul 26 [PubMed PMID: 30057365]
Kola S, Granville M, Jacobson RE. The Association of Iliac and Sacral Insufficiency Fractures and Implications for Treatment: The Role of Bone Scans in Three Different Cases. Cureus. 2019 Jan 10:11(1):e3861. doi: 10.7759/cureus.3861. Epub 2019 Jan 10 [PubMed PMID: 30899612]
Level 3 (low-level) evidenceGmachowska AM, Żabicka M, Pacho R, Pacho S, Majek A, Feldman B. Tibial stress injuries - location, severity, and classification in magnetic resonance imaging examination. Polish journal of radiology. 2018:83():e471-e481. doi: 10.5114/pjr.2018.80218. Epub 2018 Nov 5 [PubMed PMID: 30655927]
Mulligan ME. The "gray cortex ": an early sign of stress fracture. Skeletal radiology. 1995 Apr:24(3):201-3 [PubMed PMID: 7610412]
Level 3 (low-level) evidenceBurr DB, Forwood MR, Fyhrie DP, Martin RB, Schaffler MB, Turner CH. Bone microdamage and skeletal fragility in osteoporotic and stress fractures. Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research. 1997 Jan:12(1):6-15 [PubMed PMID: 9240720]
Pegrum J, Dixit V, Padhiar N, Nugent I. The pathophysiology, diagnosis, and management of foot stress fractures. The Physician and sportsmedicine. 2014 Nov:42(4):87-99. doi: 10.3810/psm.2014.11.2095. Epub [PubMed PMID: 25419892]
Marshall RA, Mandell JC, Weaver MJ, Ferrone M, Sodickson A, Khurana B. Imaging Features and Management of Stress, Atypical, and Pathologic Fractures. Radiographics : a review publication of the Radiological Society of North America, Inc. 2018 Nov-Dec:38(7):2173-2192. doi: 10.1148/rg.2018180073. Epub [PubMed PMID: 30422769]
Kaeding CC, Miller T. The comprehensive description of stress fractures: a new classification system. The Journal of bone and joint surgery. American volume. 2013 Jul 3:95(13):1214-20. doi: 10.2106/JBJS.L.00890. Epub [PubMed PMID: 23824390]
Nattiv A, Kennedy G, Barrack MT, Abdelkerim A, Goolsby MA, Arends JC, Seeger LL. Correlation of MRI grading of bone stress injuries with clinical risk factors and return to play: a 5-year prospective study in collegiate track and field athletes. The American journal of sports medicine. 2013 Aug:41(8):1930-41. doi: 10.1177/0363546513490645. Epub 2013 Jul 3 [PubMed PMID: 23825184]
Cook SD, Brinker MR, Poche M. Running shoes. Their relationship to running injuries. Sports medicine (Auckland, N.Z.). 1990 Jul:10(1):1-8 [PubMed PMID: 2197696]
McInnis KC, Ramey LN. High-Risk Stress Fractures: Diagnosis and Management. PM & R : the journal of injury, function, and rehabilitation. 2016 Mar:8(3 Suppl):S113-24. doi: 10.1016/j.pmrj.2015.09.019. Epub [PubMed PMID: 26972260]
DeFroda SF, Cameron KL, Posner M, Kriz PK, Owens BD. Bone Stress Injuries in the Military: Diagnosis, Management, and Prevention. American journal of orthopedics (Belle Mead, N.J.). 2017 Jul/Aug:46(4):176-183 [PubMed PMID: 28856344]
Overley SC, McAnany SJ, Andelman S, Kim J, Merrill RK, Cho SK, Qureshi SA, Hecht AC. Return to Play in Adolescent Athletes With Symptomatic Spondylolysis Without Listhesis: A Meta-Analysis. Global spine journal. 2018 Apr:8(2):190-197. doi: 10.1177/2192568217734520. Epub 2017 Oct 5 [PubMed PMID: 29662750]
Level 1 (high-level) evidenceLappe J, Cullen D, Haynatzki G, Recker R, Ahlf R, Thompson K. Calcium and vitamin d supplementation decreases incidence of stress fractures in female navy recruits. Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research. 2008 May:23(5):741-9. doi: 10.1359/jbmr.080102. Epub [PubMed PMID: 18433305]
Level 1 (high-level) evidenceBoden BP, Osbahr DC, Jimenez C. Low-risk stress fractures. The American journal of sports medicine. 2001 Jan-Feb:29(1):100-11 [PubMed PMID: 11206247]
Boden BP, Osbahr DC. High-risk stress fractures: evaluation and treatment. The Journal of the American Academy of Orthopaedic Surgeons. 2000 Nov-Dec:8(6):344-53 [PubMed PMID: 11104398]